Phase II Reactions - The Cleanup Crew
Phase II reactions attach endogenous polar molecules to a drug or its Phase I metabolite. This conjugation step drastically increases water solubility, preparing the compound for elimination.
- Primary Goal: ↑ Polarity & water solubility for excretion.
- Major Pathways:
- Glucuronidation (most common, uses UDP-glucuronosyltransferase)
- Acetylation (e.g., Isoniazid, Hydralazine)
- Sulfation (e.g., Acetaminophen)
- 📌 Mnemonic: GAS (Glucuronidation, Acetylation, Sulfation).
⭐ High-Yield: Genetic polymorphism in N-acetyltransferase (NAT) leads to "slow acetylators" vs. "fast acetylators." Slow acetylators have ↑ risk of drug toxicity (e.g., drug-induced lupus from hydralazine, isoniazid-induced neuropathy).
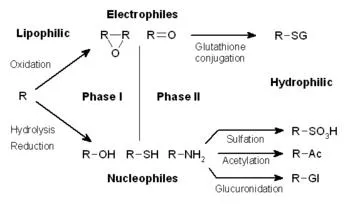
Conjugation Pathways - The Magnificent Six
Phase II reactions attach endogenous polar groups to drugs, making them more water-soluble for excretion. This process generally inactivates the drug.
- Glucuronidation
- Enzyme: UGT (UDP-glucuronosyltransferase)
- Cofactor: UDP-glucuronic acid
- Most common pathway; deficient in neonates (e.g., Gray Baby Syndrome).
- Drugs: Morphine, Acetaminophen, Lorazepam.
- Sulfation
- Enzyme: SULT (Sulfotransferase)
- Cofactor: PAPS
- Drugs: Acetaminophen, Methyldopa.
- Acetylation
- Enzyme: NAT (N-acetyltransferase)
- Cofactor: Acetyl-CoA
- Drugs: Sulfonamides, Hydralazine, Isoniazid, Procainamide (📌 SHIP).
- Glutathione Conjugation
- Enzyme: GST (Glutathione-S-transferase)
- Cofactor: Glutathione (GSH)
- Neutralizes reactive metabolites like NAPQI from acetaminophen.
- Glycine Conjugation
- Metabolizes salicylates.
- Methylation
- Enzyme: TPMT, COMT
- Cofactor: SAM
- Drugs: Azathioprine, 6-Mercaptopurine.
⭐ Slow vs. Fast Acetylators: Genetic polymorphism in NAT2 is a classic exam topic. Slow acetylators have ↑ risk of drug-induced lupus (e.g., Hydralazine, Procainamide) and peripheral neuropathy (Isoniazid).
Clinical Correlations - When Genes Stumble
-
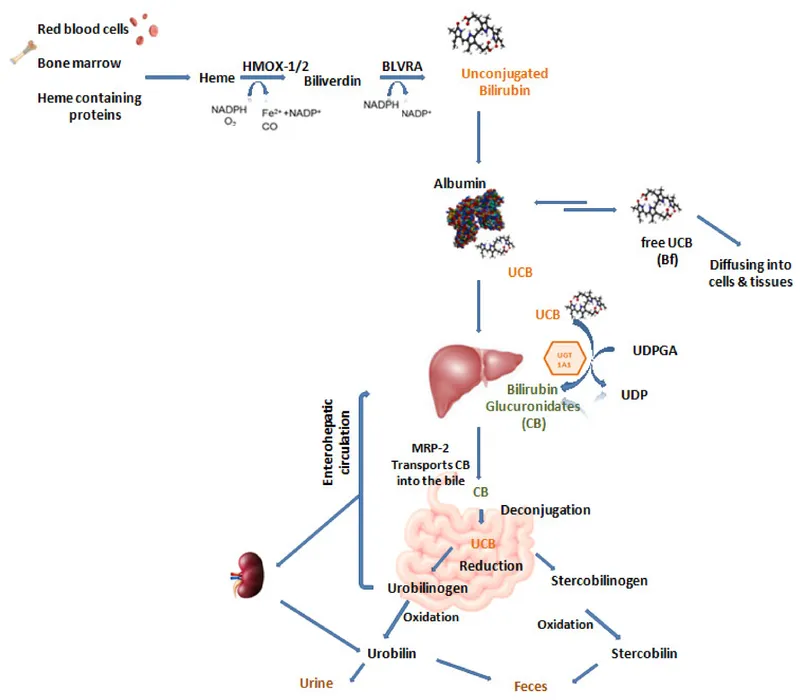
UDP-Glucuronosyltransferase (UGT) Deficiency: Affects bilirubin & drug conjugation.
- Gilbert's Syndrome: Mildly ↓ UGT activity. Benign unconjugated hyperbilirubinemia, provoked by stress or illness.
- Crigler-Najjar, Type I: Absent UGT. Severe jaundice, kernicterus; fatal without liver transplant.
- Crigler-Najjar, Type II: Markedly ↓ UGT activity. Responds to phenobarbital (induces UGT).
- Gray Baby Syndrome: Neonatal UGT immaturity causes toxic chloramphenicol accumulation.
-
N-acetyltransferase (NAT) Polymorphism:
- Slow Acetylators: ↑ risk for drug toxicity.
- Isoniazid: Peripheral neuropathy.
- Hydralazine, Procainamide, Isoniazid: Drug-induced lupus. 📌 SHIP happens.
- Fast Acetylators: May need higher doses of drugs like isoniazid.
- Slow Acetylators: ↑ risk for drug toxicity.
⭐ Slow acetylators are at increased risk for drug-induced lupus erythematosus (DILE) from hydralazine, procainamide, and isoniazid.
High-Yield Points - ⚡ Biggest Takeaways
- Phase II reactions make drugs polar and water-soluble for renal excretion by adding endogenous substrates.
- Key pathways: Glucuronidation (most common), Sulfation, Acetylation, and Glutathione conjugation.
- Genetic polymorphism of N-acetyltransferase (NAT) creates slow/fast acetylators, affecting toxicity of drugs like isoniazid.
- Neonatal UGT deficiency impairs drug/bilirubin conjugation, leading to jaundice and toxicity.
- Glutathione (GSH) depletion is the mechanism of acetaminophen hepatotoxicity; treated with N-acetylcysteine (NAC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

