Drug Distribution - Where'd That Drug Go?
- Volume of Distribution (Vd): Theoretical fluid volume that would be required to contain the amount of drug present in the body at the same concentration as in the plasma.
- Formula: $Vd = \frac{\text{Amount of drug in body}}{\text{Plasma drug concentration}}$
- Low Vd: Drug is confined to plasma (large, charged, protein-bound).
- High Vd: Drug is widely distributed in tissues (small, lipophilic, unbound).
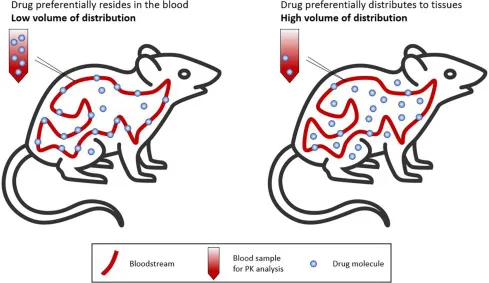
- Plasma Protein Binding:
- Primarily to albumin.
- Bound drug is inactive; only free drug exerts effects.
⭐ In states of hypoalbuminemia (e.g., liver disease, nephrotic syndrome), decreased protein binding leads to higher levels of free drug, increasing the risk of toxicity.
Plasma Protein Binding - The Clingy Molecules
- Drugs exist in two forms in plasma: bound and unbound. This binding is reversible.
- Only the unbound (free) fraction is pharmacologically active, can cross membranes, be distributed to tissues, get metabolized, and be excreted.
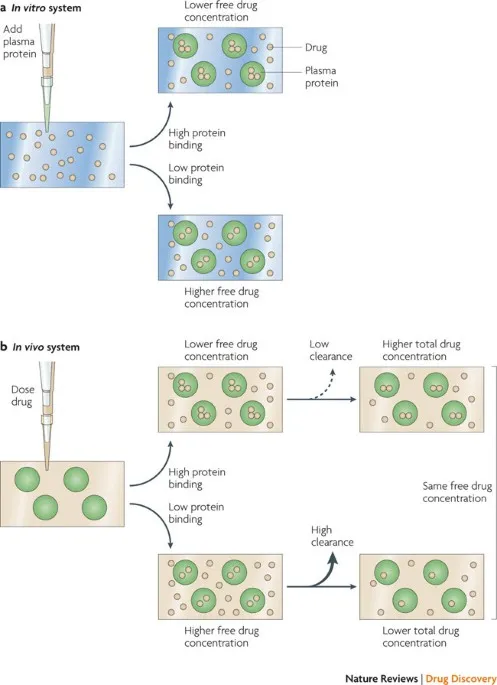
| Feature | Bound Drug | Unbound (Free) Drug |
|---|---|---|
| Activity | Inactive (sequestered) | Active |
| Distribution | Stays in plasma | Distributes to tissues |
| Metabolism | Not metabolized | Metabolized |
| Excretion | Not excreted | Excreted |
- **Albumin:** Binds acidic drugs (e.g., Warfarin, NSAIDs).
- **α₁-acid glycoprotein:** Binds basic drugs (e.g., Lidocaine, Propranolol).
⭐ Drug Displacement: When two drugs compete for the same binding site, one can displace the other. A highly bound drug like Warfarin can be displaced by sulfonamides, ↑ its free concentration and leading to bleeding risk.
- High protein binding restricts the drug to the vascular compartment, resulting in a low apparent Volume of Distribution ($V_d$).
Volume of Distribution (Vd) - High vs. Low Stakes
- Definition: The theoretical fluid volume required to contain the total amount of administered drug at the same concentration that it is in the plasma.
- Formula: $Vd = \frac{\text{Amount of drug in body}}{\text{Plasma drug concentration}}$
| Characteristic | Low Vd | High Vd |
|---|---|---|
| Distribution | Confined to plasma/ECF | Sequestered in tissues |
| Size | Large, charged molecules | Small, uncharged molecules |
| Binding | ↑ Plasma protein binding | ↑ Tissue protein binding |
| Solubility | Hydrophilic | Lipophilic |
| Example | Heparin, Warfarin | Chloroquine, Propofol |
Special Barriers - No Entry Zones
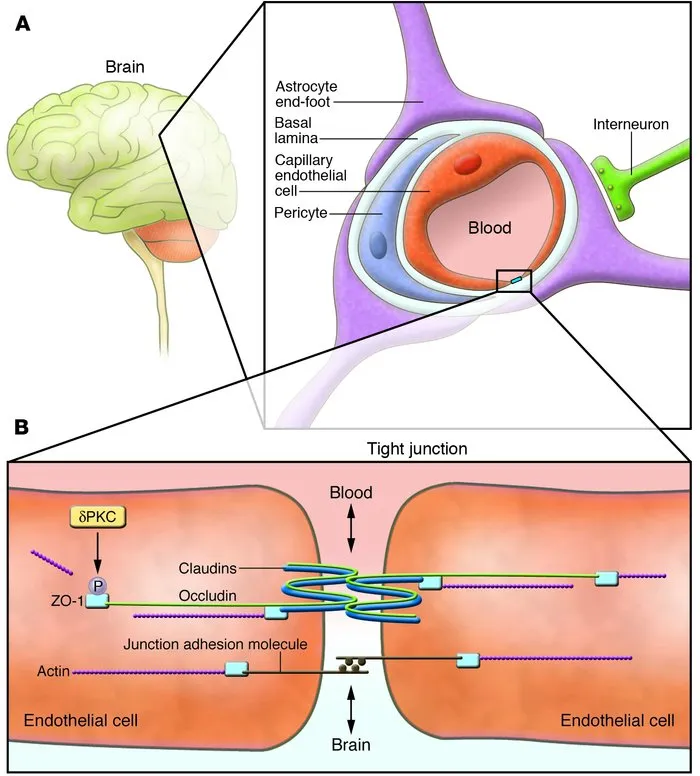
-
Blood-Brain Barrier (BBB): Restricts CNS entry.
- Formed by endothelial tight junctions & astrocyte feet.
- Permeable to lipid-soluble, non-ionized, small drugs.
- P-glycoprotein (MDR1) efflux pumps actively remove drugs.
- Inflammation (e.g., meningitis) can ↑ BBB permeability.
-
Placental Barrier:
- Semi-permeable; most drugs cross to some extent, posing fetal risk (teratogenicity).
- Lipid-soluble drugs cross more readily.
⭐ Some brain areas lack a BBB (circumventricular organs), like the area postrema (chemoreceptor trigger zone) & posterior pituitary. This allows for monitoring of systemic signals.
High-Yield Points - ⚡ Biggest Takeaways
- Volume of distribution (Vd): High Vd indicates extensive tissue distribution; low Vd suggests confinement to plasma.
- Only unbound (free) drug is pharmacologically active, can be metabolized, and can be excreted.
- Acidic drugs primarily bind to albumin; basic drugs bind to α1-acid glycoprotein.
- Displacement of highly protein-bound drugs (e.g., warfarin) ↑ free drug levels, risking toxicity.
- Lipid solubility is a key determinant for crossing the blood-brain barrier and placenta.
- Redistribution terminates the action of lipophilic drugs like propofol.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

