Mechanism of Action - Taking Out the B-Team
- Primary Target: CD20 antigen, a protein found on the surface of most B-lymphocytes, from pre-B-cells to mature B-cells.
- Antibody Binding: Monoclonal antibodies (e.g., Rituximab) bind specifically to the CD20 molecule.
- B-Cell Depletion: This binding triggers the destruction of the B-cell through several immune mechanisms:
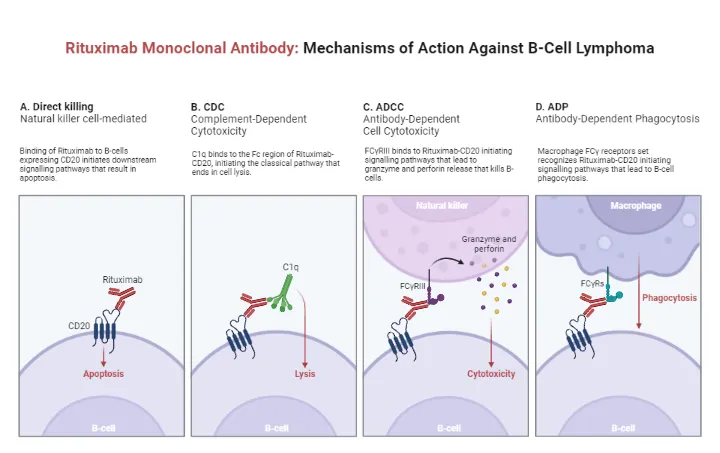
⭐ Exam Favorite: CD20 is NOT expressed on hematopoietic stem cells or mature plasma cells. This means that while mature B-cells are depleted, the body can still regenerate new B-cells and maintain long-term antibody levels from existing plasma cells.
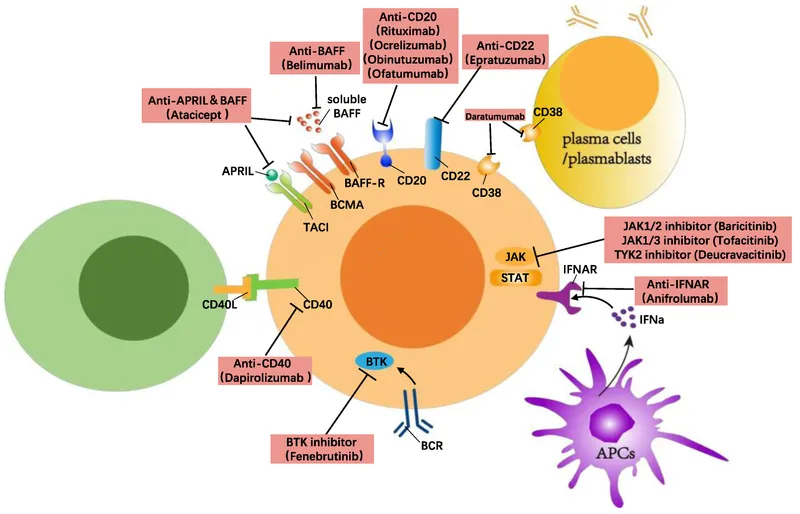
The '-mabs' - Rogues' Gallery & Indications
-
Rituximab, Ocrelizumab, Ofatumumab
- Target: CD20 on B-cells.
- Mechanism: Triggers complement-dependent cytotoxicity (CDC) and antibody-dependent cell-mediated cytotoxicity (ADCC), leading to B-cell apoptosis.
- Indications:
- Rituximab: B-cell non-Hodgkin lymphoma (NHL), chronic lymphocytic leukemia (CLL), rheumatoid arthritis (RA), granulomatosis with polyangiitis (GPA).
- Ocrelizumab: Primary progressive & relapsing multiple sclerosis (MS).
- Ofatumumab: Relapsing MS.
-
Belimumab
- Target: B-Lymphocyte Stimulator (BLyS), also known as BAFF.
- Mechanism: Inhibits BLyS, preventing B-cell survival and differentiation into plasma cells.
- Indication: Systemic Lupus Erythematosus (SLE).
⭐ High-Yield: Rituximab carries a black box warning for reactivation of the JC virus, potentially leading to Progressive Multifocal Leukoencephalopathy (PML), a severe demyelinating disease of the CNS.
Adverse Effects - When B-Gones Go Bad
-
Infusion-Related Reactions (IRRs)
- Often cytokine-release syndrome: fever, chills, rigors, hypotension, bronchospasm.
- Occur within 30-120 mins of first infusion.
- Management: Pre-medicate with antihistamines, acetaminophen, and glucocorticoids. Slow or stop infusion.
-
Infections
- ⚠️ Increased risk due to B-cell depletion and subsequent hypogammaglobulinemia.
- Hepatitis B reactivation: Screen all patients for HBsAg and anti-HBc before starting.
-
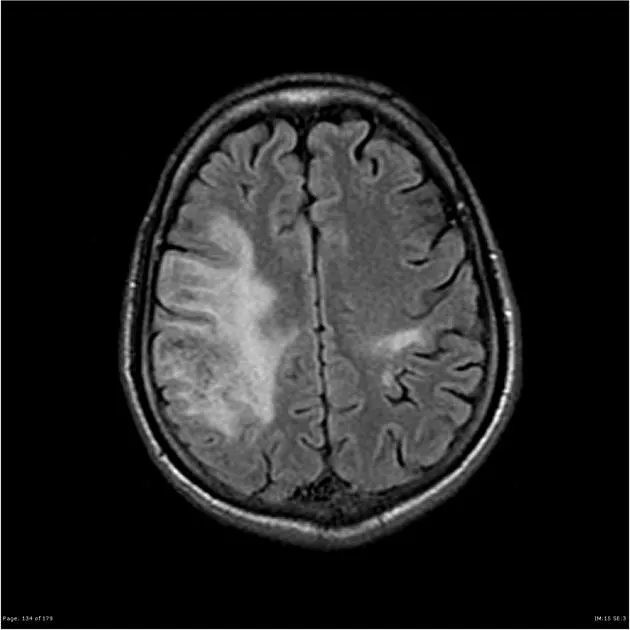
Progressive Multifocal Leukoencephalopathy (PML)
- Rare, severe brain infection caused by JC virus reactivation.
⭐ Exam Favorite: Suspect PML in a patient on B-cell depleting therapy presenting with new, progressive neurological deficits. Diagnosis is confirmed by JC virus DNA in CSF via PCR.
High-Yield Points - ⚡ Biggest Takeaways
- Rituximab is the key drug, a chimeric antibody targeting the CD20 antigen on B-lymphocytes.
- It works by causing B-cell apoptosis through complement-dependent cytotoxicity (CDC) and antibody-dependent cell-mediated cytotoxicity (ADCC).
- Crucially, it spares plasma cells, so pre-existing antibody levels are maintained.
- Used for B-cell lymphomas, CLL, and autoimmune diseases like rheumatoid arthritis.
- Watch for infusion reactions and a black box warning for Progressive Multifocal Leukoencephalopathy (PML).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

