CYP450 System - The Body's Detox Crew
- A superfamily of heme-containing monooxygenase enzymes, named for their characteristic 450 nm light absorption peak when bound to carbon monoxide.
- Primary Function: Central to Phase I drug metabolism. They catalyze reactions like oxidation, reduction, and hydrolysis, converting lipophilic compounds into more polar, water-soluble metabolites for excretion.
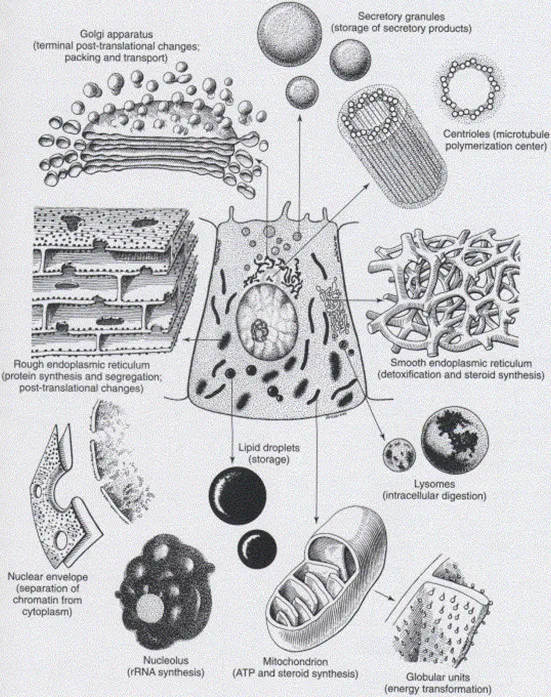
- Primary Location: Predominantly embedded in the smooth endoplasmic reticulum membrane of hepatocytes, with some presence in extrahepatic tissues (e.g., small intestine).
⭐ The CYP3A4 isozyme is the most abundant form, responsible for metabolizing approximately 50% of all clinically used drugs.
CYP450 Inducers - Stepping on the Gas
CYP450 inducers increase the synthesis of cytochrome enzymes, accelerating the metabolism of co-administered drugs. This leads to a ↓ in their plasma concentration and potential therapeutic failure.
- Mechanism: Upregulation of gene expression via activation of nuclear receptors (e.g., PXR, CAR).
- Clinical Consequences:
- ↓ plasma levels of other drugs (e.g., warfarin, OCPs) → subtherapeutic effect.
- ↑ activation of prodrugs → ↑ active metabolite levels & potential toxicity.
📌 Mnemonic: "CRAP GPS"
- Carbamazepine
- Rifampin
- Alcohol (chronic)
- Phenytoin
- Griseofulvin
- Phenobarbital
- St. John's Wort
⭐ Exam Favorite: St. John's Wort, an over-the-counter supplement for depression, is a potent CYP3A4 inducer, significantly reducing the efficacy of drugs like oral contraceptives and cyclosporine.
CYP450 Inhibitors - Hitting the Brakes
CYP450 inhibitors block the metabolic activity of one or more CYP enzymes through direct competition or irreversible inactivation. This slows the metabolism of other drugs, leading to ↑ plasma concentrations and risk of toxicity.
- Mechanism: Competitive or non-competitive binding to the enzyme active site.
- Clinical Effect: ↑ substrate drug levels, ↑ risk of adverse effects.
- Exception (Prodrugs): Inhibition ↓ conversion of prodrugs to their active form, leading to ↓ efficacy.
📌 Mnemonic: SICKFACES.COM
- Sodium valproate
- Isoniazid
- Cimetidine
- Ketoconazole
- Fluconazole
- Alcohol (acute)
- Chloramphenicol
- Erythromycin
- Sulfonamides
- .Ciprofloxacin
- Omeprazole
- Metronidazole
- Grapefruit juice
⭐ Exam Favorite: Co-administration of omeprazole (a potent CYP2C19 inhibitor) with clopidogrel (a prodrug activated by CYP2C19) can significantly reduce the antiplatelet effect of clopidogrel, increasing the risk of stent thrombosis.
Clinical Cross-Talk - Warfarin's Wild Ride
| Drug Interaction | Mechanism | Clinical Outcome |
|---|---|---|
| Warfarin + Rifampin | Rifampin induces CYP450 (notably CYP2C9), accelerating warfarin metabolism. | ↓ INR, leading to subtherapeutic anticoagulation. ↑ Risk of thrombosis. Requires ↑ warfarin dose. |
| Warfarin + Amiodarone | Amiodarone inhibits CYP450 (notably CYP2C9), slowing warfarin metabolism. | ↑ INR, leading to supratherapeutic anticoagulation. ↑ Risk of bleeding. Requires ↓ warfarin dose. |
High‑Yield Points - ⚡ Biggest Takeaways
- CYP450 inducers (Rifampin, Phenobarbital, Carbamazepine, St. John's Wort) accelerate metabolism, leading to ↓ drug effect or prodrug activation.
- CYP450 inhibitors (Grapefruit juice, Azoles, Macrolides, Protease Inhibitors) slow metabolism, causing ↑ drug levels & toxicity.
- Classic interaction: With Warfarin, inducers ↓ INR (clot risk), while inhibitors ↑ INR (bleed risk).
- Remember the kinetics: Inhibition is rapid, while induction is a slow process requiring new enzyme synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

