Malaria Lifecycle - Parasite's Progress
-
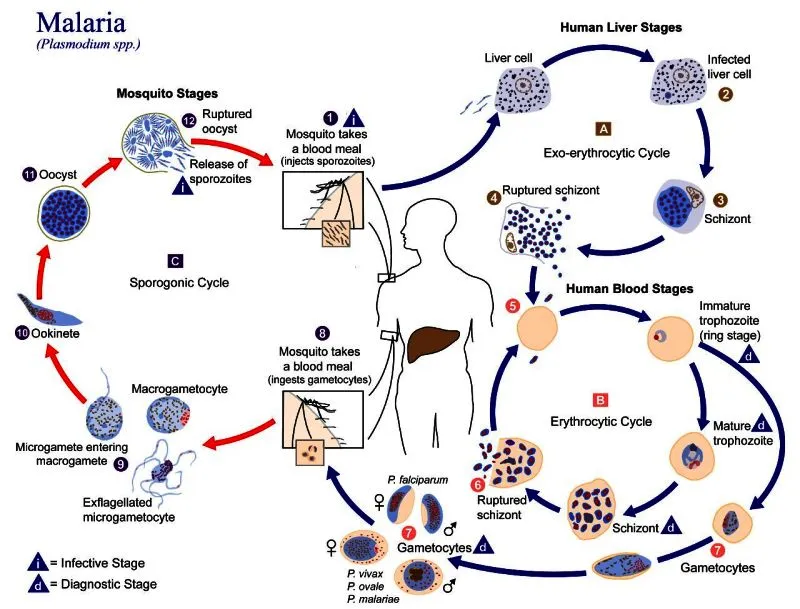
Human Host (Asexual Cycle)
- Exo-erythrocytic (Liver) Stage: Mosquito injects sporozoites → travel to liver → mature into schizonts → rupture, releasing merozoites.
- Erythrocytic (Blood) Stage: Merozoites invade RBCs → mature into trophozoites → ring forms → schizonts → rupture RBCs, causing clinical symptoms.
- Some parasites differentiate into gametocytes.
-
Mosquito Host (Sexual Cycle)
- Mosquito ingests gametocytes from human blood → mature into gametes → fertilization → oocyst forms → ruptures, releasing sporozoites.
⭐ Hypnozoites: P. vivax and P. ovale can form dormant liver stages called hypnozoites, which can reactivate months to years later, causing relapses. This is a key target for specific antimalarial drugs.
Blood Schizonticides - The Acute Attackers
-
Targets the erythrocytic stage of malaria, which is responsible for clinical symptoms. The primary use is for treating acute attacks.
-
Chloroquine
- MOA: Blocks the detoxification of heme into hemozoin by inhibiting heme polymerase. The resulting accumulation of free heme is toxic to the parasite.
- Use: Effective only against sensitive species; widespread resistance exists due to a membrane pump that decreases drug accumulation.
-
Artemisinins (Artesunate, Artemether)
- MOA: Metabolized in the parasite's food vacuole, generating free radicals that cause damage.
- Use: First-line for severe P. falciparum. Very rapid onset. Always used in combination (ACT) to prevent resistance.
-
Quinine & Quinidine
- MOA: Interferes with heme polymerization.
- Use: For severe malaria and chloroquine-resistant strains.
- Toxicity: Cinchonism (tinnitus, headache, dizziness), hypoglycemia. 📌 Quinine causes QT prolongation.
-
Mefloquine
- Use: Prophylaxis and treatment of chloroquine-resistant malaria.
- Toxicity: ⚠️ Can cause serious neuropsychiatric side effects.
⭐ G6PD Deficiency: Quinine and other oxidant drugs can trigger severe hemolytic anemia in patients with G6PD deficiency. Screening is crucial.
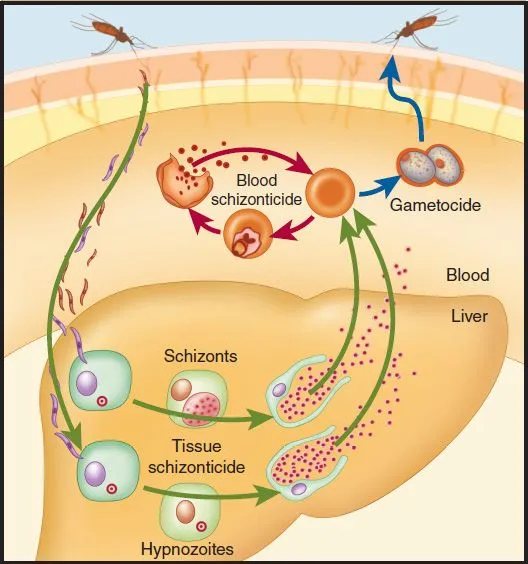
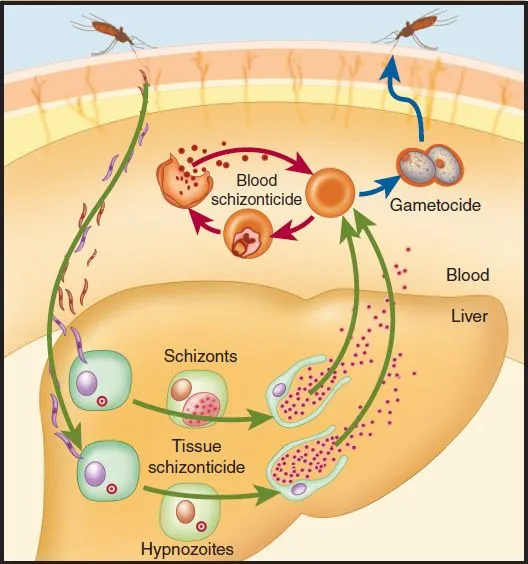
Tissue Schizonticides & Prophylaxis - Liver Stage & Prevention
-
Primary Goal: Eradicate dormant liver hypnozoites of P. vivax & P. ovale (radical cure) to prevent relapse. Also for primary prophylaxis against all species.
-
Key Agents:
- Primaquine & Tafenoquine:
- Active against hepatic stages (hypnozoites).
- Added to a blood schizonticide for radical cure of P. vivax/ovale.
- 📌 Primaquine Prevents Ping-pong relapses.
- ⚠️ Must screen for G6PD deficiency before use; risk of severe intravascular hemolysis.
- Atovaquone-Proguanil (Malarone):
- Excellent for prophylaxis in chloroquine-resistant areas.
- Disrupts parasite mitochondrial electron transport.
- Primaquine & Tafenoquine:
⭐ G6PD screening is mandatory before giving primaquine or tafenoquine. These drugs generate reactive oxygen species that overwhelm the antioxidant capacity of G6PD-deficient red blood cells, causing severe hemolysis.
High‑Yield Points - ⚡ Biggest Takeaways
- Chloroquine blocks heme polymerase but faces widespread resistance.
- Primaquine is essential for eradicating dormant hypnozoites (P. vivax/ovale); screen for G6PD deficiency to prevent hemolysis.
- Mefloquine prophylaxis is effective but carries a risk of neuropsychiatric side effects.
- Artemisinins are first-line for severe P. falciparum malaria, often used in Artemisinin-based Combination Therapy (ACT).
- Atovaquone-proguanil targets the electron transport chain and folate synthesis.
- Quinine/Quinidine can cause cinchonism and hypoglycemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

