Empiric Therapy - First Strike Fungi
- Indicated for high-risk, febrile neutropenic patients with persistent or recurrent fever after 4-7 days of broad-spectrum antibiotics, with no other identified cause.
- Goal: Preemptively cover the most probable fungal pathogens, primarily Candida species and Aspergillus.
- De-escalate to targeted therapy once a pathogen is identified and susceptibilities are determined.
⭐ Echinocandins are favored as initial therapy for most patients with suspected invasive candidiasis, particularly those who are hemodynamically unstable or had recent azole exposure.
Invasive Candidiasis - Crushing Candida
- Empiric First-Line: Echinocandins (e.g., caspofungin, micafungin) for most patients, especially if moderately to severely ill or recent azole exposure.
- Step-Down Therapy: Transition to Fluconazole within 5-7 days if patient is stable, isolates are susceptible, and blood cultures are negative.
- Specific Species:
- C. krusei: Intrinsically resistant to fluconazole; use echinocandins.
- C. glabrata: May have dose-dependent susceptibility to fluconazole; echinocandins are safer.
- Duration: Treat for 14 days after the first negative blood culture and clinical resolution.
⭐ Source control is paramount. If a central line is the suspected source, it must be removed as soon as possible.
Invasive Aspergillosis - Voriconazole's Victory
-
Primary Therapy: Voriconazole is the drug of choice, demonstrating superior efficacy over Amphotericin B.
- Requires therapeutic drug monitoring (TDM) due to variable metabolism.
- Key ADRs: Visual disturbances (flashing lights), photosensitivity, ↑LFTs.
-
Alternative Agents:
- Liposomal Amphotericin B (L-AMB).
- Isavuconazole (less hepatotoxicity and no photosensitivity).
⭐ Exam Favorite: Voriconazole is active against Candida (including krusei) and Aspergillus, but critically lacks coverage for Zygomycetes (Mucor, Rhizopus).
Other Key Pathogens - Crypto & Mucor Mayhem
-
Cryptococcus neoformans (Meningitis)
- 📌 Amp-ho-Flu → Flu: Amphotericin B + Flucytosine, then Fluconazole.
- Induction: Liposomal Amphotericin B + Flucytosine (≥2 weeks).
- Consolidation & Maintenance: Fluconazole (high-dose for 8 weeks, then low-dose ≥1 year).
-
Mucormycosis (e.g., Rhizopus, Mucor)
- Cornerstone: Aggressive surgical debridement.
- Medical: High-dose Liposomal Amphotericin B.
- Alternatives: Posaconazole, Isavuconazole.
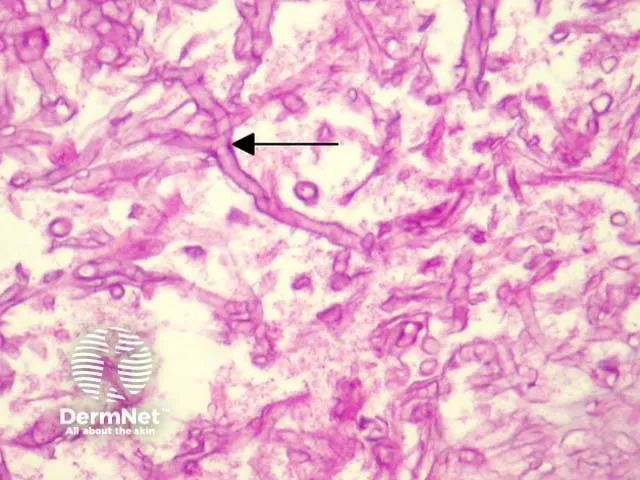
⭐ Voriconazole is ineffective against Mucorales. Prior voriconazole prophylaxis is a risk factor for breakthrough mucormycosis.
- Invasive Aspergillosis: Voriconazole is the drug of choice; alternatives include isavuconazole or liposomal amphotericin B.
- Invasive Candidiasis: First-line therapy is an echinocandin (e.g., caspofungin, micafungin); fluconazole for step-down.
- Cryptococcal Meningitis: Induction with amphotericin B + flucytosine, followed by fluconazole for consolidation and maintenance.
- Mucormycosis: Requires aggressive surgical debridement plus liposomal amphotericin B.
- Febrile Neutropenia: Add empiric antifungals if fever persists on broad-spectrum antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

