Enzymatic Destruction - The Drug Demolishers
- Bacteria produce enzymes that chemically modify and inactivate antibiotics, rendering them ineffective.
- Primary example: β-lactamases, which hydrolyze the amide bond in the β-lactam ring of penicillins and cephalosporins.
- Common in Staphylococcus aureus, Haemophilus influenzae, E. coli, and Klebsiella pneumoniae (which can produce Extended-Spectrum β-Lactamases, ESBLs).
- Other enzymes include aminoglycoside-modifying enzymes (e.g., acetyltransferases, phosphotransferases) that alter aminoglycoside structure.
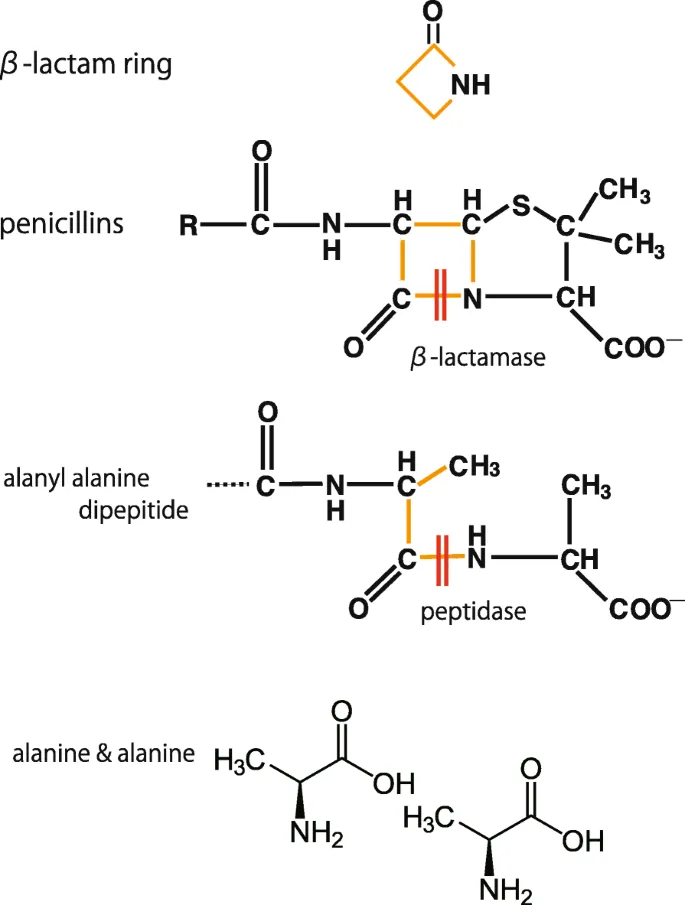
⭐ Clavulanate, Sulbactam, and Tazobactam are β-lactamase inhibitors co-formulated with penicillins to overcome this resistance mechanism. 📌 CAST (Clavulanate, Avibactam, Sulbactam, Tazobactam).
Target Modification - If You Can't Beat 'Em, Change
-
Bacteria alter the drug's target site, ↓ antibiotic binding & efficacy. 📌 "Change the lock so the key doesn't fit."
-
Cell Wall Synthesis:
- Beta-Lactams (e.g., Methicillin): Alteration of Penicillin-Binding Proteins (PBPs). The mecA gene in MRSA encodes PBP2a, which has low affinity for beta-lactams.
- Vancomycin: Modification of peptidoglycan precursor.
⭐ VRE (Vancomycin-Resistant Enterococci) changes D-Ala-D-Ala to D-Ala-D-Lac, preventing vancomycin binding.
-
Protein Synthesis:
- Macrolides/Clindamycin: Methylation of 23S rRNA binding site (erm gene) prevents drug binding.
-
Nucleic Acid Synthesis:
- Fluoroquinolones: Mutations in DNA gyrase & topoisomerase IV.
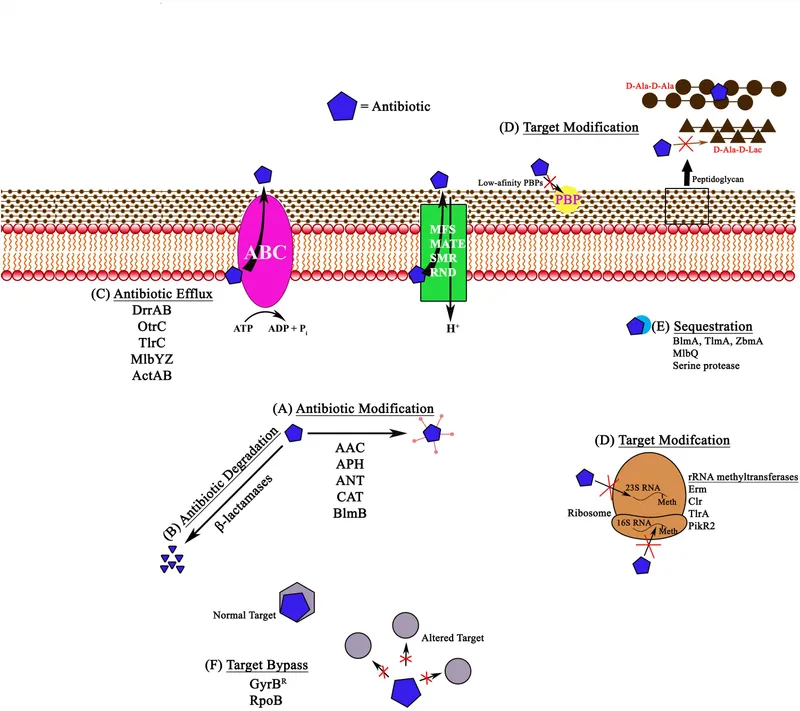
Reduced Permeability & Efflux - The Fortress Defense
-
Reduced Permeability: Bacteria limit antibiotic entry, primarily in Gram-negatives.
- Mechanism: Downregulation or mutation of outer membrane porin channels.
- Less influx means the antibiotic can't reach its intracellular target.
- Classic Example: Pseudomonas aeruginosa resistance to carbapenems.
-
Efflux Pumps: Actively transport antibiotics out of the cell.
- ATP-dependent pumps that recognize and expel drugs.
- Confers resistance to tetracyclines, macrolides, and fluoroquinolones.
- 📌 Pump Medications To Flight (Pseudomonas, Macrolides, Tetracyclines, Fluoroquinolones).
⭐ Pseudomonas aeruginosa exhibits high intrinsic resistance due to its very restrictive outer membrane porins and a wide array of constitutively expressed and inducible efflux pumps (e.g., MexAB-OprM).
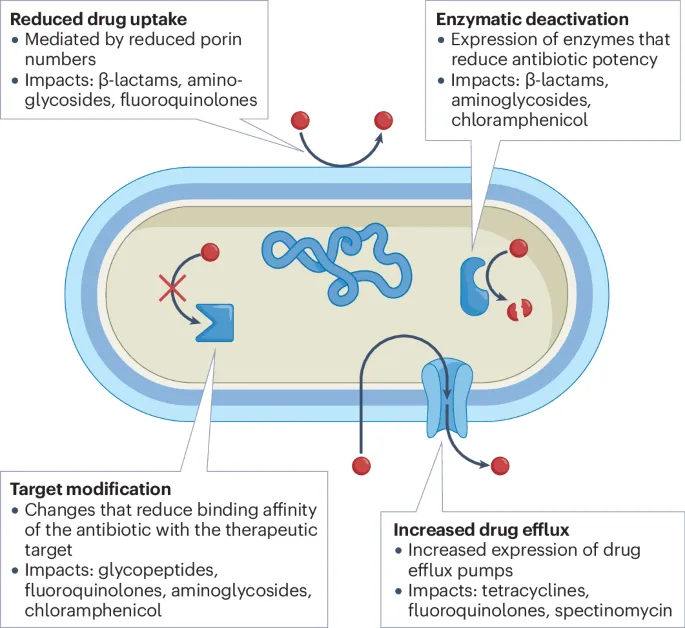
Genetic Mechanisms - Sharing the Cheat Codes
- Transformation: Bacteria uptake and incorporate naked DNA from the environment. A key mechanism for Streptococcus pneumoniae.
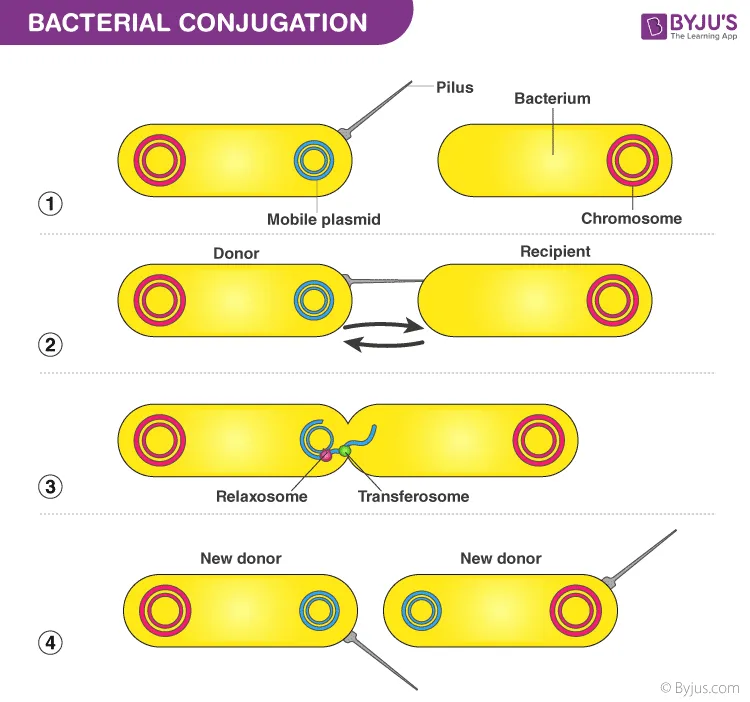
- Conjugation: Direct transfer of genetic material (plasmids, transposons) between bacteria via a sex pilus.
⭐ Plasmids, especially F-plasmids in Gram-negatives, are key drivers of multi-drug resistance transfer via conjugation.
- Transduction: A bacteriophage (virus) transfers genetic material from one bacterium to another.
- Transposons: "Jumping genes" that move resistance genes between plasmids and chromosomes.
High‑Yield Points - ⚡ Biggest Takeaways
- Enzymatic inactivation: β-lactamases are a classic example, breaking down penicillins and cephalosporins, leading to resistance.
- Target site modification: MRSA alters its penicillin-binding proteins (PBPs); fluoroquinolone resistance often involves mutated DNA gyrase.
- Active efflux pumps: These systems actively remove antibiotics like tetracyclines and macrolides from the bacterial cell.
- Decreased permeability: Gram-negative bacteria can mutate porin channels to prevent antibiotic entry into the cell.
- Metabolic pathway alteration: Bacteria may develop alternative pathways to bypass drugs like sulfonamides.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

