Pre-transport Stabilization - First, Pack 'Em Right
Stabilize before you mobilize. The ABCDE approach is paramount to prevent in-transit deterioration and ensure the child arrives alive and stable.
- A (Airway): Secure the airway; low threshold for early intubation. Maintain C-spine control in trauma.
- B (Breathing): High-flow O₂ to maintain SpO₂ >94%. Assist ventilation as needed.
- C (Circulation): Gain IV/IO access. Give isotonic crystalloid bolus (20 mL/kg) for shock. Use inotropes if shock persists.
- D (Disability & Dextrose): Assess GCS. MUST check blood glucose. Correct hypoglycemia (e.g., D10W 2-5 mL/kg).
- E (Environment & Exposure): Prevent hypothermia. Remove wet clothes, use warm blankets.
⭐ Hypoglycemia and hypothermia are silent killers in pediatric transport. Actively screen for and manage them to prevent cardiac arrest.
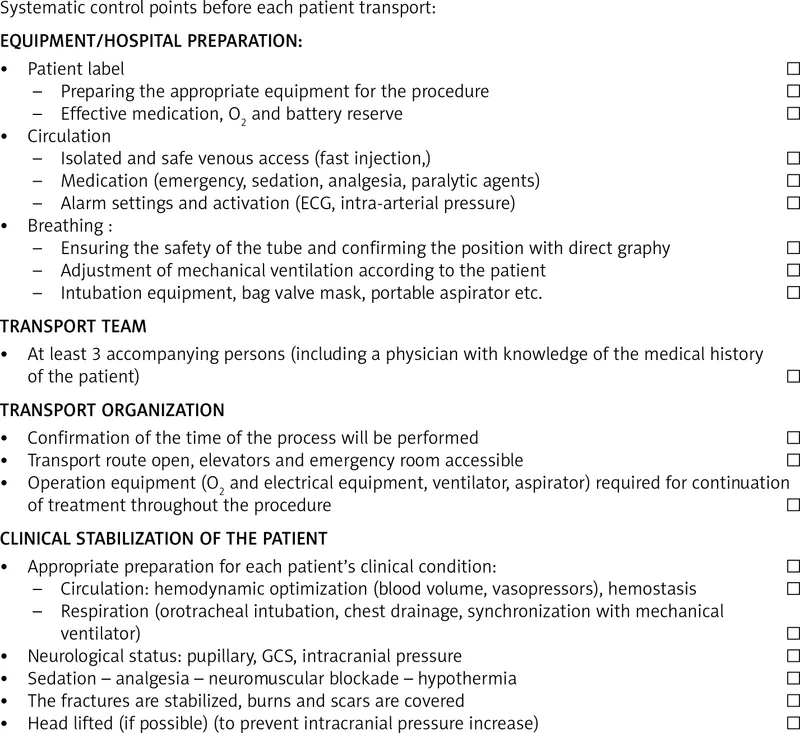

Transport Team & Equipment - The A-Team's Gear
-
Core Team Composition:
- Physician: Skilled in pediatric airway & resuscitation.
- Nurse: Critical care/emergency trained.
- Respiratory Therapist: As needed.
- Team Leader: Most experienced member; roles defined pre-departure.
-
Essential Equipment (📌 "A-B-C-D-E"):
- Airway: Laryngoscopes, ETTs, LMAs, suction.
- Breathing: Portable ventilator, O₂ source, bag-valve-mask.
- Circulation: IV/IO kits, infusion pumps, fluids.
- Drugs: PALS/NALS emergency drug box.
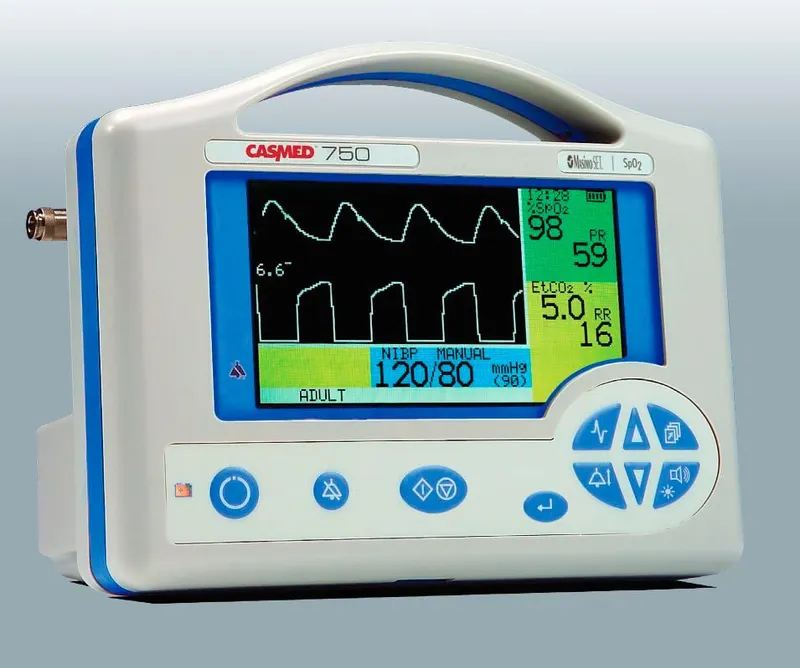
- Equipment (Monitoring): Multi-parameter monitor (ECG, SpO₂, BP, Temp), capnography, glucometer.

⭐ A pre-transport equipment checklist is mandatory. Forgetting a specific laryngoscope blade or finding an empty oxygen tank can be catastrophic. Always "Check-Before-You-Go".
In-Transit Monitoring - Are We There Yet?
- Continuous Vigilance: Constant monitoring is crucial. The transport environment is dynamic; anticipate and manage changes proactively.
- Core Monitoring (Every 5-15 min):
- ECG & HR: Detect arrhythmias, ischemia.
- Pulse Oximetry (SpO2): Target >94%.
- Capnography (EtCO2): Range 35-45 mmHg.
- NIBP: Cycle every 5-15 mins or more frequently if unstable.
- Temperature: Maintain normothermia (36.5-37.5°C).
- Documentation: Meticulously record vitals, events, and interventions. "If it wasn't documented, it wasn't done."
⭐ End-tidal CO2 (EtCO2) is the most reliable non-invasive indicator of endotracheal tube placement and adequacy of ventilation during transport.
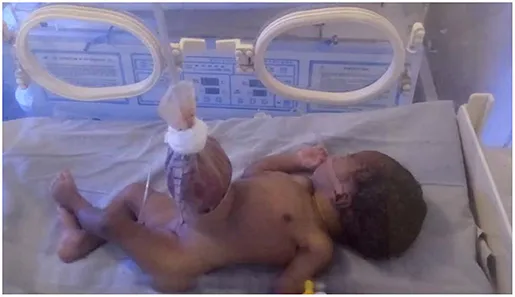
Special Cases - Tricky Tiny Travelers
- Congenital Diaphragmatic Hernia (CDH): Intubate immediately. AVOID Bag-Mask-Ventilation. Insert nasogastric tube to decompress bowel in chest.
- Tracheoesophageal Fistula (TEF): Nurse with head elevated 30-40°. Use a Replogle tube for continuous suction of the proximal pouch to prevent aspiration.
- Omphalocele/Gastroschisis: Cover abdominal defect with a sterile, saline-soaked dressing and plastic wrap or a "bowel bag" to minimize heat and fluid loss.
- Pierre Robin Sequence: Prone positioning is critical to prevent airway obstruction by the tongue.
⭐ In CDH, positive pressure ventilation via bag-mask can insufflate the stomach and intestines, severely compromising lung function and risking pneumothorax.
High‑Yield Points - ⚡ Biggest Takeaways
- Stabilization before transport is the most critical step; avoid the "scoop and run" approach.
- The transport team must be led by a physician skilled in pediatric emergencies.
- The most common preventable in-transit complications are hypoglycemia and hypothermia.
- Continuously monitor HR, RR, SpO2, BP, and temperature throughout the transfer.
- Ensure all lines, tubes, and equipment are secured and functional before departure.
- Utilize a structured handover tool like SBAR for clear communication with the receiving unit.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

