General Management - First-Response Playbook
- A, B, C, D, E: Airway, Breathing, Circulation, Disability (GCS, pupils), Exposure.
- Decontamination: Prevent absorption. Key is timing.
- Activated Charcoal: 1 g/kg within 1 hour. Does not bind all toxins. 📌 PHAILS: Pesticides, Hydrocarbons, Acids/alkalis, Iron, Lithium, Solvents.
- Gastric Lavage: Only for life-threatening ingestions within 1 hour. Contraindicated in corrosive/hydrocarbon poisoning.
- Enhanced Elimination: Hasten removal.
- Alkaline Diuresis: For salicylates, phenobarbital.
- Hemodialysis: For severe poisoning (e.g., methanol, salicylates, lithium).
⭐ For any unknown poisoning with altered sensorium, consider the empiric "coma cocktail": IV Dextrose, Naloxone, and Thiamine after securing ABCs.
Toxidromes - Poisoning Pattern Hunt
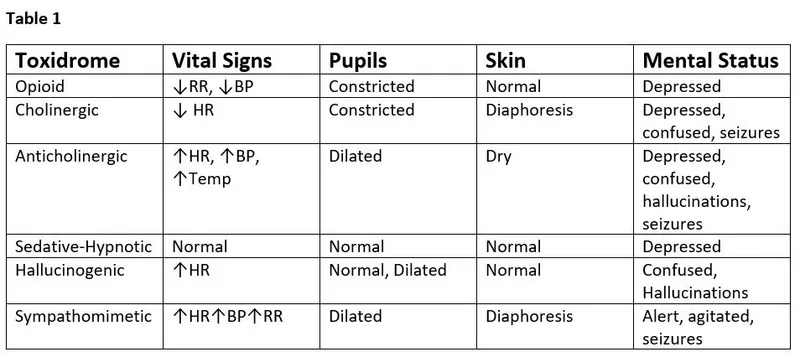
Recognizing toxidromes (toxicological syndromes) is key to identifying the poison class. Focus on vitals, pupils, and skin findings.
| Toxidrome | Vitals (HR, BP, T) | Pupils | Skin | Other | Examples |
|---|---|---|---|---|---|
| Anticholinergic | ↑ | Mydriasis | Hot, flushed, dry | ↓ Bowel sounds, urinary retention | Atropa belladonna, Datura, TCAs |
| Cholinergic | ↓ (Musc) / ↑ (Nic) | Miosis | Diaphoretic | ↑ Secretions (SLUDGE) | Organophosphates, Carbamates |
| Opioid | ↓ | Miosis (pinpoint) | Cool | ↓ RR, ↓ Bowel sounds | Morphine, Heroin, Fentanyl |
| Sympathomimetic | ↑ | Mydriasis | Diaphoretic | Agitation, seizures | Cocaine, Amphetamines |
| Sedative-Hypnotic | ↓ | Normal/Miosis | Normal | ↓ LOC, ↓ RR | Benzodiazepines, Barbiturates |
⭐ Differentiating Sympathomimetic vs. Anticholinergic: Both cause tachycardia, hypertension, and mydriasis. The key is the skin: Sympathomimetics are sweaty, while Anticholinergics are dry ("hot as a hare, dry as a bone").
Key Poisonings & Antidotes - Villains vs Heroes
| Poison (Villain) | Key Features / Toxidrome | Antidote (Hero) |
|---|---|---|
| Organophosphates | Cholinergic: DUMBELS | Atropine + Pralidoxime (PAM) |
| Paracetamol (PCM) | Hepatic necrosis (late) | N-acetylcysteine (NAC) |
| Iron | GI bleed, metabolic acidosis | Deferoxamine |
| Datura | Anticholinergic: "Hot as a hare..." | Physostigmine |
| Opioids | ↓CNS/Resp, pinpoint pupils | Naloxone |
| Benzodiazepines | Sedation, normal vitals | Flumazenil |
| Cyanide | Bitter almond breath | Hydroxocobalamin / Nitrites + Thiosulfate |
⭐ The Rumack-Matthew nomogram guides N-acetylcysteine (NAC) therapy in paracetamol poisoning. It's plotted from 4 hours post-ingestion; NAC is most effective if given within 8 hours.
High‑Yield Points - ⚡ Biggest Takeaways
- Organophosphate poisoning is treated with atropine and pralidoxime; atropine doesn't correct muscle weakness.
- For paracetamol toxicity, use the Rumack-Matthew nomogram to guide N-acetylcysteine administration.
- Iron poisoning is managed with deferoxamine, which causes a characteristic vin-rose colored urine.
- Salicylate toxicity presents with respiratory alkalosis then metabolic acidosis; treat with urinary alkalinization.
- The classic opioid toxicity triad is pinpoint pupils, respiratory depression, and coma; reverse with naloxone.
- For TCA overdose, QRS widening is a critical ECG finding, managed with sodium bicarbonate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

