Iron Deficiency - The Pale Story
- Etiology: Most common nutritional anemia worldwide.
- Causes: Inadequate intake, prematurity, exclusive breastfeeding >6mo, malabsorption (celiac disease), chronic blood loss (hookworm).
- Clinical Features:
- Pallor, fatigue, irritability.
- Pica (pagophagia: ice), koilonychia (spoon nails), glossitis.
- Plummer-Vinson syndrome: triad of dysphagia, esophageal webs, and IDA.
- Labs & Diagnosis:
- Microcytic hypochromic anemia (↓ MCV, ↓ MCH).
- ↓ Serum Ferritin (<15 ng/mL), ↓ Serum Iron, ↑ TIBC.
- Treatment: Oral elemental iron (3-6 mg/kg/day).
⭐ High-Yield: The earliest biochemical marker to decrease in iron deficiency is serum ferritin, reflecting depleted iron stores before anemia is apparent.
Vitamin A - See The Light
- Function: Essential for vision (retinal pigment), immune function, and epithelial cell integrity.
- Ocular Manifestations (Xerophthalmia):
- XN: Night blindness (earliest symptom).
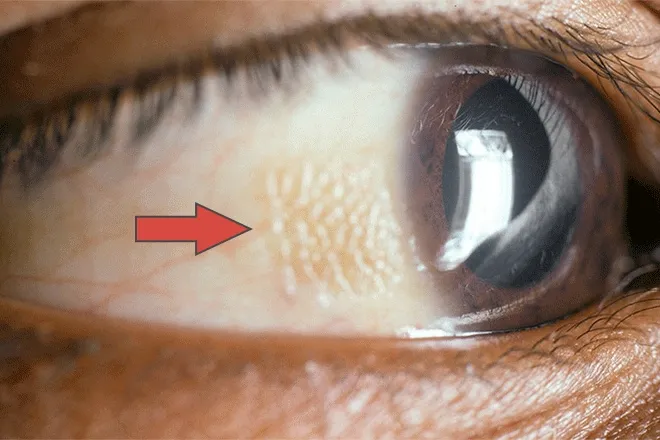
- X1A/B: Conjunctival xerosis & Bitot’s spots.
- X2/X3: Corneal xerosis, ulceration & keratomalacia.
- XS/XF: Corneal scarring & xerophthalmic fundus.
- Systemic: Follicular hyperkeratosis (phrynoderma), impaired immunity.
- Diagnosis: Serum retinol < 20 µg/dL.
- Treatment (WHO Schedule): Oral Vitamin A on days 0, 1, and 14.
- <6 mo: 50,000 IU
- 6-12 mo: 100,000 IU
-
1 yr: 200,000 IU
⭐ Bitot's Spots (X1B): Pathognomonic. Triangular, pearly-white/yellowish, foamy plaques of keratinized epithelium, classically on the temporal bulbar conjunctiva.
Vitamin D & Calcium - Rickets Rules
- Biochemistry: ↓ Ca²⁺, ↓ PO₄³⁻, ↑ Alkaline Phosphatase (ALP), ↑ PTH.
- ALP is the earliest marker to ↑.
- Clinical Features:
- Early: Craniotabes, wrist widening.
- Late: Rachitic rosary, Harrison's sulcus, delayed fontanelle closure, genu varum/valgum.
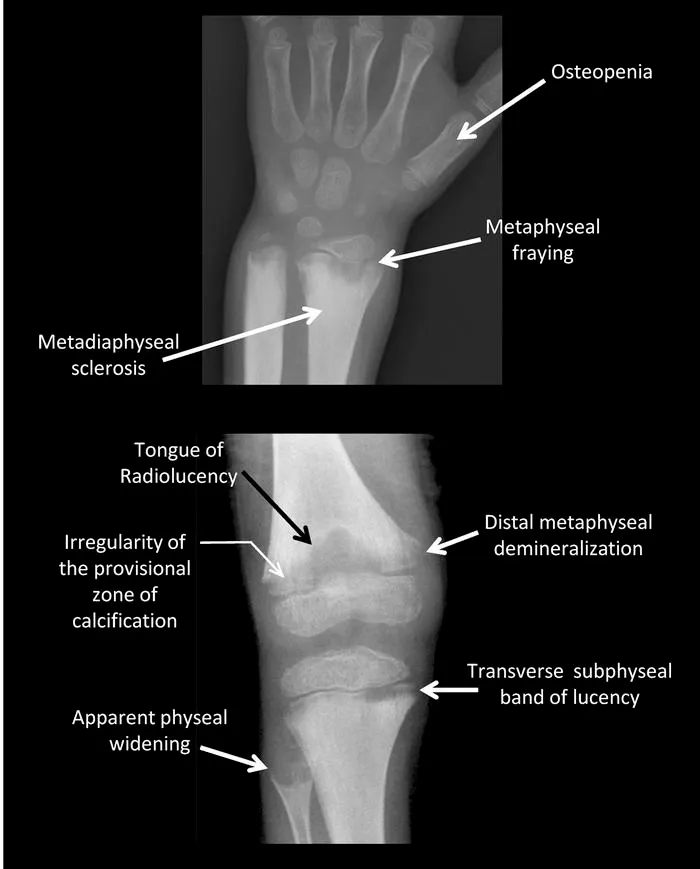
- X-Ray Findings (Metaphysis): Cupping, fraying, splaying.
- Looser's zones (pseudofractures) in osteomalacia.
- Treatment (Nutritional Rickets):
- Stoss Therapy: 600,000 IU Vitamin D₃ single dose.
- Daily: 3000-5000 IU for 6 weeks, then 400 IU prophylaxis.
- Always supplement with Calcium.
⭐ First radiological sign of healing is the appearance of the line of provisional calcification (usually within 2-4 weeks).
- VDDR-II: Features rickets + alopecia + very high 1,25(OH)₂D levels due to receptor defect.
Iodine & Zinc - The Essential Trace
-
Iodine Deficiency Disorders (IDD)
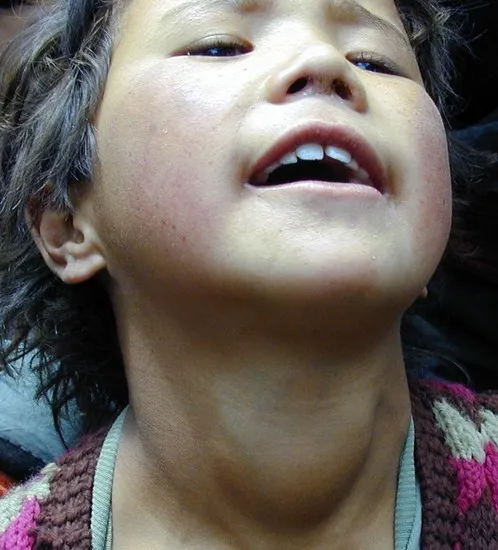
- Manifestations: Goiter, hypothyroidism, and cretinism (neurologic/myxedematous).
- Pathophysiology: ↓ Thyroid hormone synthesis → ↑ TSH.
- Diagnosis: Median urinary iodine < 100 µg/L.
- Prevention: Iodized salt (>15 ppm at consumer level).
-
Zinc Deficiency
- Classic Triad: Acrodermatitis enteropathica (periorificial/acral rash), alopecia, diarrhea.
- Other signs: Growth retardation, immune dysfunction.
⭐ High-Yield: Zinc supplementation (10-20 mg/day for 10-14 days) is crucial in acute diarrhea, reducing duration and severity.
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin A deficiency presents with Bitot's spots and keratomalacia; the first dose is given at 9 months with the measles vaccine.
- Rickets (Vitamin D deficiency) shows cupping, fraying, and splaying of metaphysis on X-ray, with rachitic rosary clinically.
- Scurvy (Vitamin C deficiency) is marked by bleeding gums, corkscrew hair, and subperiosteal hemorrhages.
- Iron deficiency, the most common nutritional disorder, causes microcytic hypochromic anemia; serum ferritin is the best screening test.
- Iodine deficiency is the most common preventable cause of intellectual disability (cretinism).
- Zinc deficiency classically presents as acrodermatitis enteropathica with periorificial dermatitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

