Etiology & Pathogenesis - The Tiny Invaders
-
Causative Agents:
- Early Onset (< 7 days): 📌 GEL
- Group B Strep (GBS) - Most common
- E. coli (esp. K1 strain)
- Listeria monocytogenes
- Late Onset (≥ 7 days):
- GBS, E. coli
- Staphylococci, Pseudomonas (nosocomial)
- Early Onset (< 7 days): 📌 GEL
-
Pathogenesis:
- Source: Maternal GU tract (early) or environment (late).
- Route: Hematogenous spread → bacteremia → meningeal seeding.
⭐ E. coli with the K1 capsular antigen is highly neuroinvasive, making it a leading cause of gram-negative neonatal meningitis.
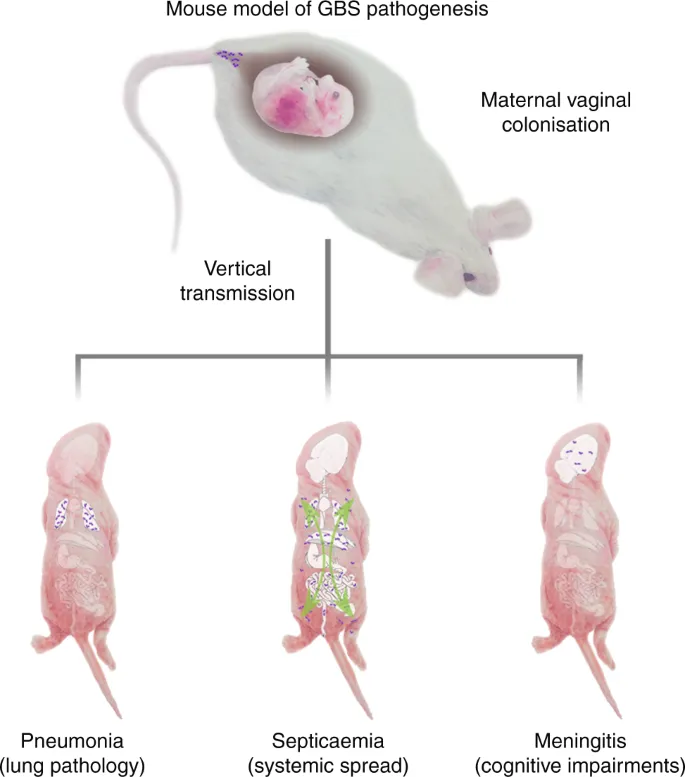
Clinical Features - Subtle Signs, Big Trouble
Signs are notoriously non-specific and subtle in neonates. Look for a constellation of findings rather than a single sign.
- Systemic: Temperature instability (fever or hypothermia), lethargy, poor feeding, irritability, vomiting, respiratory distress.
- Neurologic: Seizures (often subtle: e.g., staring, lip-smacking), altered sensorium, high-pitched cry, apnea.
- Fontanelle: Bulging or full anterior fontanelle is a late and unreliable sign.
- Classic Signs: Nuchal rigidity and Kernig's/Brudzinski's signs are typically absent.
⭐ Paradoxical irritability (crying when cuddled, quiet when left alone) is a subtle but important clue.
Diagnosis - The Spinal Tap Story
- Lumbar Puncture (LP) is mandatory on suspicion of meningitis.
- Contraindications: Cardiorespiratory instability, signs of ↑ Intracranial Pressure (ICP) like bulging fontanelle or focal deficits, infection at the puncture site, significant coagulopathy.
- CSF Analysis - Key Findings (Bacterial):
- Appearance: Turbid/Purulent
- Cells: ↑↑ Neutrophils (>80%); Total count often >1000/mm³
- Protein: ↑ >100-150 mg/dL
- Glucose: ↓ <40 mg/dL or CSF/Blood glucose ratio <0.4
- Gram Stain & Culture: Gold standard for pathogen identification.
- Adjunctive Tests:
- Blood Culture: Often positive.
- Latex Agglutination Test (LAT): For GBS, S. pneumoniae antigens.
⭐ In a traumatic (bloody) tap, a corrected WBC count is crucial. A common rule is to subtract 1 WBC for every 500-1000 RBCs in the CSF to estimate the true level of pleocytosis.
Management - Bug-Busting Bootcamp
- Empiric Antibiotics: Initiate ASAP after lumbar puncture.
-
Duration of Therapy (Minimum):
- Group B Strep: 14 days
- Listeria monocytogenes: 14-21 days
- Gram-Negative Bacilli (e.g., E. coli): 21 days
-
Supportive Care:
- Maintain fluid & electrolyte balance
- Control seizures (Phenobarbital)
- Monitor for complications (SIADH, hydrocephalus)
⭐ Exam Pearl: Cefotaxime is preferred over Ceftriaxone in neonates. Ceftriaxone displaces bilirubin from albumin, increasing the risk of kernicterus, and can cause biliary sludging.
Complications & Prognosis - The Aftermath
- Acute: SIADH, subdural effusion/empyema, ventriculitis, brain abscess, communicating hydrocephalus.
- Long-term Sequelae (25-50%):
- Sensorineural hearing loss (most common)
- Intellectual disability, epilepsy
- Cerebral palsy, visual impairment
- Prognosis:
- Mortality: 10-15% (GBS/E. coli), higher with other gram-negatives.
- Worse with seizures, coma, high CSF protein.
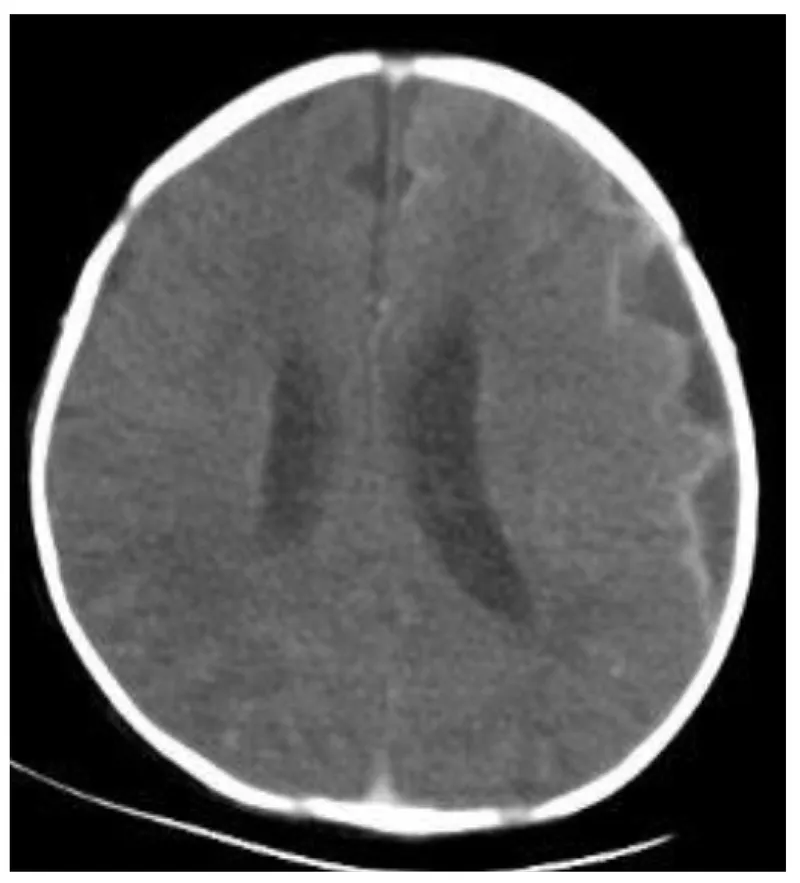
⭐ Sensorineural hearing loss is the most common sequela. All survivors require an auditory assessment (BERA/OAE) before discharge.
High‑Yield Points - ⚡ Biggest Takeaways
- Group B Streptococcus (GBS) is the leading cause of early-onset meningitis, while Coagulase-Negative Staphylococci (CoNS) is common in late-onset cases.
- Clinical signs are often non-specific (lethargy, poor feeding). A bulging fontanelle is a more specific and crucial sign.
- Lumbar puncture is the cornerstone of diagnosis; definitive diagnosis is by CSF culture.
- Empirical treatment is typically Ampicillin + Gentamicin or Ampicillin + Cefotaxime.
- Carries a high risk of severe long-term neurological sequelae.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

