Definition & Onset - The Late Invaders
- Definition: Sepsis clinically manifesting > 72 hours after birth.
- Contrasts with Early-Onset Sepsis (EOS), which occurs at < 72 hours and is vertically transmitted.
- Acquisition: Primarily horizontal transmission from the hospital environment (nosocomial) or community.
⭐ Coagulase-Negative Staphylococci (CoNS) is the most frequent pathogen, often linked to indwelling intravenous lines in preterm infants.
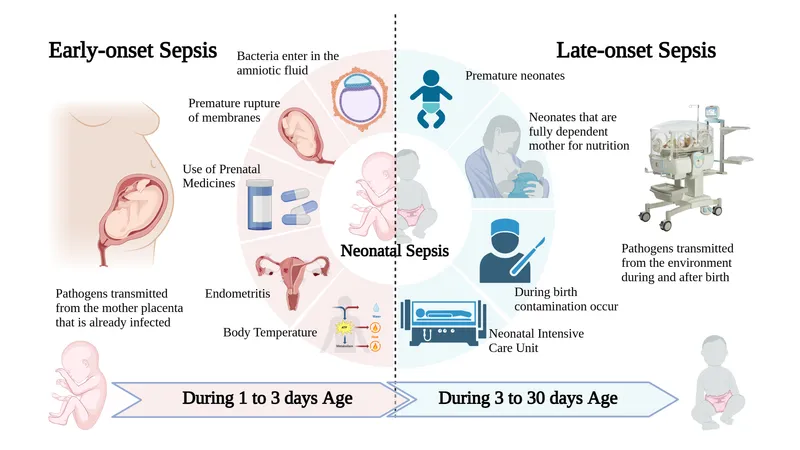
Etiology & Risk Factors - The Usual Suspects
- Major Risk Factors: Prematurity, Low Birth Weight (LBW), prolonged hospitalization.
- Invasive Devices: Central venous catheters, endotracheal tubes (mechanical ventilation).
| Organism | Common Sources / Associations |
|---|---|
| CoNS, S. aureus | Indwelling catheters, skin |
| Klebsiella, E. coli | Gut translocation, environment |
| Pseudomonas | Ventilators, humidifiers |
| Candida | Central lines, TPN, prior antibiotics |
⭐ Coagulase-negative staphylococci (CoNS) are the most common cause of late-onset sepsis, strongly associated with the presence of intravascular catheters.
Clinical Features - Subtle Warning Signs
Presentation is often subtle and non-specific. Any deviation from normal behavior warrants suspicion. Key signs include:
- Systemic: Temperature instability (fever >38°C or hypothermia <36.5°C), lethargy, hypotonia.
- Feeding: Poor feeding, vomiting, feeding intolerance.
- Cardio-Respiratory: Apnea, bradycardia, respiratory distress (grunting, tachypnea), poor perfusion (↑CRT >3s), hypotension.
- GI: Abdominal distension.
- CNS: Irritability, seizures (can be subtle: chewing, eye deviation).
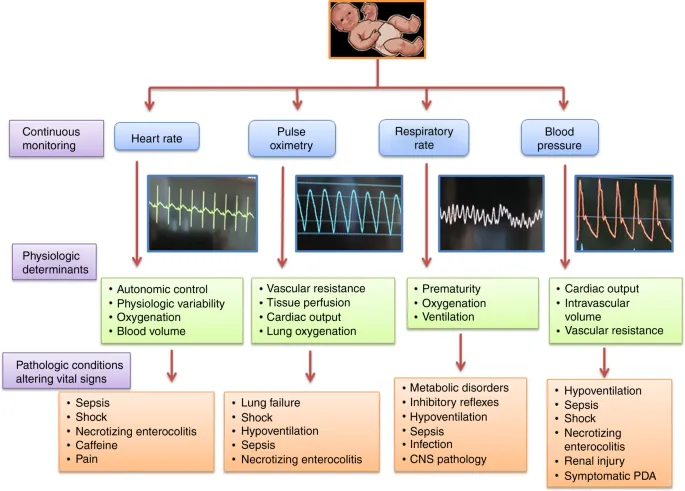
⭐ Apnea and bradycardia can be the only initial signs in preterm infants.
Diagnostic Workup - Cracking the Case
- Gold Standard: Blood culture is definitive.
- Sepsis Screen:
- Complete Blood Count (CBC) with peripheral smear.
- C-Reactive Protein (CRP): > 10 mg/L is significant.
- Micro-ESR.
- Key Markers:
- Immature-to-Total Neutrophil ($I:T$) ratio > 0.2.
- Crucial Investigations:
- Lumbar Puncture (LP): Essential for CSF analysis to rule out meningitis.
- Urine Culture: Via catheterization, especially if > 7 days old.
⭐ Serial CRP measurements are more valuable for monitoring treatment response than a single baseline value. A falling CRP indicates effective therapy.
Management & Prevention - Fighting Back Fast
- Empirical Antibiotics: Administer immediately after sending cultures. Goal is to cover common pathogens like CoNS, S. aureus, and Gram-negative bacilli.
- Standard Regimen: Vancomycin + an aminoglycoside (e.g., Amikacin) OR a 3rd-gen cephalosporin (e.g., Cefotaxime).
- Add Amphotericin B if fungal sepsis is suspected (risk factors: TPN, prior broad-spectrum antibiotics).
⭐ In neonates, Cefotaxime is preferred over Ceftriaxone. Ceftriaxone can displace bilirubin from albumin, increasing the risk of kernicterus, and can precipitate with calcium-containing IV solutions.
- Prevention: Key to reducing incidence.
- Strict hand hygiene & aseptic precautions for all procedures.
- Meticulous care of central and peripheral catheters.
- Promoting and supporting breastfeeding (provides IgA).
High‑Yield Points - ⚡ Biggest Takeaways
- Late-onset sepsis (LOS) is defined as sepsis occurring >72 hours after birth, typically acquired from the hospital environment (nosocomial).
- Coagulase-Negative Staphylococci (CoNS) is the most common causative organism, especially in preterm infants with indwelling central lines.
- Clinical signs are often subtle and non-specific, including lethargy, poor feeding, and temperature instability.
- Always suspect and evaluate for meningitis with a lumbar puncture, as it is a common co-occurrence.
- A definitive diagnosis requires a positive blood culture.
- Empirical antibiotics should cover both Gram-positive and Gram-negative organisms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

