Etiopathogenesis - The Trigger Theory
-
Infectious Trigger: Believed to be initiated by an unidentified infectious agent in genetically predisposed children.
- Epidemiological clues: Seasonal peaks (winter/spring), self-limited course, and geographic clustering.
- Suspected agents: Parvovirus B19, coronaviruses (HCoV-NH), bocavirus, Staphylococcus, Streptococcus.
-
Superantigen Hypothesis: The leading theory suggests bacterial toxins act as superantigens.
- These toxins bypass normal antigen processing.
- They directly link MHC class II on antigen-presenting cells to the T-cell receptor (TCR).
- Result: Massive, non-specific polyclonal T-cell activation and a subsequent cytokine storm (↑ TNF-α, IL-1, IL-6), leading to systemic inflammation and vasculitis.
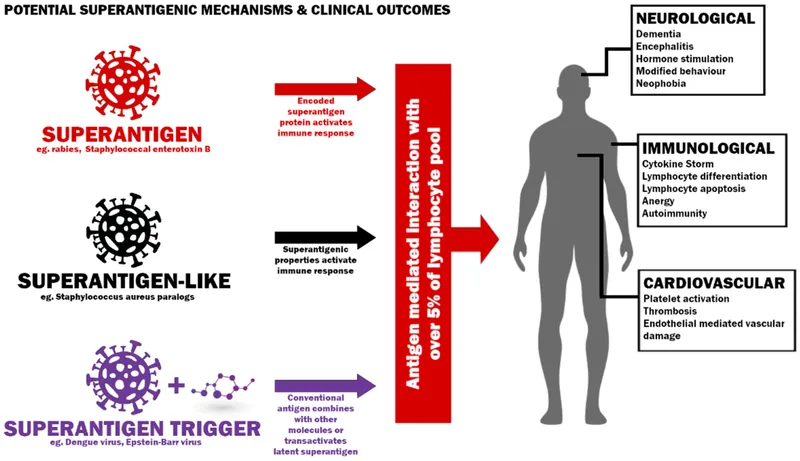
⭐ Exam Favourite: The superantigen theory is strongly supported by the association of Kawasaki disease with strains of Staphylococcus aureus (producing TSST-1) and Streptococcus pyogenes (producing pyrogenic exotoxins).
Immunopathogenesis - Superantigen Mayhem
- Trigger: An unknown trigger, likely infectious, is thought to introduce superantigens (SAgs) into the host.
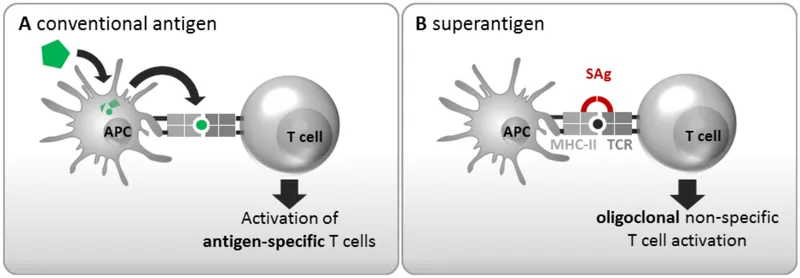
- Mechanism: SAgs bypass typical antigen processing.
- They directly cross-link the MHC class II molecules on antigen-presenting cells with the Vβ-region of the T-cell receptor (TCR).
- This leads to massive, non-specific (polyclonal) activation of T-lymphocytes.
- Inflammatory Cascade: Activated T-cells unleash a cytokine storm.
- Massive release of TNF-α, IL-1, IL-6, and other pro-inflammatory mediators.
- This drives systemic inflammation, endothelial cell activation, and widespread vasculitis.
⭐ The resulting pathology is a necrotizing vasculitis of medium-sized muscular arteries, with a distinct predilection for the coronary arteries.
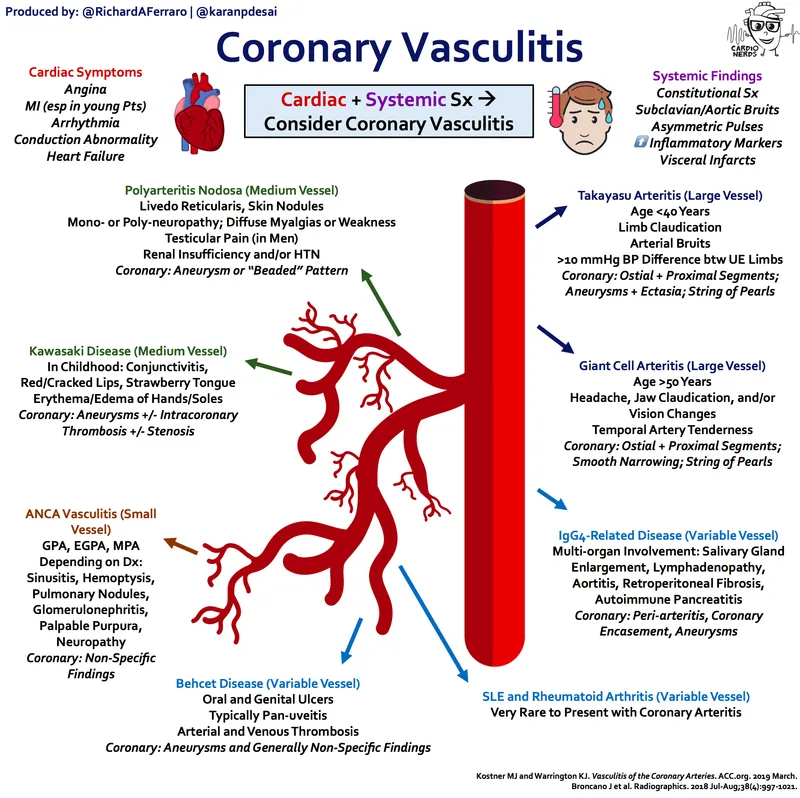
Vasculitic Pathology - The Artery Attack
- A systemic, necrotizing medium-vessel vasculitis with a strong predilection for the coronary arteries.
- Initial Stage (Weeks 1-2): Intense inflammation with neutrophils infiltrates all vessel layers (panvasculitis), causing edema.
- Subacute Stage (Weeks 2-4): The infiltrate evolves to lymphocytes, plasma cells, and eosinophils. This phase is critical for:
- Progressive destruction of the tunica media and internal elastic lamina.
- This structural damage directly weakens the wall, leading to ectasia and coronary artery aneurysms (CAA).
- Late Stage: Active inflammation subsides. Proliferation of myofibroblasts can cause progressive stenosis, thrombosis, or occlusion.
⭐ High-Yield Fact: The destruction of the internal elastic lamina is the key pathological event predisposing to aneurysm formation, making coronary artery involvement the most feared complication of Kawasaki disease.
High‑Yield Points - ⚡ Biggest Takeaways
- KD is an acute, necrotizing vasculitis of medium-sized arteries, especially the coronary arteries.
- The leading theory is a superantigen-mediated immune response, likely from a common infectious agent.
- This causes widespread T-cell activation and a massive cytokine storm (TNF-α, IL-1, IL-6).
- Another theory involves oligoclonal IgA plasma cells infiltrating tissues like the coronary arteries.
- Genetic susceptibility is crucial, with links to HLA-B51 and ITPKC gene polymorphisms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

