GH Physiology - The Growth Blueprint
- Secretion: Pulsatile, with largest peak during deep sleep (Stage N3).
- Actions (Dual Role):
- Direct: Anti-insulin effects (↑ lipolysis, ↑ blood glucose).
- Indirect: Via IGF-1 from liver; mediates linear growth (epiphyseal plates) and protein synthesis.
⭐ Screening for GH disorders relies on IGF-1 levels, not random GH, due to GH's pulsatile release versus IGF-1's stable, longer half-life.
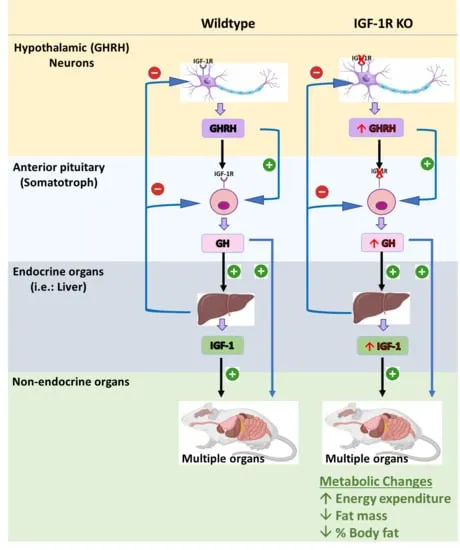
GH Deficiency - The Short Story
-
Etiology
- Congenital: Idiopathic (most common), genetic (e.g., GH1, GHRHR mutations), midline defects (septo-optic dysplasia).
- Acquired: Craniopharyngioma (most common tumor), CNS radiation, trauma, infection.
-
Clinical Features
- Neonate: Hypoglycemia, micropenis, prolonged jaundice.
- Child: Short stature (height < -2 SD), ↓ growth velocity, delayed bone age, cherubic facies, truncal obesity, high-pitched voice.
-
Diagnosis & Treatment
- Screening: ↓ IGF-1 & IGFBP-3.
- Confirmation: GH stimulation tests (Insulin, Clonidine). Peak GH < 10 ng/mL is diagnostic.
- Imaging: Pituitary MRI to identify structural causes.
- Treatment: Recombinant Human GH (rhGH).
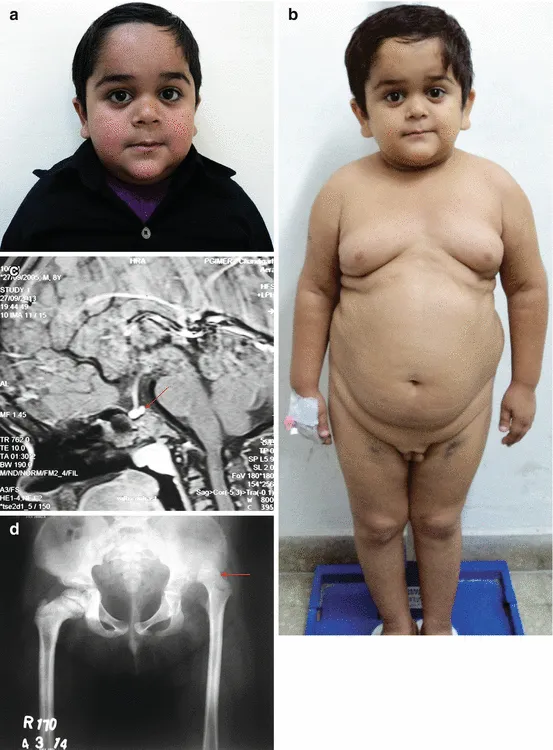
⭐ Laron Syndrome: A GH receptor defect causing GH insensitivity. Presents with features of GHD but has ↑ GH and ↓ IGF-1 levels.
GH Excess - Towering Troubles
- Etiology: Most commonly a pituitary adenoma.
- Clinical Manifestations:
- Gigantism: Before epiphyseal fusion. Symmetrical overgrowth, ↑ height.
- Acromegaly: After epiphyseal fusion. Coarse facial features, frontal bossing, prognathism, macroglossia, spade-like hands/feet.
- Systemic: Cardiomegaly, hypertension, insulin resistance (diabetes).
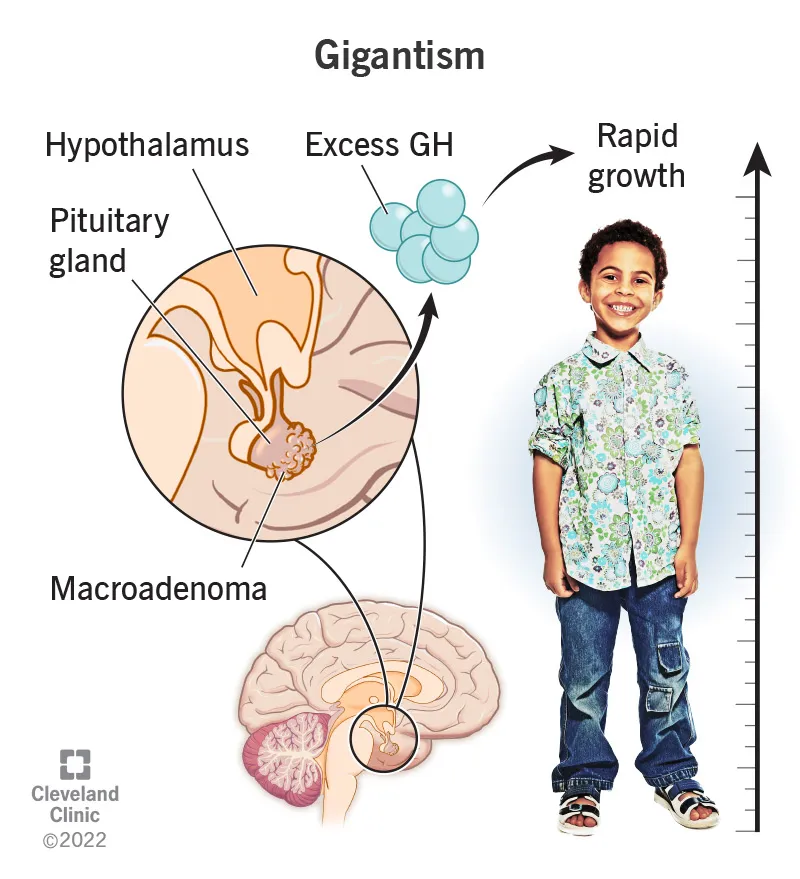
- Diagnosis:
⭐ Most specific test: Oral Glucose Tolerance Test (OGTT). Failure to suppress GH levels below 1 ng/mL after a 75g glucose load is diagnostic.
- Management:
- 1st Line: Trans-sphenoidal surgery.
- Medical: Somatostatin analogs (Octreotide), GH receptor antagonists (Pegvisomant).
Laron Syndrome - Unresponsive Receptors
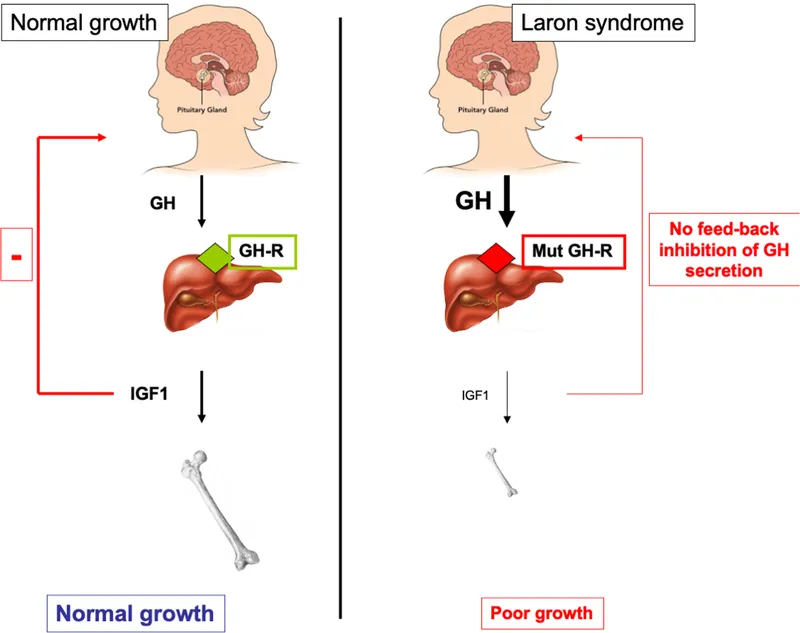
- Pathophysiology: Autosomal recessive mutation in the Growth Hormone Receptor (GHR) gene, causing end-organ insensitivity to GH.
- Biochemical Profile: ↑ GH, but ↓↓ IGF-1 & IGFBP-3. This paradoxical finding is key.
- Clinical Features: Severe short stature, prominent forehead, depressed nasal bridge, small hands/feet, and hypoglycemia.
- Treatment: Ineffective GH therapy. Requires Recombinant IGF-1 (Mecasermin).
⭐ Exam Pearl: Despite obesity, patients with Laron syndrome have a significantly lower incidence of cancer and diabetes mellitus.
High‑Yield Points - ⚡ Biggest Takeaways
- GH deficiency is a key cause of pathological short stature, often with neonatal micropenis and hypoglycemia.
- Screening involves IGF-1/IGFBP-3 levels; confirmation needs GH stimulation tests (e.g., insulin-induced hypoglycemia).
- Laron syndrome (GH insensitivity) is a receptor defect presenting with high GH but low IGF-1.
- GH excess causes gigantism before epiphyseal fusion and acromegaly after.
- The most common cause of GH excess is a pituitary adenoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

