Muscular Dystrophies - An Overview
- Inherited genetic disorders causing progressive muscle weakness and degeneration, with muscle tissue replaced by fat and fibrous tissue.
- Classified based on mode of inheritance, age of onset, and distribution of weakness.
- Major types include:
- Dystrophinopathies (Duchenne, Becker)
- Myotonic Dystrophy
- Limb-Girdle Muscular Dystrophies (LGMDs)
- Facioscapulohumeral Dystrophy (FSHD)

⭐ Dystrophinopathies (DMD, BMD) are X-linked recessive disorders caused by mutations in the dystrophin gene, primarily affecting males.
Duchenne MD - Gower's Power-Up Fail
- X-linked recessive disorder; mutation in the dystrophin gene (Xp21).
- Presents at 3-5 years with progressive proximal muscle weakness.
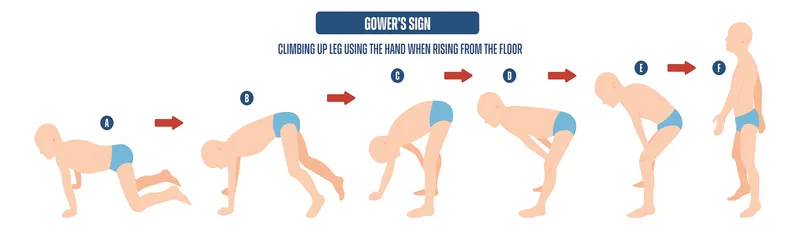
- Key Signs: Gower's sign, waddling gait, and calf pseudohypertrophy (fatty/fibrous infiltration).
- Investigations:
- ↑↑ Serum Creatine Kinase (CK) > 10,000 U/L.
- Muscle Biopsy: Absent dystrophin staining.
- Genetic analysis is the gold standard.
⭐ Becker MD vs. Duchenne MD: Becker has a later onset and reduced dystrophin (not absent), leading to a milder phenotype. Cause of death in DMD is typically cardiorespiratory failure by age 20-30.
📌 Mnemonic: Duchenne = Deleted Dystrophin.
Becker MD - Duchenne's Kinder Cousin
- Genetics: X-linked recessive; in-frame dystrophin gene mutation. Produces a shorter but partially functional protein.
- Onset & Progression: Milder than DMD. Onset: 5-15 years. Slower progression; patients often ambulatory past 16 years, sometimes into their 30s.
- Clinical Features:
- Progressive proximal muscle weakness (pelvic girdle).
- Calf pseudohypertrophy.
- Gower's sign is present.
- Complications: Cardiomyopathy is a significant cause of mortality.
⭐ Key Distinction: BMD results from an in-frame mutation (partially functional dystrophin), while DMD has a frameshift mutation (non-functional protein).
Myotonic Dystrophy - The Shake-It-Off Struggle
- Autosomal Dominant; CTG trinucleotide repeat expansion in DMPK gene.
- Myotonia: Delayed muscle relaxation (e.g., can't let go of handshake).
- Clinical Features: Progressive distal muscle weakness, "hatchet face" (temporal wasting, ptosis), dysphagia.
- Systemic Involvement:
- Cataracts (iridescent "Christmas tree" type)
- Frontal balding, testicular atrophy
- Cardiac conduction defects (arrhythmias)
⭐ Anticipation: Disease severity increases & age of onset decreases in successive generations.
Other Types - The Supporting Cast
- Myotonic Dystrophy (DM1): Autosomal Dominant (CTG repeat). Myotonia (impaired muscle relaxation), distal weakness, “Christmas tree” cataracts, frontal balding, and cardiac conduction defects.
⭐ Genetic anticipation is characteristic: disease severity increases and age of onset decreases in successive generations.
- Facioscapulohumeral Dystrophy (FSHD): Presents with facial weakness (inability to smile/whistle), scapular winging, and upper arm weakness. Often asymmetric.
- Emery-Dreifuss (EDMD): 📌 Classic triad: early contractures (elbows, Achilles), slowly progressive weakness, and life-threatening cardiac conduction defects.
High-Yield Points - ⚡ Biggest Takeaways
- Duchenne (DMD) and Becker (BMD) muscular dystrophies are X-linked recessive disorders affecting the dystrophin protein.
- Gower's sign (using hands to push off legs to stand) is a classic sign of DMD.
- BMD is a milder variant of DMD with a later onset and slower progression.
- Myotonic dystrophy, an autosomal dominant condition, is characterized by myotonia, cataracts, and cardiac issues.
- Limb-girdle muscular dystrophy presents with proximal muscle weakness in the shoulder and pelvic girdles.
- Serum Creatine Kinase (CK) is massively elevated in DMD/BMD.
- Glucocorticoids are the primary treatment to slow disease progression in DMD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

