NTD Embryology - The Great Closure
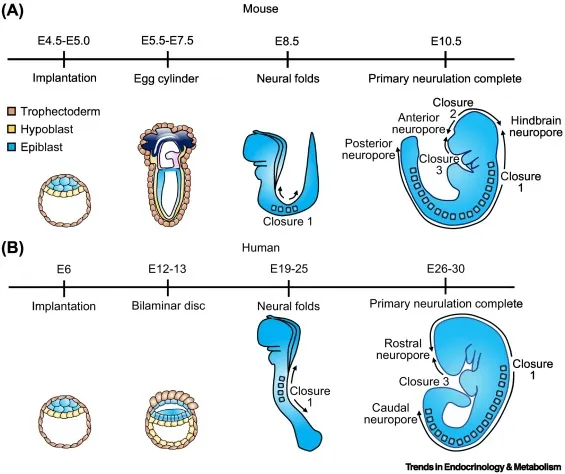
- Neurulation (Week 3-4): Neural plate folds into the neural tube. Closure begins cervically, extending cranially and caudally.
- Anterior (Rostral) Neuropore: Closes ~Day 25. Failure → Anencephaly.
- Posterior (Caudal) Neuropore: Closes ~Day 27-28. Failure → Spina Bifida.
- Folic Acid's Role: Essential for the Methionine-Homocysteine pathway, crucial for DNA synthesis and cell division.
- Prevention Dosage:
- Low-risk: 400 mcg/day pre-conceptionally.
- High-risk (e.g., prior NTD): 4 mg/day.
- Prevention Dosage:
⭐ Exam Fact: Neural tube closure is complete by the 4th week post-conception, often before a woman realizes she is pregnant. This underscores the critical need for pre-conceptional folate supplementation.
NTD Spectrum - Open & Shut Cases
Neural tube defects (NTDs) are classified as open (exposed neural tissue) or closed (skin-covered).
| Defect | Common Location | Sac Contents | Skin Cover | Key Clinical Signs |
|---|---|---|---|---|
| Spina Bifida Occulta | Lumbosacral | None | Yes (intact) | Tuft of hair, dimple, lipoma |
| Meningocele | Lumbosacral | Meninges + CSF | Yes (thin) | Visible cystic swelling |
| Myelomeningocele | Lumbosacral | Cord + Meninges + CSF | No (open) | Neurological deficits below lesion |
| Anencephaly | Cranial | - | No | Absence of forebrain/skull |
| Encephalocele | Occipital | Brain + Meninges + CSF | Yes | Visible sac on the skull |
⭐ Exam Favourite: Myelomeningocele is almost universally associated with Arnold-Chiari II malformation, causing hydrocephalus.
Clinical Clues - Finding the Flaw
Focuses on prenatal diagnosis, primarily through maternal screening and ultrasound.
-
Maternal Serum Screening (Triple/Quad Screen) at 15-20 weeks:
- ↑ Alpha-fetoprotein ($AFP$): Open neural tube allows fetal protein to leak into amniotic fluid and maternal circulation.
- ↑ Acetylcholinesterase ($AChE$) in amniotic fluid: More specific than AFP.
-
Level II Ultrasound Findings:
- Anencephaly: 'Frog-eye' or 'Mickey Mouse' sign due to absent cranial vault.
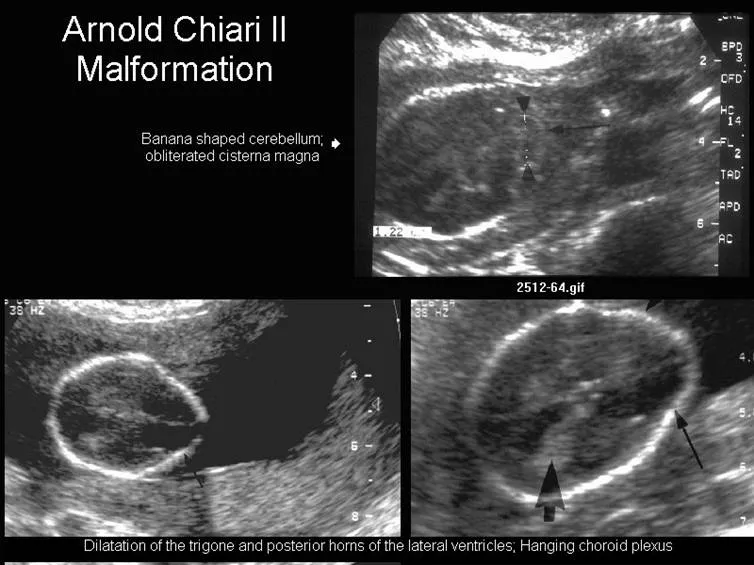
- Spina Bifida (Chiari II Malformation):
- 'Lemon sign': Scalloping of frontal bones.
- 'Banana sign': Cerebellum is pulled caudally, obliterating the cisterna magna.
⭐ High-Yield Fact: While elevated maternal serum $AFP$ is a sensitive screening marker, the presence of Acetylcholinesterase ($AChE$) in the amniotic fluid is highly specific for an open NTD.
Complications & Care - The Aftermath
-
Immediate Complications:
- Hydrocephalus: Blockage of CSF flow; occurs in >80% of cases.
- Arnold-Chiari II Malformation: Universal finding in myelomeningocele; cerebellar vermis & medulla herniate through foramen magnum.
- Neurogenic Bladder/Bowel: Risk of incontinence, retention, and recurrent UTIs.
- Motor/Sensory Deficits: Flaccid paralysis, lack of sensation below the lesion level.
-
Management Principles:
- Surgical Closure: Ideally within 24-72 hours to minimize infection risk.
- Ventriculoperitoneal (VP) Shunt: Placed to manage progressive hydrocephalus.
⭐ Exam Pearl: The level of motor paralysis is the single most useful predictor of ambulation potential.
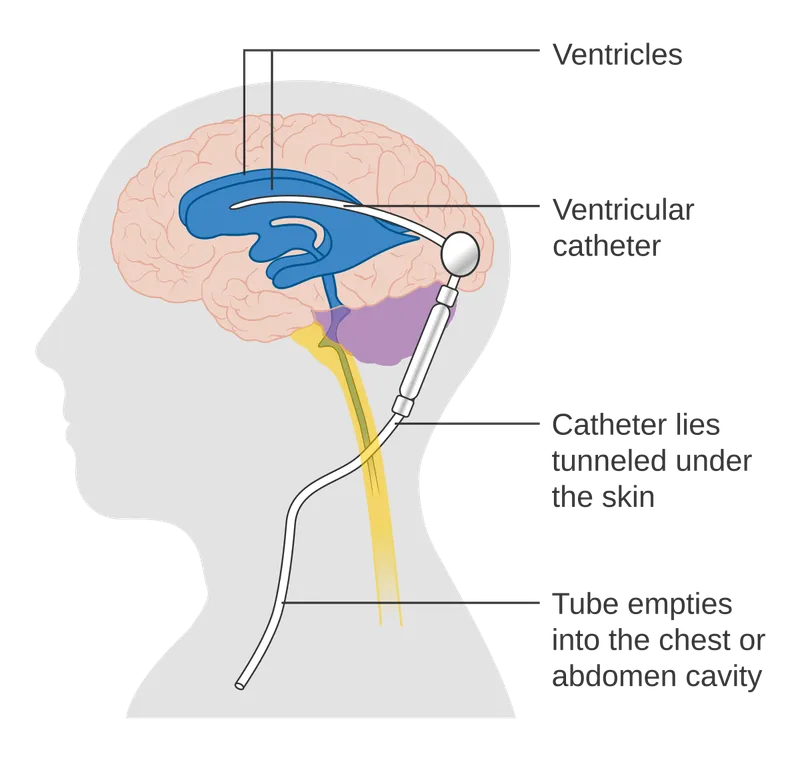 shunt placement for hydrocephalus)
shunt placement for hydrocephalus)
- Folic acid supplementation is the most crucial preventive measure; dose varies with risk (0.4 mg vs 4 mg).
- Maternal serum alpha-fetoprotein (MSAFP) is the key screening marker, elevated in open NTDs.
- Ultrasound is the primary diagnostic tool for antenatal detection.
- Anencephaly presents with polyhydramnios and a characteristic "frog-eye" appearance; it is lethal.
- Myelomeningocele is the most common severe form, strongly associated with Arnold-Chiari II malformation and hydrocephalus.
- Spina bifida occulta is the mildest form, often marked only by a sacral dimple or hair tuft.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

