Reproductive Ethics - Life's Big Questions
- Contraception & Sterilization: Patient autonomy is paramount. Minors' rights to access contraception vary by state. For sterilization, informed consent must be rigorous to prevent coercion, especially in vulnerable populations.
- Abortion: Involves a conflict between maternal autonomy and the moral/legal status of the fetus. The legal framework is highly variable post-Dobbs decision, shifting regulation to the state level.
- Assisted Reproductive Technology (ART): Includes IVF, surrogacy. Creates ethical dilemmas regarding the disposition of unused embryos, selective reduction, and rights of gamete donors/surrogates.
⭐ A key ethical and legal issue is whether a minor can consent to an abortion without parental notification or consent, which varies significantly by state.
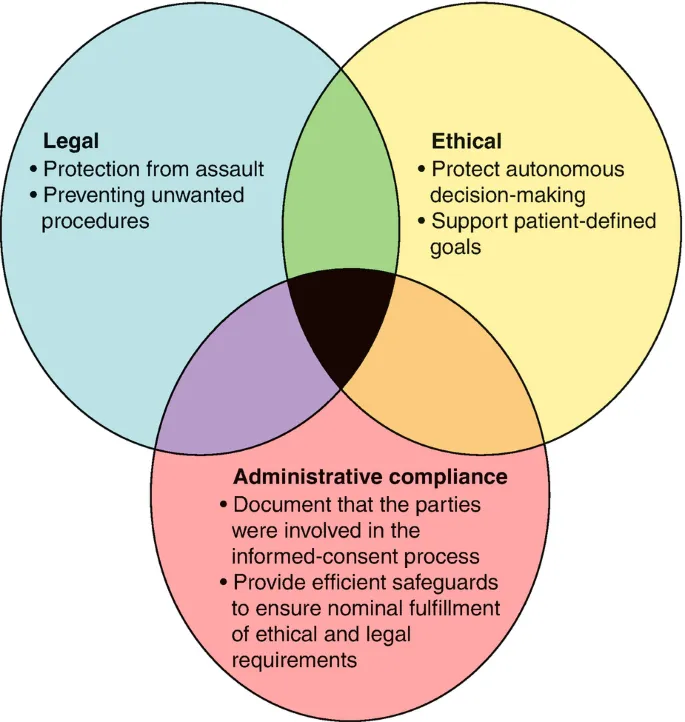
Contraception & Abortion - Choice & Controversy
- Core Principles: Patient autonomy is paramount. Decisions involve a complex interplay of beneficence, non-maleficence, and justice in the context of reproductive rights.
- Informed Consent: Mandatory for all procedures. Must cover risks, benefits, and alternatives. State laws vary significantly regarding minors, parental consent, and judicial bypass.
- Conscientious Objection: Physicians may decline to provide services (e.g., abortion) that violate their deeply held moral or religious beliefs.
- This right is not absolute. It must not create an undue burden or obstruct a patient's access to care.
⭐ A physician exercising conscientious objection still has an ethical and often legal duty to refer the patient to another provider in a timely manner.
Assisted Reproductive Tech - Making Modern Miracles
-
ART involves handling gametes/embryos to achieve pregnancy, raising complex ethical, legal, and social questions. Key methods include IVF, ICSI, and IUI.
-
Core IVF Sequence:
- Ethical Framework:
- Informed Consent: Must be exhaustive, covering success rates, risks (e.g., Ovarian Hyperstimulation Syndrome), and the disposition of unused embryos.
- Status of Embryos: Requires explicit directives for cryopreserved embryos, especially in cases of divorce or death.
- PGD: Screens for genetic disorders; use for non-medical trait selection is highly controversial.
- Third-Party Reproduction: Surrogacy and gamete donation raise complex issues of parentage, anonymity, and psychological impact.
⭐ Disputes over cryopreserved embryos after a couple divorces are a common ethical vignette. A prior written agreement or "embryo directive" is the best legal and ethical guide.
Maternal-Fetal Conflict - Two Patients, One Body
- Primary Patient: The pregnant person is the sole individual with legal rights and full autonomy. The fetus is not considered a separate legal person.
- Respect for Autonomy: A competent pregnant patient's informed decision to refuse any treatment (e.g., C-section) must be respected, even if it could harm the fetus. Forcing treatment constitutes battery.
- Physician's Duty: Counsel on risks/benefits to both parties. The goal is to find a solution that honors the patient's wishes without coercion.
⭐ ACOG strongly opposes using court orders to compel treatment. A competent patient's refusal of care is ethically and legally the final word.
- Minors can confidentially consent to contraception and STI services without parental permission.
- A competent pregnant patient's autonomy to refuse treatment overrides fetal interests in a conflict.
- Informed consent for sterilization must be voluntary, with full disclosure of its permanence.
- Physicians with a conscientious objection must still provide a timely referral to another provider.
- Key ART ethics issues include the disposition of unused embryos and respecting procreative autonomy.
- A competent patient’s bodily integrity allows refusal of any procedure, even if it benefits the fetus.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

