Core Principles - The Big Four
-
Autonomy: The patient's right to make informed, voluntary, and competent decisions about their own medical care.
- Foundation for informed consent, truth-telling, and confidentiality.
- Respects individual values, even if they conflict with the physician's recommendations.
-
Beneficence: The duty to act in the best interest of the patient; to promote their well-being.
- Focuses on providing a net benefit to the patient.
- Core concept: "Do good."
-
Non-maleficence: The duty to avoid causing unnecessary harm to the patient.
- "Primum non nocere" or "First, do no harm."
- Requires balancing the potential benefits against the risks of any intervention.
-
Justice: Fair and equitable distribution of healthcare resources and treatment.
- Treating similar cases with similar care, regardless of patient characteristics.
- Applies to both individual patient encounters and societal resource allocation.
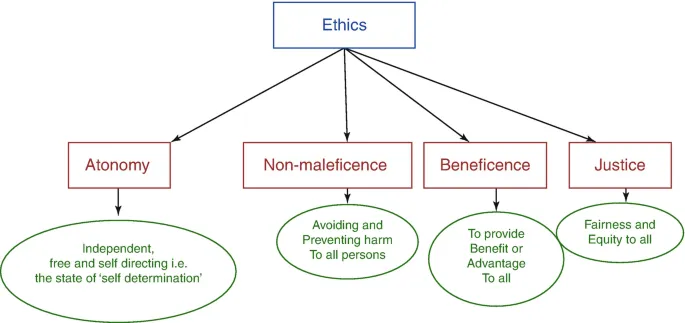
⭐ Ethical dilemmas frequently arise from conflicts between these principles, most commonly pitting patient Autonomy against physician Beneficence (e.g., a patient refusing a life-saving treatment).
Ethical Theories - Duty vs. Outcomes
-
Deontology (Duty-Based)
- Focuses on inherent rightness/wrongness of an act, not its consequences.
- Associated with Immanuel Kant.
- An act is moral if it follows a universal rule (e.g., "do not lie," "do not steal").
- The physician's duty to the individual patient is paramount.
-
Consequentialism (Outcome-Based)
- Judges an act based on its results.
- Utilitarianism: A common form; seeks the "greatest good for the greatest number."
- An action is moral if it maximizes positive outcomes and minimizes harm for the largest group.
⭐ In clinical dilemmas, Deontology prioritizes individual patient duties (e.g., confidentiality), while Utilitarianism might justify breaking that duty for a greater public good (e.g., warning others of a direct threat).
Practical Application - Consent & Capacity
- Informed Consent: A process ensuring patient voluntarism & autonomy. Not just a form.
- 📌 BRAIN: Benefits, Risks, Alternatives, Implications of No treatment.
- Exceptions: Emergencies, waiver, therapeutic privilege (rare), incapacity.
- Decision-Making Capacity: A clinical assessment; competence is a legal term.
- Assessed if a patient refuses recommended treatment or makes questionable decisions.
- Requires the patient to:
- Communicate a choice.
- Understand relevant information.
- Appreciate the situation & consequences.
- Reason about treatment options.
⭐ A patient with capacity has the right to refuse any medical treatment, including life-sustaining therapy, even if it results in death. This is a cornerstone of patient autonomy.
High‑Yield Points - ⚡ Biggest Takeaways
- Beneficence (act in patient's best interest) and Non-maleficence (do no harm) are core duties.
- Autonomy respects a patient's right to make informed decisions about their own body.
- Justice ensures fair allocation of healthcare resources and equitable treatment.
- Informed consent is a process, not just a signature; requires decision-making capacity.
- Confidentiality is paramount but can be breached to prevent serious harm to self or others.
- Ethical dilemmas often involve conflicts between these fundamental principles.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

