Rejection Timelines - The Graft's Clock
- Hyperacute (Minutes-Hours): Pre-formed anti-donor Abs (Type II HSR) → widespread thrombosis, fibrinoid necrosis.
- Acute (<6 months):
- Cellular (Type IV HSR): Lymphocytic infiltrate of tubules & interstitium (tubulitis).
- Humoral (Type II HSR): C4d deposition, neutrophilic glomerulitis, vasculitis.
- Chronic (>6 months): Irreversible fibrosis & atrophy.
- Vascular intimal fibrosis, glomerulosclerosis, tubular atrophy.
⭐ Acute cellular rejection is the most common type of rejection and typically responds well to immunosuppressants.
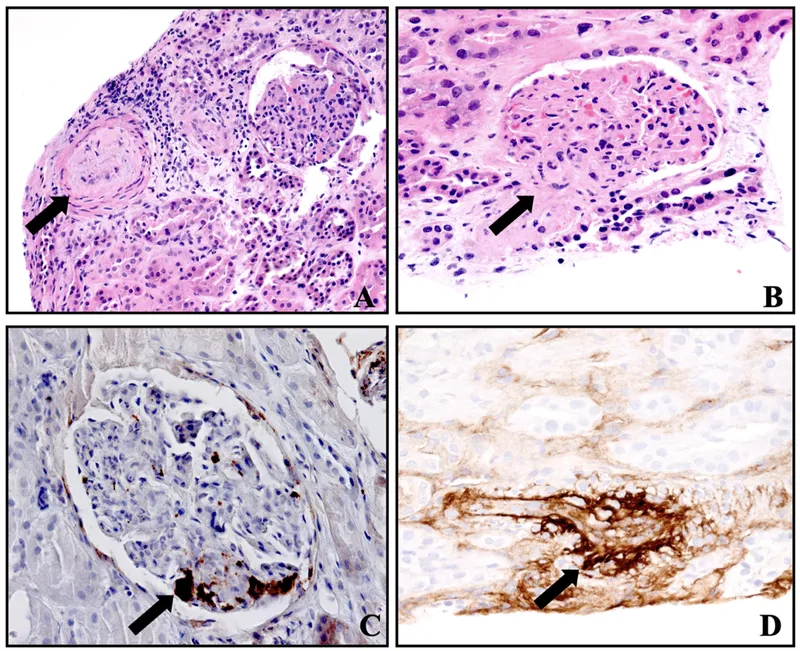
Acute Rejection - The Early Battle
-
Timeline: Typically occurs <6 months post-transplant.
-
Presentation: ↑ Serum Creatinine, oliguria, fever, graft pain/swelling.
-
Two Main Types:
- Acute Cellular Rejection (ACR): T-cell mediated (Type IV HSR).
- Path: Interstitial inflammation & tubulitis (lymphocytic invasion of tubular epithelium).
- Grading: Banff classification (t-score, i-score).
- Antibody-Mediated Rejection (AMR): Antibody-driven (Type II HSR).
- Path: Microvascular inflammation (glomerulitis, capillaritis), C4d deposition in peritubular capillaries.
- Requires presence of Donor-Specific Antibodies (DSAs).
- Acute Cellular Rejection (ACR): T-cell mediated (Type IV HSR).
⭐ C4d staining in peritubular capillaries is a key histological marker for active, antibody-mediated rejection.
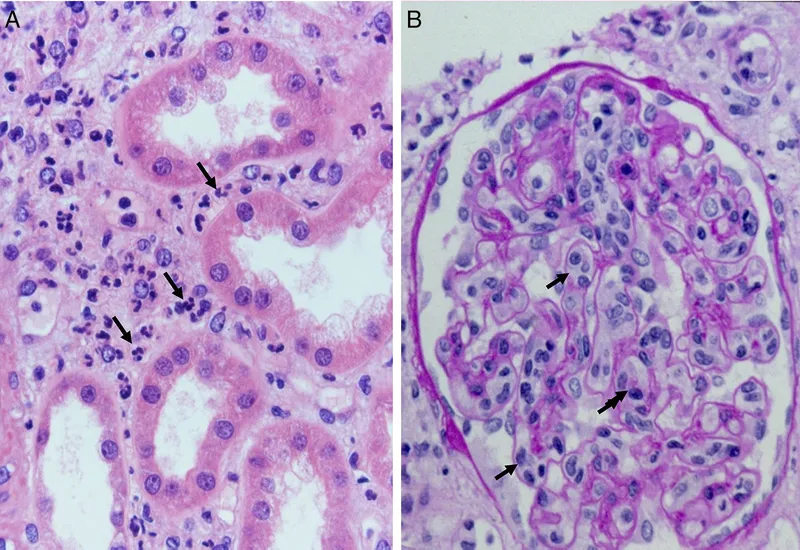
Chronic Rejection - The Slow Fade
- Timeline: Months to years post-transplant; insidious onset.
- Pathophysiology: Slow, progressive T-cell and/or antibody-mediated injury, leading to irreversible structural damage.
- Hallmark Pathology: Chronic allograft vasculopathy.
- Vessels: Concentric intimal fibrosis & smooth muscle proliferation → arterial occlusion.
- Glomeruli: Chronic transplant glomerulopathy (double contours).
- Tubules/Interstitium: Tubular atrophy and interstitial fibrosis (IF/TA).
- Clinical: Gradual ↑ serum creatinine, new or worsening hypertension, proteinuria.
- Outcome: Irreversible graft dysfunction leading to eventual graft loss.
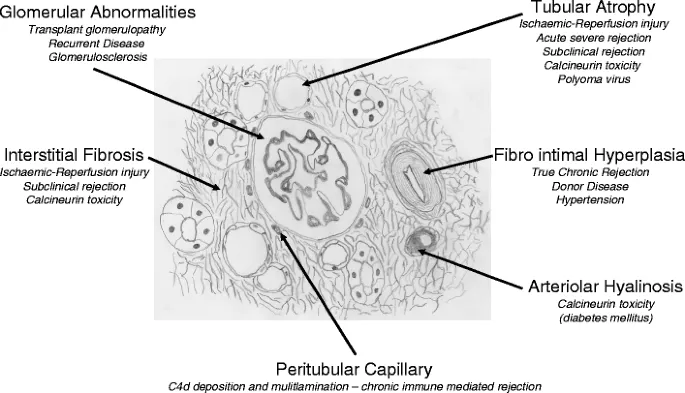
⭐ High-Yield: Chronic antibody-mediated rejection is often associated with the presence of donor-specific antibodies (DSAs), particularly against HLA class II antigens, and C4d deposition in peritubular capillaries.
Other Complications - Rogues' Gallery
- Recurrent Glomerulonephritis (GN):
- Primary disease returns to haunt the allograft.
- Most common: IgA Nephropathy, Membranoproliferative GN (MPGN), Focal Segmental Glomerulosclerosis (FSGS).
- FSGS recurrence can be rapid (days to weeks) with massive proteinuria.
- De Novo Glomerulonephritis:
- New glomerular disease in the allograft.
- Most common: Membranous nephropathy.
- Calcineurin Inhibitor (CNI) Toxicity (e.g., Tacrolimus, Cyclosporine):
- Acute: Toxic acute tubulopathy with isometric vacuolization of proximal tubules.
- Chronic: Arteriolar hyalinosis, striped cortical fibrosis, and tubular atrophy.
- Post-Transplant Lymphoproliferative Disorder (PTLD):
- Uncontrolled proliferation of B-lymphocytes, strongly associated with Epstein-Barr Virus (EBV) infection.
- Spectrum: from polyclonal hyperplasia to monoclonal lymphoma.
⭐ Chronic allograft nephropathy is the leading cause of graft loss after the first year, representing the final common pathway of chronic injury (rejection, CNI toxicity, hypertension).
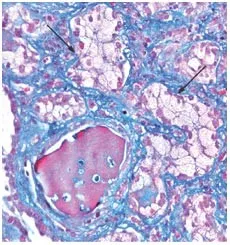
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection: Immediate thrombosis & necrosis from pre-formed anti-donor antibodies.
- Acute rejection: Weeks to months post-transplant; either cellular (T-cell infiltrate) or humoral (C4d deposition).
- Chronic rejection: Months to years; leads to vascular intimal fibrosis, glomerulosclerosis, and interstitial fibrosis.
- BK virus nephropathy: Mimics rejection; diagnosed by intranuclear viral inclusions in tubular cells.
- Calcineurin inhibitor toxicity: Key cause of non-rejection dysfunction; shows arteriolar hyalinosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

