Embryology & Overview - Lung Budding Gone Wild
- Origin: Respiratory diverticulum (lung bud) arises from the ventral foregut endoderm around week 4.
- Separation: The tracheoesophageal septum partitions the foregut into the dorsal esophagus and ventral trachea.
- Errors: Faulty partitioning leads to tracheoesophageal fistulas (TEF); abnormal budding causes bronchogenic cysts, sequestration, or agenesis.
⭐ Most common TEF: Esophageal atresia with a distal tracheoesophageal fistula (~85% of cases). This presents with polyhydramnios in utero, and choking/aspiration upon first feeding.

Pulmonary Sequestration - Rogue Lung Tissue
- Non-functional lung tissue with no connection to the bronchial tree.
- Receives arterial blood from systemic circulation (e.g., aorta), not pulmonary arteries.
-
Intralobar (ILS):
- More common (~85%).
- Located within a normal lung lobe; shares visceral pleura.
- Presents in adults with recurrent, localized pneumonia.
- Venous drainage: Pulmonary veins.
-
Extralobar (ELS):
- Less common (~15%).
- Located outside normal lung; has its own pleura.
- Presents in infants, often with other anomalies (e.g., diaphragmatic hernia).
- Venous drainage: Systemic veins (e.g., azygous).
⭐ The hallmark is an anomalous systemic artery supplying the sequestered segment, most commonly arising from the thoracic or abdominal aorta.

CPAM & Bronchogenic Cysts - Airway Malformation Mayhem
- Congenital Pulmonary Airway Malformation (CPAM):
- Hamartomatous mass of cystic lung tissue; communicates with airway.
- Presents as neonatal respiratory distress or recurrent infections.
- CXR/CT shows a multicystic, air-filled lesion.
- Bronchogenic Cyst:
- Arises from abnormal ventral foregut budding; does NOT communicate with airway.
- Typically a fluid-filled, unilocular cyst in the mediastinum.
- Can cause compressive symptoms (dyspnea, dysphagia).
⭐ While most CPAMs are benign, they carry a risk of malignant transformation to pleuropulmonary blastoma, especially Type 4.
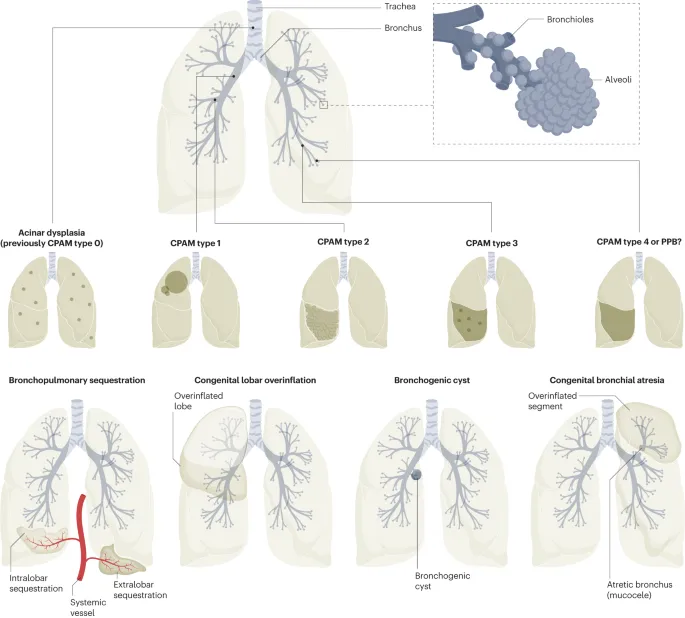
Congenital Lobar Overinflation - One-Way Air Trap
- Pathophysiology: Ball-valve bronchial obstruction leads to progressive lobar air-trapping and hyperinflation. Often from defective bronchial cartilage (~50% of cases) or extrinsic compression.
- Presentation: Neonatal respiratory distress, wheezing, cyanosis.
- Common Lobes: LUL > RML > RUL.
- Diagnosis:
- CXR: Hyperlucent lobe, mediastinal shift away from the affected side, atelectasis of adjacent lobes.
- CT confirms diagnosis.
- Management: Surgical lobectomy is the definitive treatment.
⭐ Unlike a simple pneumothorax, CLO causes severe mediastinal compression, risking cardiovascular collapse; it's a surgical emergency.

High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary sequestration is non-functional lung tissue lacking connection to the airway and pulmonary artery, receiving systemic arterial supply.
- Bronchogenic cysts are mediastinal masses from abnormal foregut budding that can become secondarily infected.
- CPAM is a hamartomatous lesion presenting with respiratory distress and a risk of malignant transformation.
- Pulmonary hypoplasia is frequently secondary to congenital diaphragmatic hernia or severe oligohydramnios.
- Intralobar sequestration drains to pulmonary veins; extralobar sequestration drains into the systemic venous system.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

