Bronchiectasis - Widened Airways Woes
- Patho: Permanent, abnormal bronchial dilation from necrotizing inflammation, creating a vicious cycle of infection and damage.
-
Etiologies:
- Cystic Fibrosis (severe cases)
- Infections (Aspergillus, NTM)
- Obstruction (tumor)
- Primary Ciliary Dyskinesia (e.g., Kartagener)
-
Clinical:
- Copious, purulent, foul-smelling sputum
- Hemoptysis, persistent cough
-
Diagnosis:
- High-Resolution CT (HRCT) is key.
- Shows "tram tracks," signet ring sign (bronchus > artery).
⭐ High-Yield: Kartagener syndrome presents with situs inversus, chronic sinusitis, and bronchiectasis due to a dynein arm defect causing primary ciliary dyskinesia.
- Tx: Chest physiotherapy, antibiotics for exacerbations.
Etiology - The Root Causes
-
Infectious Insults (50% of non-CF cases)
- Severe pneumonia (bacterial, viral)
- Aspergillus fumigatus → Allergic Bronchopulmonary Aspergillosis (ABPA)
- Mycobacterium avium complex (MAC) → Lady Windermere Syndrome
-
Airway Obstruction
- Endobronchial tumors (carcinoid, carcinoma)
- Foreign body aspiration
-
Genetic & Systemic Disease
- Cystic Fibrosis (CFTR gene mutation)
- Primary Ciliary Dyskinesia (e.g., Kartagener's Syndrome)
- Immunodeficiency (e.g., Hypogammaglobulinemia)
- Autoimmune (Rheumatoid Arthritis, Sjögren's)
⭐ Cystic Fibrosis is the underlying cause in approximately 50% of all bronchiectasis cases in the US.
Signs & Diagnosis - The Cough Conundrum
- Clinical Picture: Persistent productive cough with copious, purulent, often foul-smelling sputum that may form three layers upon settling.
- Accompanied by dyspnea, pleuritic pain, and recurrent infections.
- Hemoptysis can be significant.
- Physical Exam: Persistent crackles, rhonchi, and wheezing at lung bases. Digital clubbing is a classic but late finding.
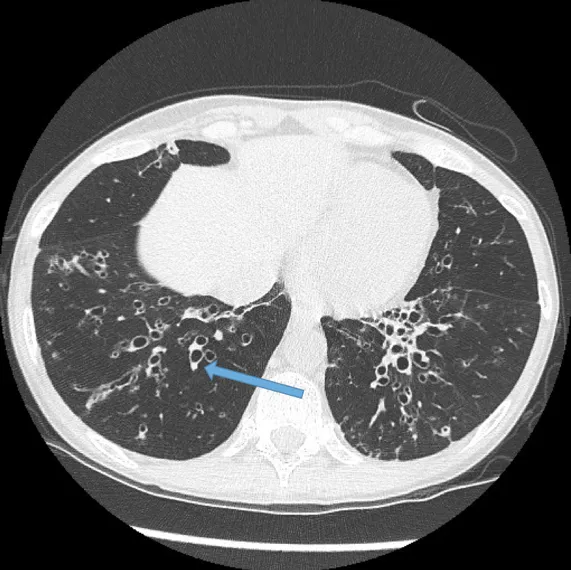
⭐ Exam Favorite: The "signet ring sign" on HRCT is the key diagnostic finding. It represents a dilated bronchus immediately adjacent to its smaller accompanying pulmonary artery branch.
Management - Taming the Tubes
- Cornerstone: Airway Clearance
- Chest physiotherapy (postural drainage, percussion).
- Mucolytics: Nebulized hypertonic saline; Dornase alfa (for CF-related).
- Bronchodilators (e.g., albuterol) before therapy.
- Treating Exacerbations
- Culture-guided antibiotics for 10-14 days.
- Empiric coverage for H. influenzae, S. pneumoniae, P. aeruginosa.
- Reducing Recurrence
- Consider long-term macrolides (e.g., azithromycin) for ≥3 exacerbations/year.
⭐ In bronchiectasis exacerbations, always cover for Pseudomonas aeruginosa, especially in patients with cystic fibrosis. It is a frequent and difficult-to-eradicate pathogen associated with more rapid lung function decline.
High‑Yield Points - ⚡ Biggest Takeaways
- Bronchiectasis is a permanent, irreversible dilation of the bronchi, most commonly due to necrotizing infections or underlying conditions like cystic fibrosis and Kartagener syndrome.
- The hallmark is a vicious cycle of inflammation and infection leading to progressive airway damage.
- Clinically, presents with a chronic cough producing copious, purulent, foul-smelling sputum, and frequent hemoptysis.
- High-resolution CT (HRCT) is the diagnostic gold standard, revealing characteristic "tram track" and "signet ring" signs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

