Atelectasis - The Collapsed Lung
- Definition: Lung collapse due to inadequate air space expansion, leading to a V/Q mismatch.
- Pathophysiology: Results in hypoxia; collapse can be partial or complete.
- Clinical Features: Dyspnea, cough, diminished breath sounds, dullness to percussion.
- Diagnosis: Chest X-ray shows opacification and volume loss.
⭐ High-Yield: In resorption atelectasis, the trachea and mediastinum deviate towards the collapsed lung. In compression atelectasis (e.g., tension pneumothorax), they deviate away.
Types & Causes - Why Lungs Deflate
- Resorption (Obstructive): Airway blockage (mucus plug, tumor) prevents ventilation. Trapped air is resorbed, collapsing the lung.
- Mediastinal shift toward the collapse.
- Compression: External force pushes air out. Caused by pleural effusion, pneumothorax, or tumor.
- Mediastinal shift away from the pressure source.
- Contraction (Cicatrization): Fibrotic changes in the lung or pleura prevent full expansion (e.g., post-TB, radiation).
- ⚠️ This type is irreversible.
- Microatelectasis: Loss of surfactant (e.g., in ARDS, NRDS) leads to widespread alveolar collapse.
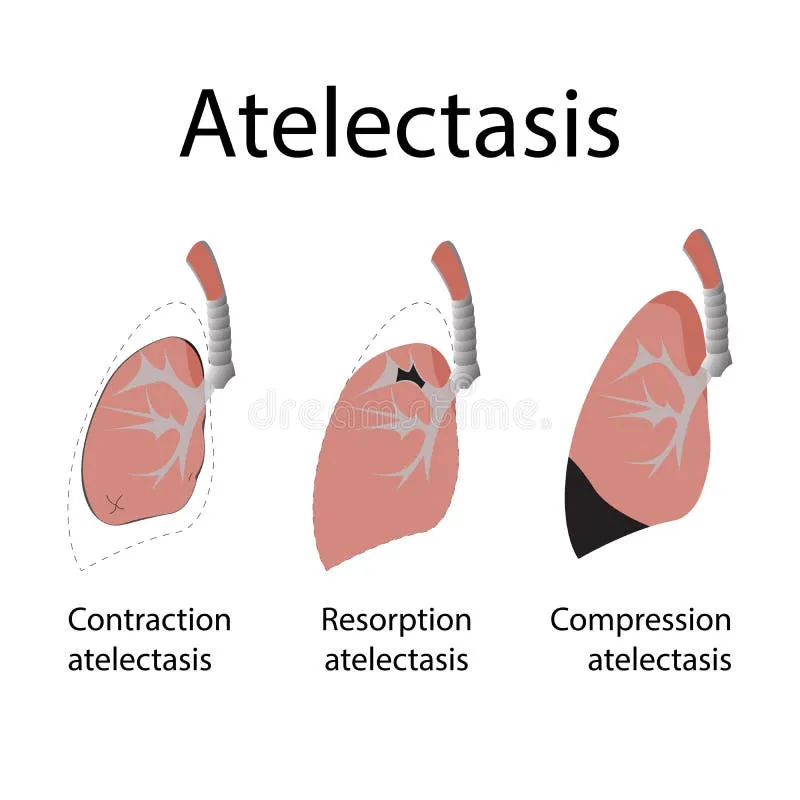
⭐ In resorption atelectasis, the mediastinum shifts toward the collapsed lung, a key radiological sign to differentiate it from compression atelectasis where it shifts away.
Clinical Picture - Spotting the Collapse
-
Symptoms: Often asymptomatic. If severe, may present with:
- Sudden-onset dyspnea & chest pain
- Cough, sputum production
-
Physical Exam: Key signs point to volume loss.
- Palpation: ↓ Tactile fremitus
- Percussion: Dullness over the affected area
- Auscultation: ↓ or absent breath sounds
⭐ On imaging, look for signs of volume loss: tracheal deviation towards the collapse, elevated hemidiaphragm, and crowding of ribs. This differentiates it from consolidation or effusion where the trachea is pushed away.
Management - Reinflating the Lung
- Primary Goal: Recruit and re-expand collapsed alveoli to improve ventilation/perfusion (V/Q) matching.
- Core Strategies (Non-invasive):
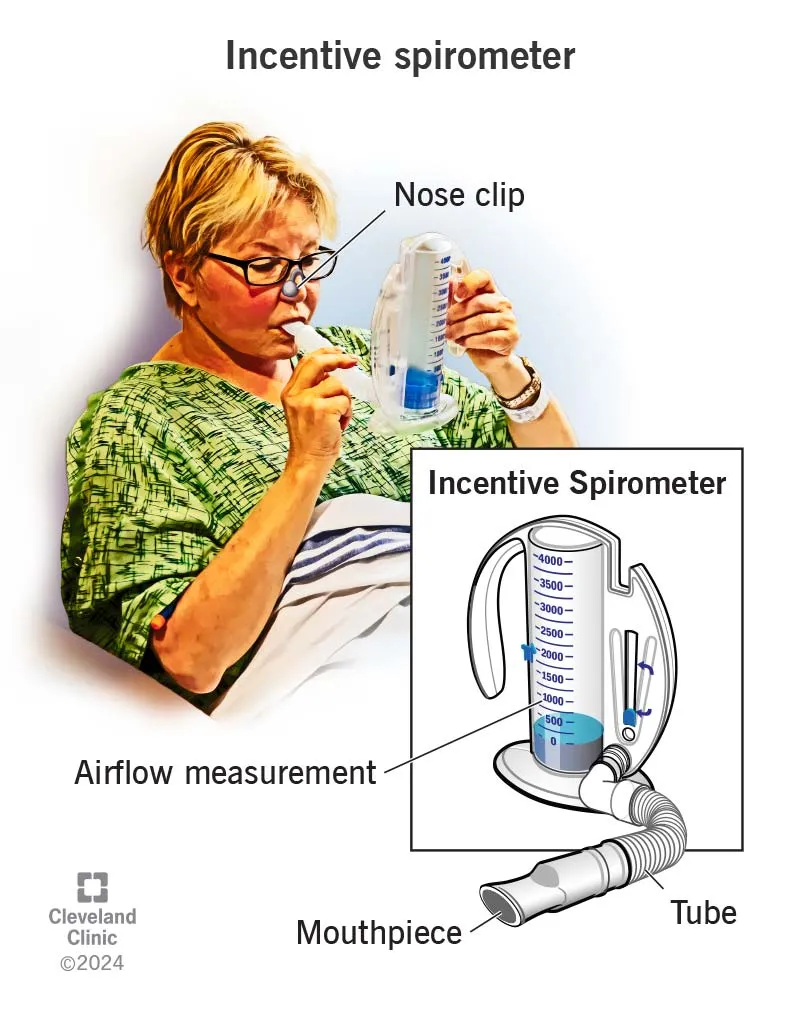
- Chest Physiotherapy: Incentive spirometry, deep breathing exercises, directed coughing, and postural drainage.
- Early Ambulation: Crucial post-operatively to promote deep inspiration.
- Pain Control: Adequate analgesia enables effective deep breaths and coughing.
- Advanced Measures:
- Positive Pressure: CPAP or PEEP via ventilation stents airways open.
- Therapeutic Bronchoscopy: For suctioning thick mucous plugs or removing foreign bodies.
⭐ Supplemental O₂ corrects hypoxemia but does not resolve the underlying atelectasis. High FiO₂ can worsen it by accelerating gas absorption from poorly ventilated alveoli (absorption atelectasis).
High‑Yield Points - ⚡ Biggest Takeaways
- Resorption atelectasis follows complete airway obstruction (e.g., mucus plug), pulling the mediastinum toward the collapse.
- Compression atelectasis is from external pressure (e.g., pleural effusion), pushing the mediastinum away.
- Contraction atelectasis, caused by pleural or parenchymal fibrosis, is the only irreversible form.
- Adhesive atelectasis stems from surfactant deficiency, the hallmark of Neonatal Respiratory Distress Syndrome.
- Key findings include decreased breath sounds, dullness to percussion, and ipsilateral tracheal deviation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

