Asthma Basics - The Wheezy Setup
- A chronic inflammatory disorder of the airways leading to reversible bronchoconstriction from bronchial hyperresponsiveness.
- Clinically presents with episodic wheezing, cough, and shortness of breath.
- Common Triggers:
- Allergens (e.g., pollen, dust mites)
- Viral respiratory infections
- Cold air, exercise
- Medications (Aspirin, β-blockers)
⭐ Atopic (extrinsic) asthma, the most common subtype, is a classic Type I Hypersensitivity reaction mediated by IgE, often with childhood onset.
Pathophysiology - Immune System Overdrive
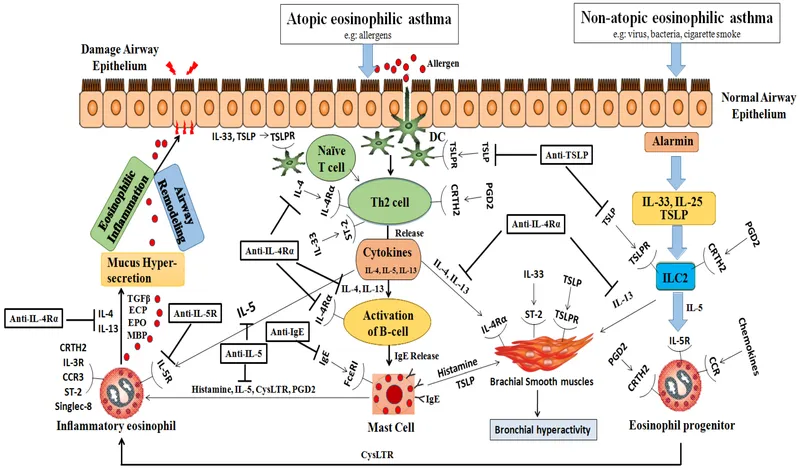
- Core Mechanism: A Type I Hypersensitivity reaction, driven by T-helper 2 (Th2) cells.
- Initial Sensitization: Allergen exposure prompts APCs to activate Th2 cells, stimulating B-cells to produce IgE, which coats mast cells.
Phases of Attack:
- Early Phase (Minutes): Re-exposure to allergen → IgE cross-linking on mast cells → degranulation. Releases histamine, leukotrienes (LTC₄, LTD₄, LTE₄) → potent bronchoconstriction, mucus production, and vasodilation.
- Late Phase (Hours): Cytokines (esp. IL-5) from Th2 cells recruit eosinophils. Eosinophils release major basic protein and eosinophilic cationic protein, damaging epithelium and amplifying inflammation.
⭐ Exam Favorite: Microscopic examination of sputum may reveal Curschmann spirals (whorled mucus plugs) and Charcot-Leyden crystals (crystalline aggregates of eosinophil proteins).
Gross & Microscopic - Airway Makeover Mess
-
Gross Findings
- Lungs are over-distended (hyperinflated) due to air trapping.
- Bronchi and bronchioles are occluded by thick, tenacious mucus plugs.
-
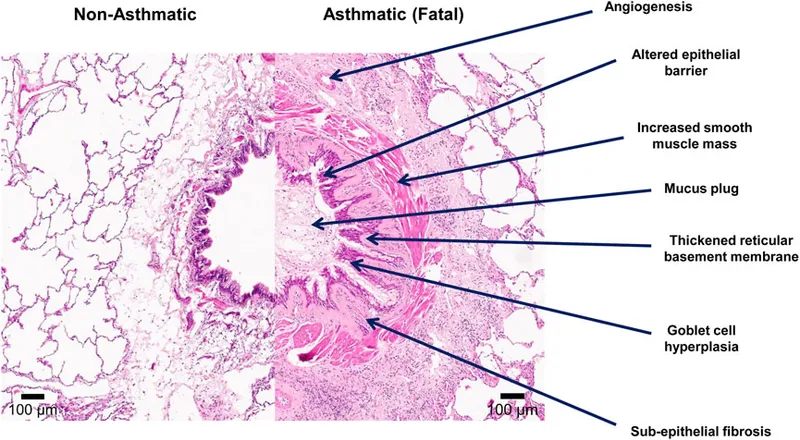
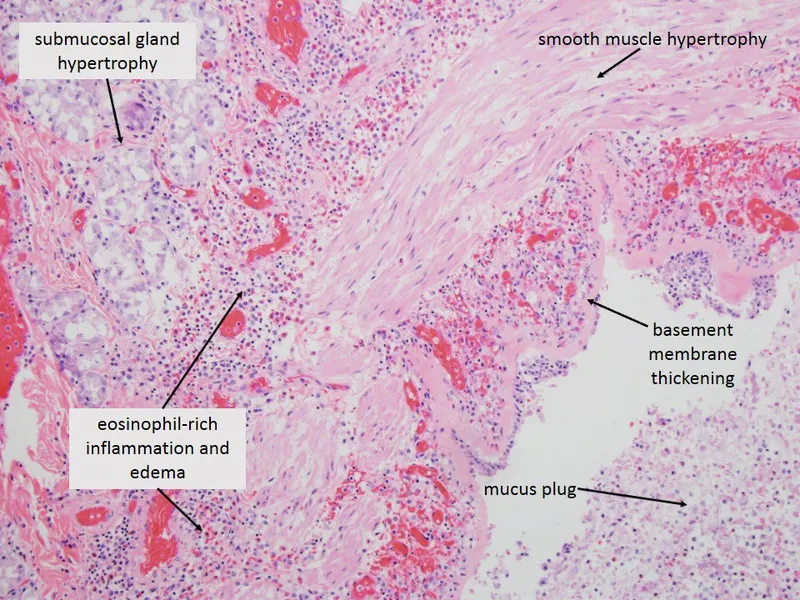
Microscopic Hallmarks (Airway Remodeling)
- Smooth muscle hypertrophy & hyperplasia (↑ muscle mass).
- Goblet cell hyperplasia in epithelium & submucosal gland hypertrophy (↑ mucus).
- Thickened basement membrane due to subepithelial fibrosis.
- Heavy inflammatory infiltrate, especially eosinophils and mast cells.
- Key Luminal Findings
- Curschmann spirals: Spiral-shaped mucus plugs from shed epithelium.
- Charcot-Leyden crystals: Eosinophil-derived, needle-shaped crystals.
⭐ Airway remodeling can cause a progressive, irreversible loss of lung function over time, mimicking some features of COPD.
Clinical Correlation - Symptoms & Status
- Classic Triad: Episodic wheezing, cough (esp. nocturnal), and dyspnea.
- Pathophysiologic Link:
- Bronchoconstriction → Expiratory wheeze.
- Mucus hypersecretion/Plugging → Airflow obstruction, chest tightness.
- Inflammation & Edema → Airway hyperresponsiveness to triggers.
- Status Asthmaticus:
- Severe, unremitting exacerbation; a medical emergency.
- Leads to respiratory muscle fatigue and potential failure.
- ⚠️ Ominous signs: "Silent chest" (no audible wheezing due to poor air entry), cyanosis, rising PaCO₂.
⭐ Pulsus Paradoxus: An exaggerated fall in systolic BP >10 mmHg during inspiration is a key indicator of severe asthma, reflecting negative intrathoracic pressure swings.
High‑Yield Points - ⚡ Biggest Takeaways
- Reversible bronchoconstriction is the cardinal feature, a result of profound airway hyperresponsiveness to various stimuli.
- Chronic inflammation is dominated by Th2 lymphocytes, eosinophils, and mast cell degranulation.
- Key histologic findings include Curschmann spirals (whorled mucus plugs) and Charcot-Leyden crystals (from eosinophil protein).
- Long-term airway remodeling features bronchial smooth muscle hypertrophy, sub-basement membrane fibrosis, and goblet cell hyperplasia.
- Most cases represent a Type I hypersensitivity reaction initiated by common environmental allergens.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

