Outcomes of Acute Inflammation - The Aftermath
- Complete Resolution: Ideal outcome with restoration of normal tissue architecture. Occurs with minimal damage and high regenerative capacity.
- Healing by Fibrosis (Scarring): Occurs after substantial tissue destruction or in non-regenerative tissues.
- Abscess Formation: A walled-off collection of pus (neutrophils & necrotic debris), typical of pyogenic bacterial infections.
- Progression to Chronic Inflammation: Results from persistent injurious stimuli or interference with normal healing.
⭐ Resolution is an active process mediated by specialized pro-resolving mediators (SPMs) like lipoxins, resolvins, and protectins.
Resolution's Key Players - The Clean-Up Crew
-
Macrophages (M2 Phenotype): The primary "clean-up" cells.
- Phagocytose apoptotic neutrophils & cellular debris.
- Secrete anti-inflammatory cytokines (e.g., TGF-β, IL-10).
- Produce growth factors to initiate tissue repair.
-
Specialized Pro-Resolving Mediators (SPMs): Actively terminate inflammation.
- Lipoxins: Generated via neutrophil-platelet interaction.
- Resolvins & Protectins: Derived from omega-3 fatty acids (EPA, DHA).
- Function: Inhibit neutrophil chemotaxis & adhesion; stimulate clearance of apoptotic cells.
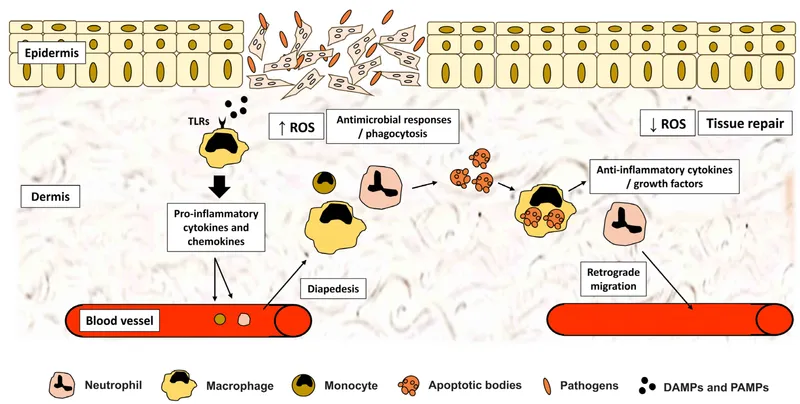
⭐ Macrophage Polarization: The switch from pro-inflammatory M1 macrophages to anti-inflammatory M2 macrophages is a critical step for inflammation to resolve and transition into a healing phase. This switch is driven by phagocytosis of apoptotic cells and cytokines like IL-4 and IL-13.
Mechanisms of Resolution - Winding It Down
- Active Termination: Resolution is an active, programmed process, not just a passive decay of the inflammatory response.
- Lipid Mediator Class Switch: A pivotal shift occurs from pro-inflammatory leukotrienes to anti-inflammatory lipoxins.
- This switch is initiated by neutrophils, which then undergo apoptosis.
- Specialized Pro-Resolving Mediators (SPMs):
- Includes Resolvins, Protectins, and Maresins, derived from omega-3 fatty acids.
- These molecules halt neutrophil influx and promote the clearance of apoptotic cells (efferocytosis).
- Cytokine Profile Change: Shift towards anti-inflammatory cytokines, primarily IL-10 and TGF-β.
⭐ The "lipid mediator class switch" is a core principle. Aspirin-triggered lipoxins are a key pharmacologic example, enhancing resolution by mimicking this natural pathway.
Failed Resolution - The Lingering Problem
- Failure of acute inflammation to resolve leads to:
- Abscess Formation: A collection of pus (neutrophils, necrotic debris) confined by a fibrous capsule. Typically caused by pyogenic organisms like S. aureus.
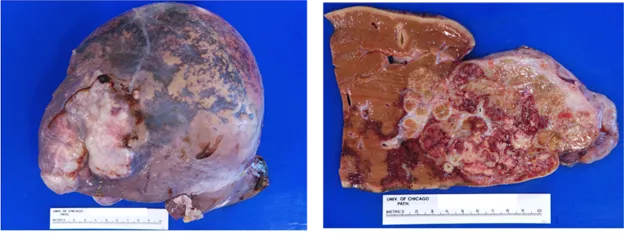
- Chronic Inflammation: Develops if the injurious agent persists, marked by an influx of lymphocytes and macrophages.
- Fibrosis (Scarring): Tissue replacement with collagen following substantial destruction, a process termed "organization," resulting in functional loss.
- Abscess Formation: A collection of pus (neutrophils, necrotic debris) confined by a fibrous capsule. Typically caused by pyogenic organisms like S. aureus.
⭐ The abscess capsule is produced by fibroblasts, a key feature distinguishing it from diffuse purulent inflammation (cellulitis).
High‑Yield Points - ⚡ Biggest Takeaways
- Complete resolution is the ideal outcome, where macrophages clear debris and restore normal tissue structure.
- Fibrosis (scarring) results from substantial tissue destruction or in non-regenerating tissues, mediated by fibroblasts.
- Abscess formation (pus) is characteristic of pyogenic bacterial infections, like Staphylococcus aureus.
- Progression to chronic inflammation occurs when the injurious agent persists, involving lymphocytes and macrophages.
- Key anti-inflammatory mediators driving resolution include lipoxins, resolvins, and cytokines like IL-10 and TGF-β.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

