Introduction - The Slow Burn
-
Prolonged inflammation (weeks to months) characterized by coexisting inflammation, tissue injury, and attempts at repair (fibrosis).
-
May follow acute inflammation or arise insidiously.
-
Key Cellular Players:
- Macrophages: Central conductors of the process.
- Lymphocytes: (T and B cells) provide specific immunity.
- Plasma cells: Produce antibodies.
-
Primary Causes:
- Persistent Infections: e.g., Tuberculosis, viral hepatitis.
- Hypersensitivity Diseases: e.g., Rheumatoid arthritis, Multiple Sclerosis.
- Prolonged Toxin Exposure: e.g., Silicosis (exogenous), Atherosclerosis (endogenous).
⭐ The histological hallmark is the replacement of normal tissue with inflammatory cells (mononuclear infiltrate) and fibrosis, reflecting simultaneous destruction and healing.
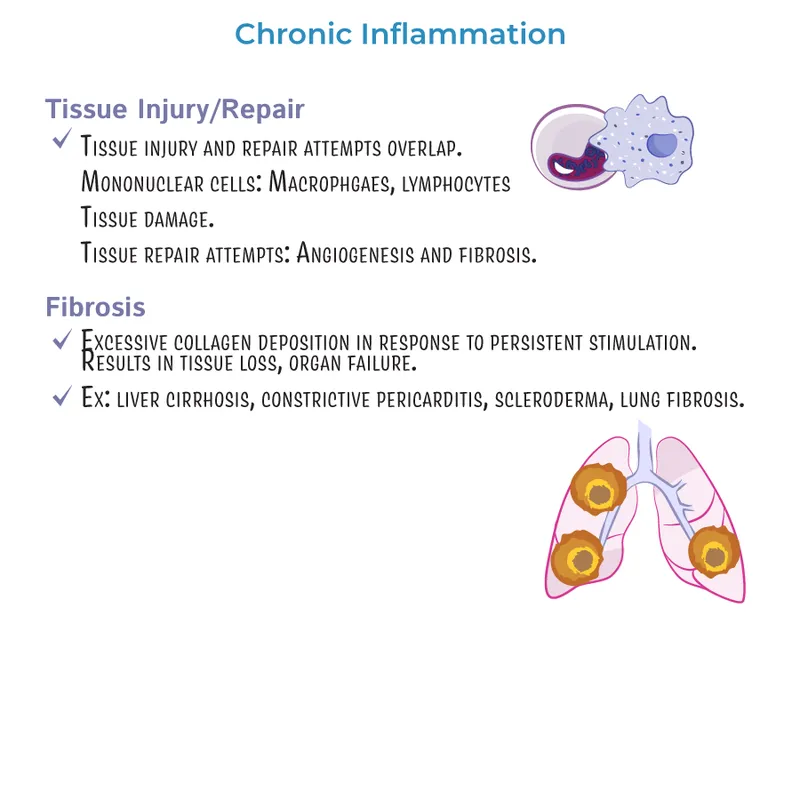
Key Cellular Players - The Usual Suspects
- Macrophages: The central conductors. Derived from circulating monocytes which extravasate into tissue.
- Classical (M1) Activation: Induced by microbial products & IFN-γ. Pro-inflammatory; phagocytosis & killing.
- Alternative (M2) Activation: Induced by IL-4 & IL-13. Anti-inflammatory; tissue repair & fibrosis.
- Lymphocytes (T & B cells): Mobilized for specific adaptive immunity. Create a feedback loop with macrophages.
- Plasma Cells: Terminally differentiated B-cells producing antibodies against persistent antigens.
- Eosinophils: Key in IgE-mediated reactions (allergies, asthma) and parasitic infections. Recruited by eotaxin.
- Mast Cells: Sentinel cells that release mediators (e.g., histamine) and cytokines, contributing to the inflammatory milieu.
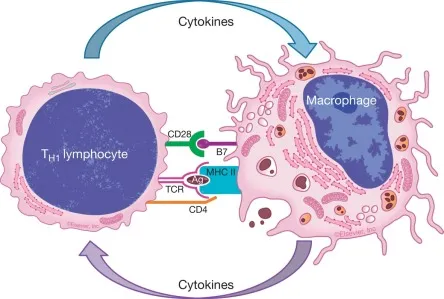
⭐ The IFN-γ / IL-12 Axis: Th1 cells secrete IFN-γ, the most potent activator of macrophages (M1 pathway). Activated macrophages, in turn, release IL-12, which promotes further Th1 differentiation, locking in the chronic response.
Granulomatous Inflammation - Walling Off Trouble
- A distinct pattern of chronic inflammation; an attempt to contain an offending agent that is difficult to eradicate.
- Key Cells: Aggregates of activated macrophages (epithelioid histiocytes); often with a collar of lymphocytes. Multinucleated giant cells (Langhans, foreign-body) are common.
- Pathogenesis:
- Driven by cytokines, primarily IFN-γ (from Tн1 cells) which activates macrophages, and TNF-α which sustains the granuloma.
- Types & Causes:
- Caseating: Central necrosis. Examples: Tuberculosis, fungal infections.
- Non-caseating: No necrosis. Examples: Sarcoidosis, Crohn disease, foreign body.
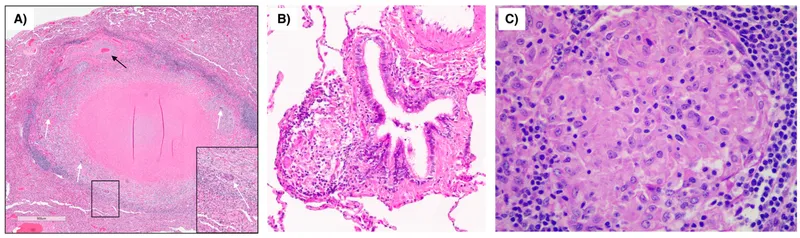
⭐ TNF-α is critical for maintaining granulomas. Patients on anti-TNF-α therapy (e.g., for rheumatoid arthritis) are at increased risk for reactivation of latent tuberculosis.
Systemic Effects - Body-Wide Fallout
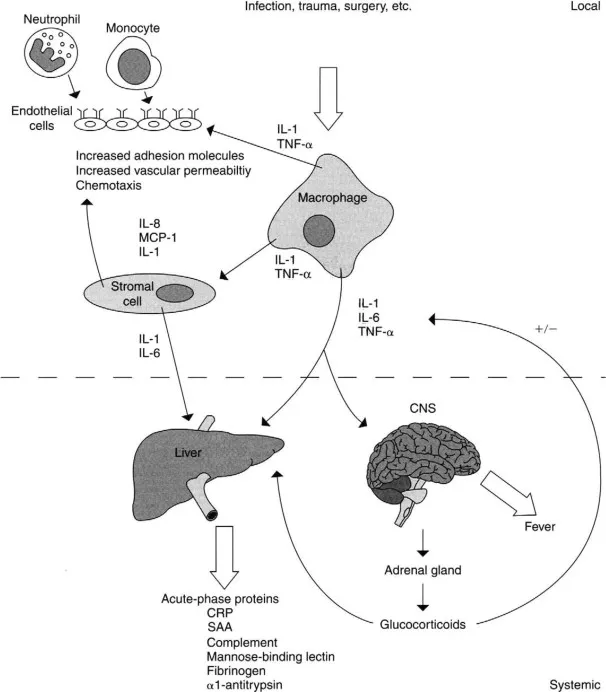
- Fever: Pyrogens (LPS) → Leukocytes release IL-1, TNF → Hypothalamus ↑ COX → ↑ PGE₂ → Resets temperature set-point.
- Acute-Phase Response: Liver synthesizes acute-phase proteins (APPs), driven mainly by IL-6.
- Positive (↑): C-reactive protein (CRP), Fibrinogen, Hepcidin, Serum Amyloid A (SAA).
- Negative (↓): Albumin, Transferrin.
- Leukocytosis: ↑ WBCs. Neutrophilia (bacterial), Lymphocytosis (viral), Eosinophilia (parasitic/allergic). "Left shift" indicates ↑ immature cells.
- Other: Anemia of chronic disease (↑ hepcidin), cachexia (TNF-α), septic shock (high TNF).
⭐ C-reactive protein (CRP) opsonizes pathogens and activates complement. Elevated CRP is a risk factor for myocardial infarction, linking inflammation to atherosclerosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Characterized by mononuclear cells: macrophages, lymphocytes, and plasma cells, not neutrophils.
- Caused by persistent infections (e.g., TB), prolonged exposure to toxic agents, or autoimmune reactions.
- Macrophages are the central players, activated by T-cell-derived IFN-γ.
- Hallmarks are concurrent tissue destruction and attempts at repair via angiogenesis and fibrosis.
- Granulomatous inflammation is a key subtype, featuring epithelioid macrophages and giant cells.
- Systemic effects like fever are driven by cytokines like TNF, IL-1, and IL-6.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

