T-Cell Activation - The Two-Signal Handshake
-
Signal 1 (Activation): T-cell receptor (TCR) on a naïve T-cell binds to an antigen presented by the Major Histocompatibility Complex (MHC) on an antigen-presenting cell (APC).
- CD4+ helper T-cells recognize MHC-II.
- CD8+ cytotoxic T-cells recognize MHC-I.
-
Signal 2 (Co-stimulation/Survival): A crucial safety check to prevent autoimmunity.
- CD28 protein on the T-cell binds to the B7 protein (CD80/CD86) on the APC.
⭐ Without Signal 2, T-cells become anergic (unresponsive) or undergo apoptosis. This is a key mechanism of peripheral tolerance.
Inhibitory Pathways - Pumping the Brakes
-
CTLA-4 Pathway (Cytotoxic T-Lymphocyte-Associated Protein 4):
- Location: Primarily acts in the lymph node during T-cell activation.
- Mechanism: CTLA-4 on T-cells has a higher affinity for B7 ligands (CD80/86) on antigen-presenting cells (APCs) than the co-stimulatory receptor CD28.
- Outcome: This competitive binding prevents T-cell co-stimulation, effectively ↓ T-cell activation.
-
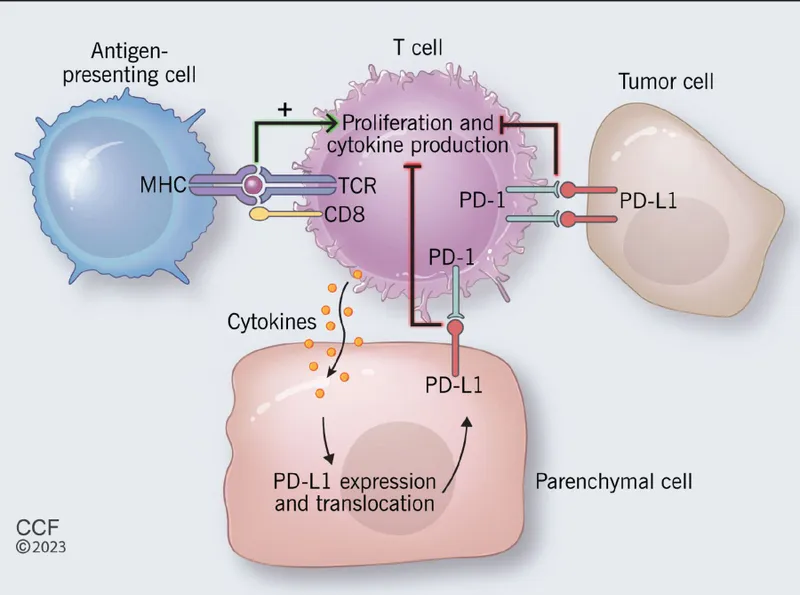
PD-1 Pathway (Programmed Cell Death Protein 1):
- Location: Functions later in peripheral tissues and the tumor microenvironment.
- Mechanism: PD-1 on activated T-cells binds to its ligands, PD-L1 and PD-L2. Tumor cells often upregulate PD-L1 to protect themselves.
- Outcome: Induces T-cell anergy or exhaustion, ↓ cytokine release, and suppresses cytotoxic T-cell activity.
⭐ Exam Favorite: CTLA-4 blockade acts earlier in the immune response (priming phase in lymph nodes), while PD-1/PD-L1 blockade acts later (effector phase in peripheral tissues).
Checkpoint Inhibitors - Releasing the Hounds
- Mechanism: Monoclonal antibodies that block inhibitory signals on T-cells, unleashing an anti-tumor immune response.
- CTLA-4 Blockade: Prevents CD28 co-stimulation negation. Primarily acts in lymph nodes.
- Drug: Ipilimumab
- PD-1/PD-L1 Blockade: Prevents T-cell "exhaustion" signal. Primarily acts in peripheral tissues.
- PD-1 Drugs: Nivolumab, Pembrolizumab
- PD-L1 Drugs: Atezolizumab, Durvalumab, Avelumab
- CTLA-4 Blockade: Prevents CD28 co-stimulation negation. Primarily acts in lymph nodes.
-
Clinical Use: Melanoma, Non-Small Cell Lung Cancer (NSCLC), Renal Cell Carcinoma (RCC), Bladder Cancer.
-
Adverse Effects (Immune-Related Adverse Events - irAEs):
- Common: Dermatitis, colitis (diarrhea), hepatitis, endocrinopathies (e.g., hypophysitis, thyroiditis), pneumonitis.
- 📌 "Ipi, Nivo, Pembro... itis!" - most side effects are inflammatory.
⭐ High-Yield: Management of immune-related adverse events (irAEs) often involves high-dose corticosteroids (e.g., prednisone) and temporary or permanent discontinuation of the checkpoint inhibitor.
High‑Yield Points - ⚡ Biggest Takeaways
- CTLA-4 and PD-1 are crucial inhibitory pathways that downregulate T-cell activation, preventing autoimmunity.
- CTLA-4 outcompetes the co-stimulatory molecule CD28 for its ligand, B7, on antigen-presenting cells.
- PD-1 on activated T-cells binds to PD-L1 on tumor cells, leading to T-cell exhaustion.
- Cancers exploit this by upregulating PD-L1 to hide from the immune system.
- Checkpoint inhibitors block these interactions, “releasing the brakes” on anti-tumor immunity.
- Their main toxicity is immune-related adverse events (irAEs) like colitis, dermatitis, and endocrinopathies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

