Type I HSR - Allergic Anarchy
- Mechanism: Immediate (Allergic, Anaphylactic), IgE-mediated degranulation of mast cells & basophils.
- Phases:
- Early (minutes): Antigen cross-links IgE → histamine release → vasodilation, edema.
- Late (hours): Eosinophils & inflammatory cells recruited → sustained inflammation.
- Examples: Allergic rhinitis, asthma, systemic anaphylaxis.
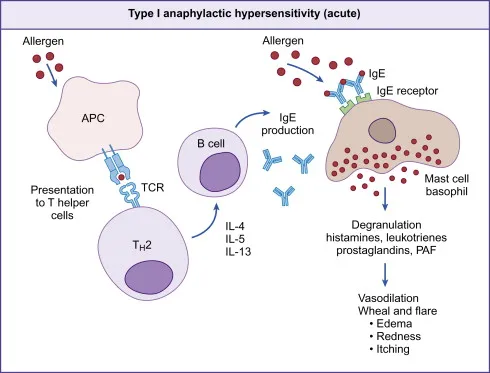
⭐ Tryptase is a specific marker for mast cell activation and can be measured in the blood to help diagnose anaphylaxis.
Type II HSR - Cytotoxic Crisis
- Mechanism: Antibody-mediated (IgG, IgM) destruction of cells or tissues. Antibodies bind to cell-surface or extracellular matrix antigens.
- Key Pathways:
- Complement activation → MAC complex → cell lysis.
- Opsonization & phagocytosis by macrophages.
- Antibody-dependent cell-mediated cytotoxicity (ADCC) by NK cells.
- Clinical Examples:
- Autoimmune hemolytic anemia, Goodpasture syndrome, Rheumatic fever.
- Receptor-specific: Myasthenia gravis (blocking), Graves' disease (stimulating).
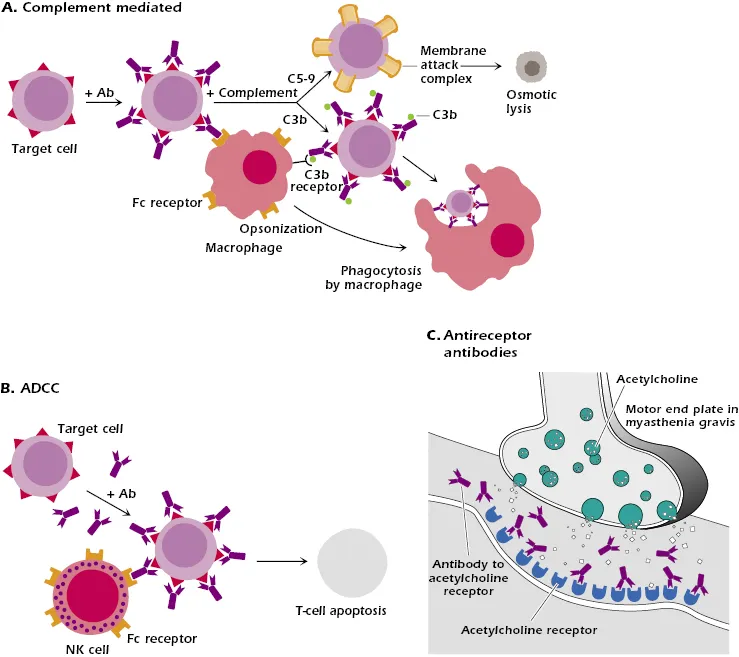
⭐ The Coombs test is crucial for diagnosis. Direct detects antibodies bound to RBCs; indirect detects anti-RBC antibodies in the patient's serum.
Type III HSR - Complex Chaos
- Mechanism: Antigen-antibody (IgG) complexes form in circulation → deposit in tissues (e.g., vessels, glomeruli) → activate complement.
- Pathology:
- Complement (C3a, C5a) attracts neutrophils.
- Neutrophils release lysosomal enzymes → tissue damage (vasculitis, fibrinoid necrosis).
- Develops over 3-8 hours.
- Clinical Examples:
- Systemic: SLE, post-streptococcal glomerulonephritis, serum sickness.
- Local: Arthus reaction (e.g., after a booster vaccine).

⭐ Serum Sickness: A classic drug-induced Type III HSR. Drugs act as haptens, forming immune complexes. Presents with fever, urticaria, arthralgia, and proteinuria 1-2 weeks post-exposure.
Type IV HSR - Delayed Drama
- Mechanism: T-cell mediated (no antibodies); delayed onset (48-72 hrs).
- Pathways:
- Sensitization: Antigen-presenting cells (APCs) prime naive T-cells.
- Elicitation: Re-exposure → memory Th1 cells release IFN-γ → activates macrophages → inflammation.
- Clinical Forms: Contact dermatitis (poison ivy, nickel), tuberculin skin test (PPD), granulomas (TB, sarcoidosis).

⭐ The PPD test for tuberculosis is a classic example; the diameter of induration (palpable hardening), not just erythema, is measured.
Comparative Review - Reaction Roundup
📌 ACID Mnemonic: Anaphylactic (I), Cytotoxic (II), Immune Complex (III), Delayed (IV).
| Feature | Type I (Anaphylactic) | Type II (Cytotoxic) | Type III (Immune Complex) | Type IV (Delayed) |
|---|---|---|---|---|
| Mediator | IgE | IgG, IgM | Antigen-Ab Complexes | T-Cells, Macrophages |
| Onset | Minutes | Variable | 4-10 hours | 48-72 hours |
| Mechanism | Mast cell degranulation | Complement activation | Neutrophil recruitment | Cytokine-mediated inflammation |
| Examples | Asthma, Allergies | Goodpasture, AIHA | SLE, Serum Sickness | PPD test, Contact Dermatitis |
High‑Yield Points - ⚡ Biggest Takeaways
- Type I (Anaphylactic) is IgE-mediated; requires initial sensitization, then re-exposure causes mast cell degranulation.
- Type II (Cytotoxic) involves IgG/IgM against fixed cell-surface antigens, leading to complement-mediated damage.
- Type III (Immune Complex) results from deposition of circulating antigen-antibody complexes, causing vasculitis or nephritis.
- Type IV (Delayed-Type) is T-cell mediated; Th1 cells activate macrophages, causing a reaction in 48-72 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

