HIV Basics - The Immune Hijacker
- Virus: Retrovirus (Lentivirus) targeting immune cells.
- Primary Target: CD4+ T-helper lymphocytes. Macrophages and dendritic cells act as reservoirs.
- Key Glycoproteins:
-
- gp120: Binds to the CD4 receptor.
-
- gp41: Facilitates viral fusion and entry.
-
- Coreceptors: Requires CCR5 (macrophage-tropic) or CXCR4 (T-cell-tropic) for entry.
- Replication: Uses reverse transcriptase to convert viral RNA into DNA, which integrates into the host genome.
⭐ HIV establishes a latent reservoir by integrating its proviral DNA into the genome of long-lived memory T-cells, making it a lifelong, incurable infection.
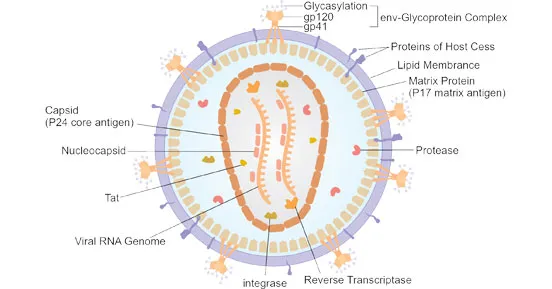
Pathogenesis - Immune System Takedown
- Primary Target: CD4+ T-helper lymphocytes, macrophages, and dendritic cells.
- Mechanism: Viral gp120 protein binds to the CD4 receptor and a coreceptor.
- Early Stage: CCR5 coreceptor (R5-tropic virus).
- Late Stage: CXCR4 coreceptor (X4-tropic virus).
- Consequence: Progressive depletion of CD4+ T-cells through viral replication, budding (lysis), and apoptosis.
- Immune Collapse: Leads to a critical drop in cell-mediated immunity, defined by a CD4+ count < 200 cells/mm³.
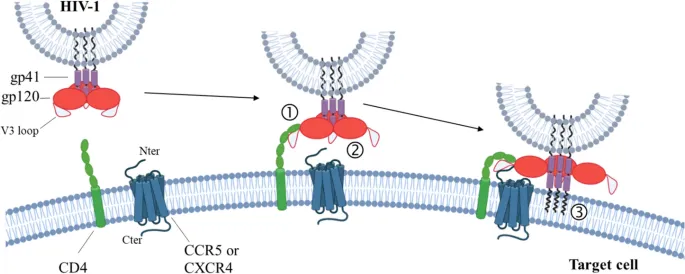
⭐ The CD4:CD8 ratio, normally ~2:1, inverts to <1:1 in AIDS, a key diagnostic indicator of immune dysregulation.
Diagnosis & Staging - Finding the Foe
- Screening: Sensitive ELISA detects anti-HIV (p24) antibodies & antigen.
- Confirmation: Specific Western blot (WB) or HIV-1/2 differentiation immunoassay.
- Viral Load: RT-PCR measures HIV RNA; used for monitoring treatment response and in acute infection.
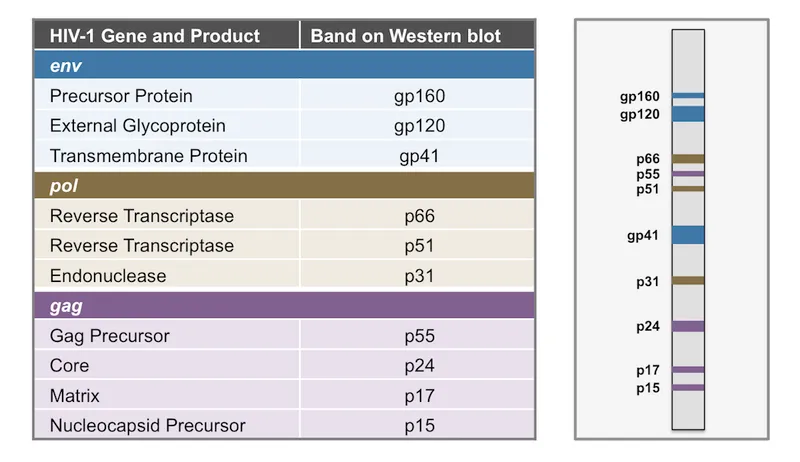
- Staging (CDC): Based on CD4+ T-cell count.
- Stage 1: > 500 cells/mm³
- Stage 2: 200-499 cells/mm³
- Stage 3 (AIDS): < 200 cells/mm³ or AIDS-defining illness.
⭐ Window Period: Time after infection when serology is negative as antibodies are not yet produced, but viral load (NAAT/PCR) is high and the patient is highly infectious.
Opportunistic Illnesses - When Defenses Fail
As CD4+ T-cell counts decline, the body becomes susceptible to a range of infections and malignancies. The specific opportunistic illness (OI) often correlates with the degree of immunosuppression.
-
General OIs: Candida albicans (oral thrush), EBV (oral hairy leukoplakia), HHV-8 (Kaposi sarcoma), Streptococcus pneumoniae (pneumonia).
-
Prophylaxis is key:
- CD4 < 200: Pneumocystis jirovecii pneumonia (PJP). Prophylaxis with TMP-SMX.
- CD4 < 100: Toxoplasma gondii, Cryptococcus neoformans.
- CD4 < 50: Mycobacterium avium complex (MAC). Prophylaxis with Azithromycin.
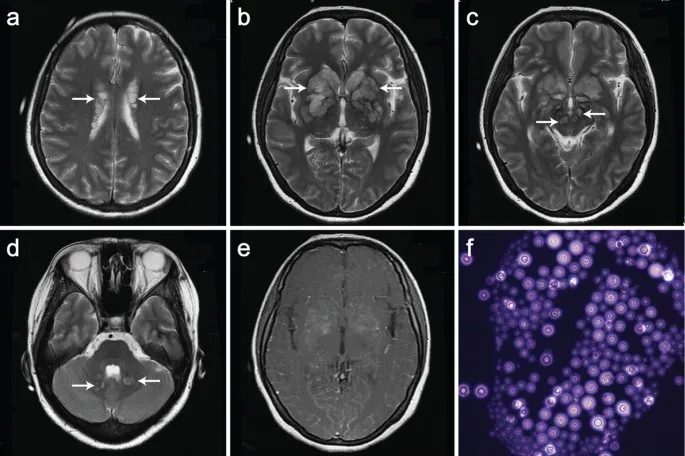
⭐ In an HIV+ patient with headache and fever, the most common cause of meningitis is Cryptococcus neoformans. Diagnosis is made via India ink stain or cryptococcal antigen test on CSF.
- HIV is a retrovirus that depletes CD4+ T-helper cells, causing profound immunosuppression.
- A CD4+ count < 200 cells/mm³ or an AIDS-defining illness confirms the diagnosis.
- High risk for opportunistic infections like Pneumocystis jirovecii pneumonia (PJP), CMV, and Toxoplasmosis.
- Associated malignancies include Kaposi's sarcoma (HHV-8) and EBV-related B-cell lymphomas.
- Neurologic complications like AIDS dementia complex and PML are common in advanced disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

