Coagulation Cascade - The Clotting Symphony
- Two main arms: Intrinsic (contact activation) and Extrinsic (tissue factor). They converge on the Common Pathway.
- Goal: Convert fibrinogen (Factor I) to a stable fibrin clot.
- Key Players: Vitamin K-dependent factors (II, VII, IX, X, Proteins C & S).
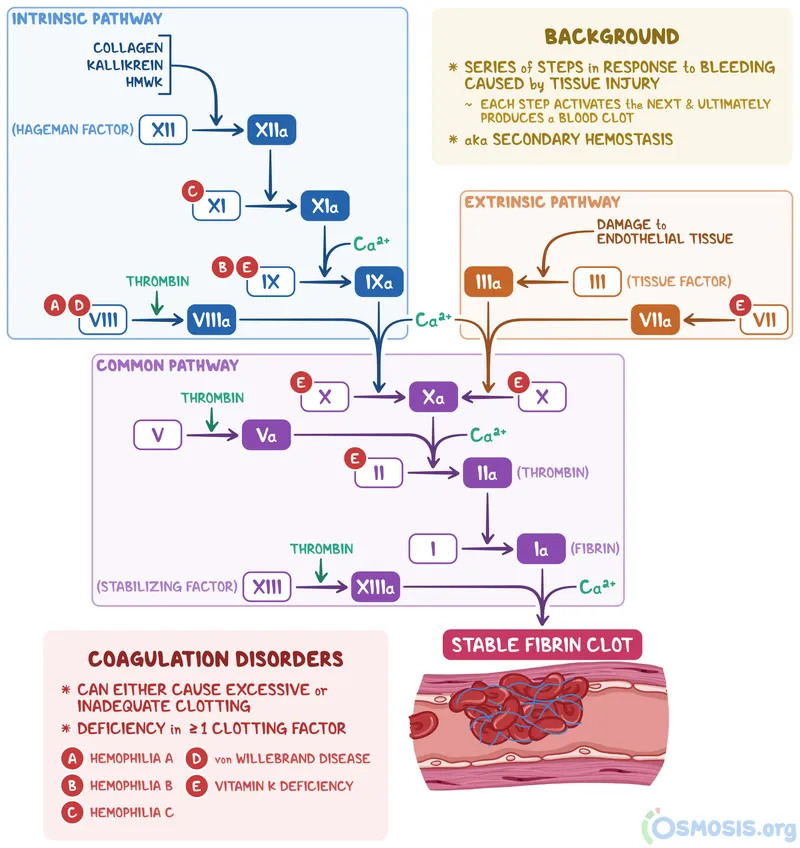
⭐ Calcium (Factor IV) is essential for the function of multiple clotting factors. Without it, the cascade grinds to a halt. This is why citrate is used in blood collection tubes to chelate calcium and prevent clotting.
📌 Mnemonic: The extrinsic pathway is initiated by factor 7 and is measured by PT (7 letters in "Extrinsic").
Primary Hemostasis - Platelet Problems
- Pathophysiology: Defective platelet plug formation, leading to mucocutaneous bleeding.
- Clinical Signs: Petechiae, purpura, ecchymoses, epistaxis, gingival bleeding. Prolonged bleeding time (BT).
-
Quantitative Disorders (Thrombocytopenia)
- Immune Thrombocytopenia (ITP): Anti-GpIIb/IIIa Abs → splenic destruction. Isolated ↓ platelets. Tx: corticosteroids, IVIG.
- Thrombotic Thrombocytopenic Purpura (TTP): Deficient ADAMTS13. Pentad: fever, MAHA, thrombocytopenia, renal/neuro signs.
-
Qualitative Disorders (Thrombocytopathy)
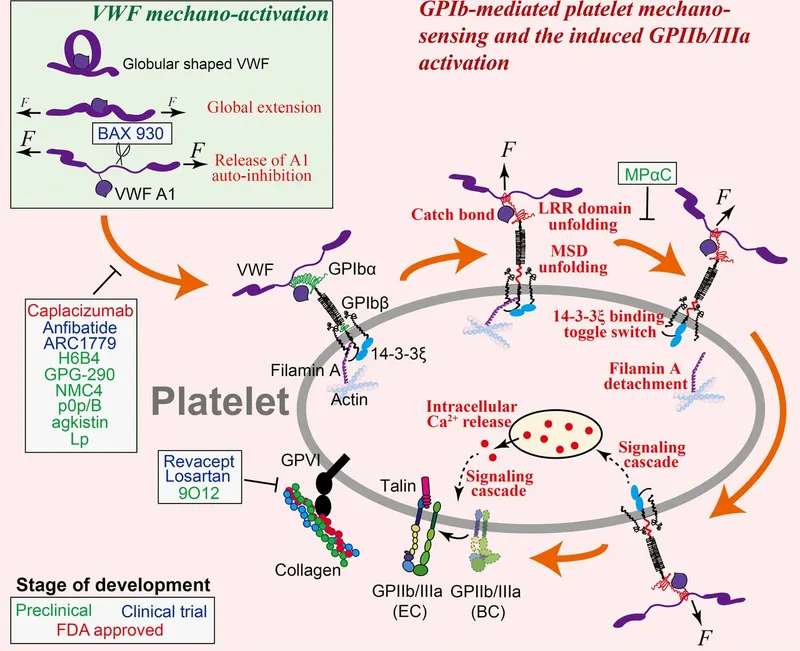
- Bernard-Soulier Syndrome: Deficient GpIb → impaired adhesion. Large platelets.
- Glanzmann Thrombasthenia: Deficient GpIIb/IIIa → impaired aggregation.
⭐ In TTP, plasma exchange is the emergent treatment of choice. Do not wait for the full pentad to manifest before initiating therapy.
Secondary Hemostasis - Factor Fiascos
- X-linked recessive disorders causing deep tissue bleeding & hemarthrosis.
- Hemophilia A: Factor VIII deficiency. Most common.
- Hemophilia B (Christmas Disease): Factor IX deficiency.
- Labs: ↑ PTT, normal PT & platelet count.
- Treatment: Desmopressin (for mild Hemophilia A), recombinant factor concentrates.
- Acquired Coagulopathy:
- Vitamin K Deficiency: ↓ Factors II, VII, IX, X, Protein C/S. ↑ PT (first) and PTT. Seen in liver disease, malabsorption, warfarin use.
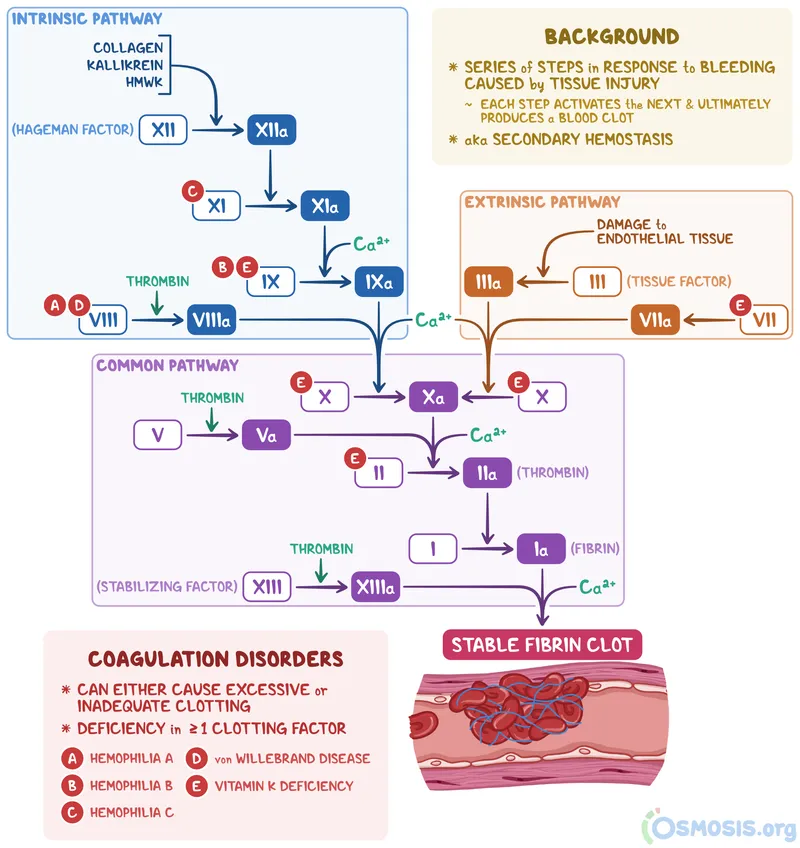
⭐ Mixing studies differentiate factor deficiency from a factor inhibitor. PTT/PT corrects with a deficiency but remains prolonged if an inhibitor (e.g., anti-FVIII antibody) is present.
Mixed Disorders - Clot & Bleed Chaos
- Disseminated Intravascular Coagulation (DIC): Widespread activation of coagulation leads to consumption of clotting factors & platelets, causing simultaneous thrombosis and hemorrhage.
- Triggers: 📌 Sepsis, Trauma, Obstetrics, Pancreatitis, Malignancy.
- Labs: ↑ PT/PTT, ↑ D-dimer, ↓ Platelets, ↓ Fibrinogen.
- Thrombotic Thrombocytopenic Purpura (TTP): Autoantibodies against ADAMTS13.
- Pentad: 📌 Fever, Anemia (MAHA), Thrombocytopenia, Renal failure, Neurologic symptoms.
- Hemolytic Uremic Syndrome (HUS): Endothelial damage by Shiga-like toxin (E. coli O157:H7).
- Triad: MAHA, Thrombocytopenia, Acute Kidney Injury.
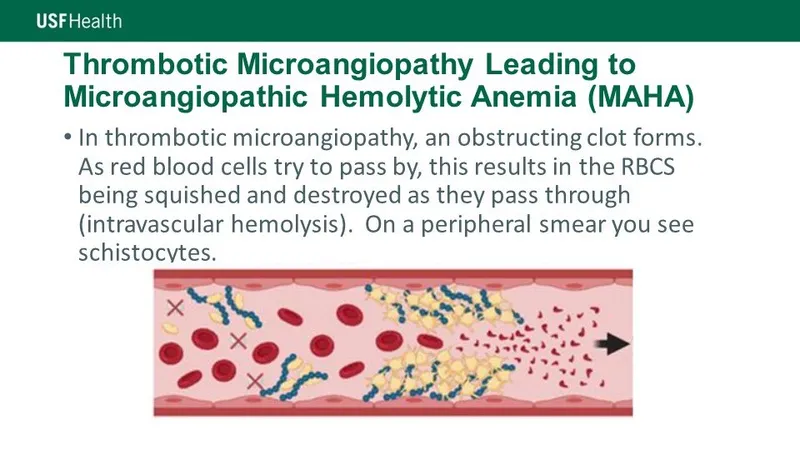
⭐ In TTP and HUS, coagulation studies (PT/PTT) are typically normal, distinguishing them from DIC where these are prolonged.
High‑Yield Points - ⚡ Biggest Takeaways
- Hemophilia A (Factor VIII) & B (Factor IX) are X-linked disorders causing deep tissue bleeding and an isolated ↑ PTT.
- Vitamin K deficiency (Factors II, VII, IX, X) and liver disease cause an ↑ in both PT and PTT.
- von Willebrand disease is the most common, an autosomal dominant defect in platelet adhesion causing mucocutaneous bleeding.
- DIC involves widespread clot consumption, leading to both thrombosis and hemorrhage with ↑ D-dimer and ↓ platelets.
- Platelet defects: Bernard-Soulier (adhesion, GpIb) vs. Glanzmann (aggregation, GpIIb/IIIa).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

