Edema & Effusions - Leaky Ship Fluids
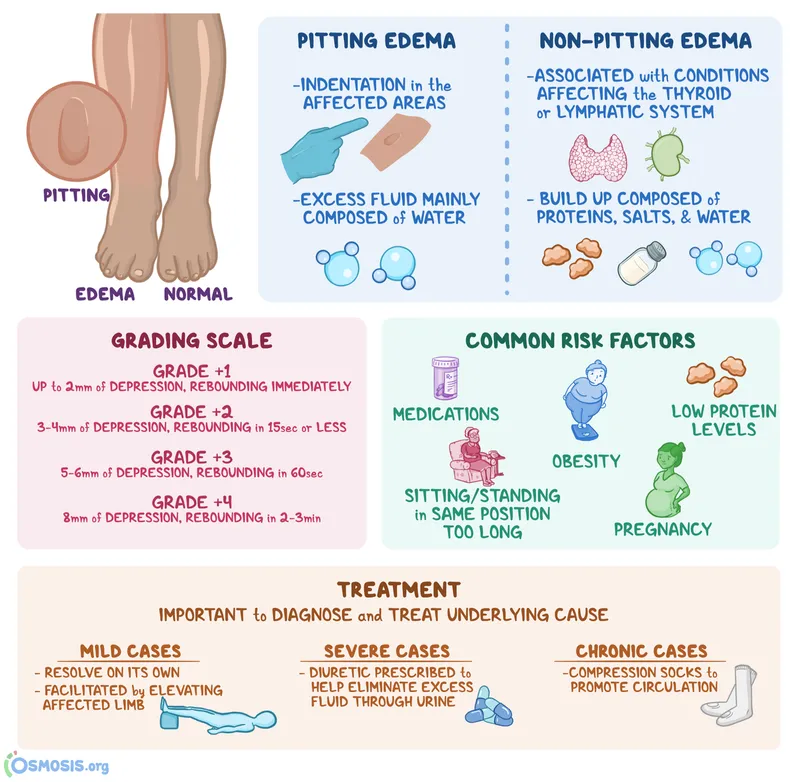
- Edema: Excess fluid in interstitial tissue; effusion is fluid in body cavities.
- Pathophysiology: Imbalance in Starling forces.
- ↑ Hydrostatic pressure (e.g., heart failure, DVT).
- ↓ Plasma oncotic pressure (e.g., nephrotic syndrome, liver failure).
- ↑ Capillary permeability (e.g., inflammation, burns).
- Lymphatic obstruction (lymphedema).
- Transudate: Protein-poor (<3 g/dL), SG <1.012. Pressure-driven.
- Exudate: Protein-rich (>3 g/dL), SG >1.020. Inflammation-driven.
⭐ Pulmonary edema, a classic sign of left-sided heart failure, presents with pink, frothy sputum and dyspnea.
Hyperemia & Congestion - Seeing Red
- Hyperemia: An active process from arteriolar dilation (e.g., exercise, inflammation).
- Leads to ↑ arterial inflow and erythema (redness).
- Congestion: A passive process from reduced venous outflow (e.g., heart failure, deep vein thrombosis).
- Leads to ↑ hydrostatic pressure, edema, and cyanosis.
- Chronic form causes hypoxia, scarring, and hemosiderin-laden macrophages (“heart failure cells” in lungs).
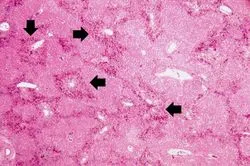
⭐ Chronic passive congestion of the liver (right-sided heart failure) creates a “nutmeg liver” appearance due to centrilobular necrosis, hemorrhage, and fatty change.
Thrombosis - Clotting Gone Wild
Pathological clot (thrombus) formation. Virchow's Triad outlines the causes:
- Endothelial Injury: The most critical factor. Caused by toxins, hypertension, inflammation.
- Abnormal Blood Flow: Stasis (e.g., atrial fibrillation) or turbulence (e.g., aneurysm) disrupts laminar flow.
- Hypercoagulability:
- Primary (Genetic): Factor V Leiden mutation.
- Secondary (Acquired): Malignancy, oral contraceptives, pregnancy.
⭐ Lines of Zahn-alternating pale (platelets, fibrin) and red (RBCs) layers-are hallmarks of a true thrombus formed in flowing blood.
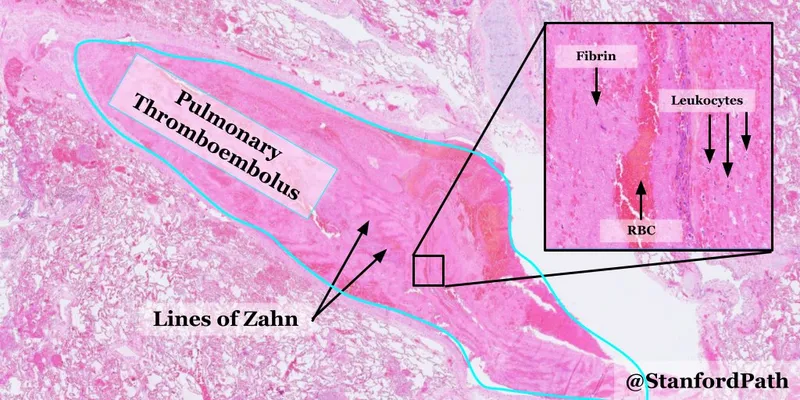
Embolism & Infarction - Deadly Traffic Jams
- Embolism: Intravascular mass that travels downstream to obstruct a vessel.
- Over 99% are thromboemboli (dislodged thrombus).
- Types: Fat, Air, Thrombus, Bacteria, Amniotic fluid, Tumor (📌 Mnemonic: FAT BAT).
- Pulmonary Embolism (PE): Most originate from deep vein thrombosis (DVT) in the legs.
- Infarction: Ischemic necrosis caused by vascular occlusion.
- Red (Hemorrhagic): Occurs in tissues with dual blood supply (e.g., lung, liver).
- White (Anemic): Occurs in solid organs with end-arterial circulation (e.g., heart, kidney).
⭐ The lung's dual circulation (pulmonary and bronchial arteries) means most PEs cause hemorrhage but not infarction in healthy individuals.
Shock - The Final Shutdown
Systemic hypoperfusion from ↓ cardiac output or ↓ effective circulating blood volume, leading to cellular hypoxia & organ failure.
- Stages of Shock:
- Non-progressive (Compensated): Reflex neurohumoral mechanisms (e.g., tachycardia, vasoconstriction) maintain vital organ perfusion.
- Progressive: Widespread tissue hypoxia. Cells switch to anaerobic glycolysis, causing lactic acidosis & ↓ blood pH.
- Irreversible: Severe cellular/tissue injury. Even with hemodynamic correction, survival is not possible.
⭐ In the irreversible stage of shock, lysosomal enzyme leakage contributes to widespread cellular necrosis, making organ damage permanent and recovery impossible.
- Edema results from ↑ hydrostatic pressure, ↓ oncotic pressure, or lymphatic obstruction; transudate is protein-poor, while exudate is protein-rich.
- Virchow's triad (endothelial injury, abnormal blood flow, hypercoagulability) is fundamental to thrombosis.
- The most common pulmonary embolism (PE) arises from a lower extremity deep vein thrombosis (DVT).
- Red (hemorrhagic) infarcts occur in tissues with dual blood supplies (e.g., lung), while white (anemic) infarcts affect solid organs (e.g., heart, kidney).
- Shock is systemic hypoperfusion; septic shock is characterized by peripheral vasodilation and is a high-mortality state.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

