Pituitary Anatomy - Command Center
- Location: Protected within the sella turcica of the sphenoid bone.
- Lobes & Embryology:
- Anterior (Adenohypophysis): From oral ectoderm (Rathke's pouch).
- Posterior (Neurohypophysis): From neuroectoderm.
- Anterior Pituitary Hormones: 📌 FLAT PEG
- Tropic: FSH, LH, ACTH, TSH
- Direct: Prolactin, Endorphins, GH
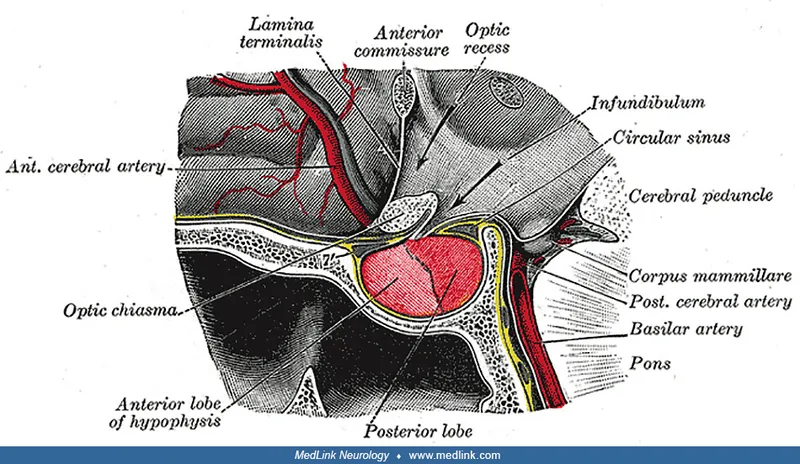
⭐ Pituitary adenomas can compress the optic chiasm superiorly, causing classic bitemporal hemianopsia.
Pituitary Adenomas - Hyperactive Hormones
-
Prolactinoma (Most Common):
- Secretes ↑ Prolactin → Galactorrhea & amenorrhea (females), ↓ libido & infertility (males).
- Dx: ↑ serum prolactin.
- Rx: Dopamine agonists (e.g., Cabergoline, Bromocriptine).
-
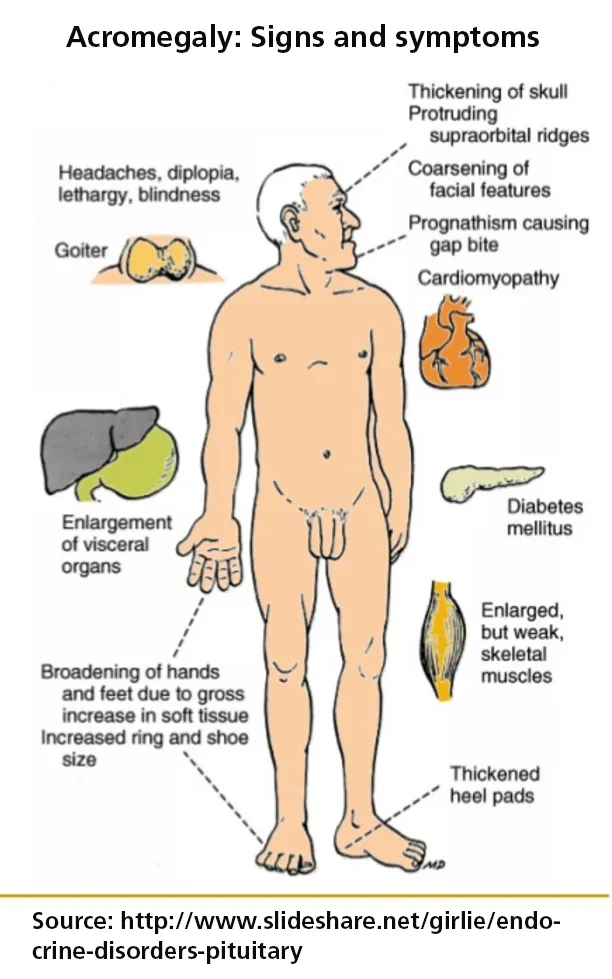
Somatotroph Adenoma (↑ GH):
- Acromegaly (Adults): Large hands/feet, coarse facial features, insulin resistance.
- Gigantism (Children): ↑ linear growth before epiphyseal closure.
- Dx: ↑ IGF-1; failure of GH suppression with oral glucose tolerance test.
-
Corticotroph Adenoma (↑ ACTH):
- Cushing's Disease: The specific cause of Cushing's syndrome due to a pituitary adenoma.
- Dx: ↑ 24-hr urine free cortisol; failure of low-dose dexamethasone suppression.
⭐ Nelson Syndrome: Post-bilateral adrenalectomy, a pre-existing corticotroph adenoma grows rapidly. Presents with mass effects and hyperpigmentation (↑ MSH).
Posterior Pituitary - Wet or Dry
-
SIADH (Wet - ↑ ADH): Euvolemic hyponatremia.
- Causes: Ectopic (Small cell lung cancer), CNS trauma, drugs.
- Labs: ↓ Serum Osm, ↑ Urine Osm (>100 mOsm/kg), ↑ Urine Na+ (>40 mEq/L).
- 📌 Small cell, Increased ADH, Dilutional Hyponatremia.
-
Diabetes Insipidus (Dry - ↓ ADH effect): Hypernatremia & polyuria.
- Central: ↓ ADH production. Responds to desmopressin.
- Nephrogenic: Renal ADH resistance. No response.
⭐ Correcting hyponatremia from SIADH too rapidly (>8-12 mEq/L/24h) risks osmotic demyelination syndrome (central pontine myelinolysis).
Hypopituitarism - Powering Down
- Etiology: Pituitary adenomas (most common), Sheehan syndrome (postpartum necrosis), apoplexy, empty sella syndrome, craniopharyngioma.
- Clinical Presentation: Sequential loss of hormones.
- ↓GH → Dwarfism (children)
- ↓FSH/LH → Amenorrhea, ↓libido
- ↓TSH → Secondary hypothyroidism
- ↓ACTH → ↓cortisol, no hyperpigmentation
- 📌 Sequence of Loss: Go Look For The Adenoma (GH, LH, FSH, TSH, ACTH)
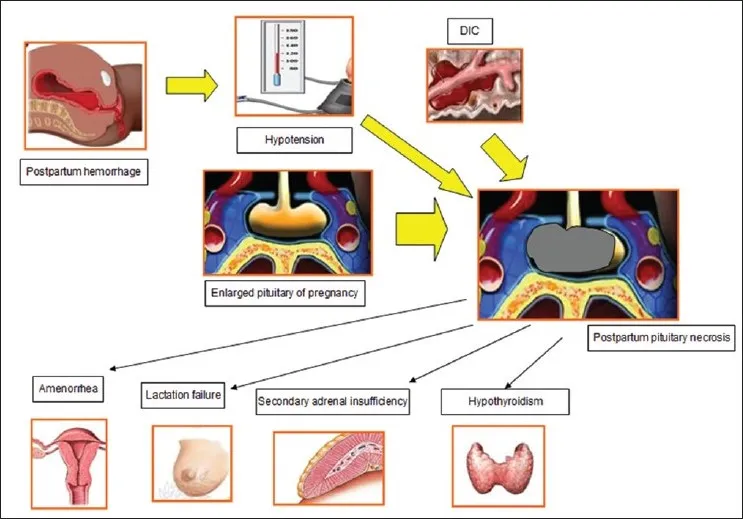
⭐ In pituitary-dependent adrenal insufficiency (↓ACTH), aldosterone levels are preserved by the renin-angiotensin system, but cortisol is low.
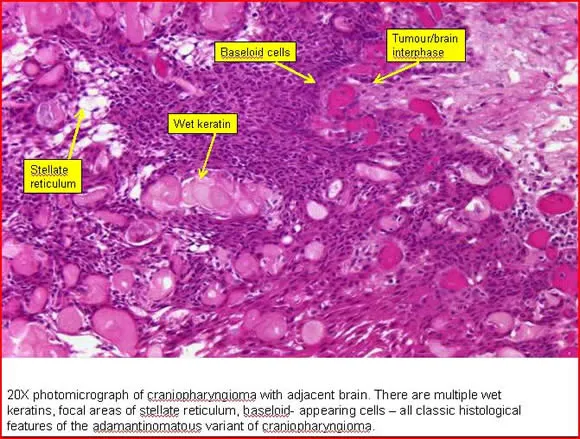
Craniopharyngioma - Rathke's Revenge
- Benign suprasellar tumor from Rathke's pouch remnants (ectoderm).
- Bimodal age distribution: common in children (5-15 yrs) & adults (>50 yrs).
- Presents with headaches, visual defects (bitemporal hemianopsia), and panhypopituitarism.
- Histology: "Wet" keratin, dystrophic calcification, and cysts with "machine oil" fluid (cholesterol crystals).
⭐ Most common childhood supratentorial tumor.
High‑Yield Points - ⚡ Biggest Takeaways
- Pituitary adenomas are the most common cause of hyperpituitarism; prolactinomas are the most frequent type.
- Mass effect from adenomas classically causes bitemporal hemianopsia by compressing the optic chiasm.
- Sheehan syndrome is postpartum pituitary necrosis, leading to hypopituitarism and failure to lactate.
- Central Diabetes Insipidus (↓ ADH) causes polyuria and hypernatremia; it responds to desmopressin.
- SIADH (↑ ADH) results in euvolemic hyponatremia and inappropriately concentrated urine.
- Pituitary apoplexy, an acute hemorrhage into an adenoma, is a neurosurgical emergency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

