Pheochromocytoma 101 - The Rule of 10s
📌 A classic mnemonic for pheochromocytoma characteristics, though some figures are now considered higher with modern testing.
- 10% Extra-adrenal (paraganglioma)
- 10% Bilateral (consider genetic syndromes)
- 10% Malignant
- 10% Occur in children
- 10% Are not associated with hypertension (can be normotensive or have episodic HTN)
⭐ Modern studies, especially with increased genetic screening, suggest that the rates of malignancy (
15-20%) and heritability (30-40%) are significantly higher than the classic 10% rule suggests.
Clinical Picture - The Catecholamine Cascade
- Classic Triad: Episodic Headache, Sweating, Tachycardia.
- Mnemonic (📌 The 5 P's):
- Pressure (paroxysmal hypertension)
- Pain (headache)
- Perspiration (diaphoresis)
- Palpitations (tachycardia)
- Pallor (vasoconstriction)
- Episodes are paroxysmal, lasting minutes to hours. Can be triggered by surgery, trauma, or medications (e.g., TCAs, MAOIs).
⭐ While the classic presentation is episodic, the most common sign is sustained hypertension.
Lab & Imaging Dx - Finding the Pheo
-
Biochemical Confirmation First:
- Initial test: Plasma free metanephrines (high sensitivity) or 24-hr urinary fractionated metanephrines.
- Positive if levels are >3-4x the upper limit of normal.
- Equivocal results? Consider clonidine suppression test (pheo won't suppress).
-
Tumor Localization (Post-Biochemical Dx):
- 1st line: Abdominal/pelvic CT with contrast or MRI (T2-bright).
- Functional Imaging: For extra-adrenal, metastatic, or multifocal disease.
- ¹²³I-MIBG Scintigraphy
- ⁶⁸Ga-DOTATATE PET/CT (higher sensitivity)
⭐ Warning: Percutaneous biopsy is contraindicated! It can provoke a hypertensive crisis from massive catecholamine release.
Pathology & Genetics - Code Blue Genes
- Germline mutations are present in ~30-40% of cases. Key syndromes dictate genetic testing.
- 📌 MEN have Very Nice Pheos: MEN2A/2B, Von Hippel-Lindau, Neurofibromatosis 1, Paraganglioma Syndromes (SDHx).
- Syndromic Associations:
- MEN 2A & 2B: RET proto-oncogene.
- Von Hippel-Lindau: VHL gene; often bilateral pheochromocytomas.
- Neurofibromatosis Type 1: NF1 gene.
- Familial Paraganglioma: Succinate dehydrogenase (SDHx) genes (SDHB, SDHD).
⭐ SDHB mutations carry the highest risk for malignant transformation and extra-adrenal tumors (paragangliomas).

Treatment - Alpha Before Beta
Pre-operative medical management is crucial to prevent intraoperative hypertensive crisis. The sequence is key.
📌 Mnemonic: Give Alpha-blockers Before Beta-blockers.
-
Alpha-Blockade (10-14 days pre-op):
- Irreversible: Phenoxybenzamine (preferred)
- Reversible: Phentolamine, Doxazosin
- Goal: Control blood pressure and vasoconstriction.
-
Beta-Blockade (2-3 days pre-op):
- Initiate only after adequate alpha-blockade.
- Goal: Control reflex tachycardia.
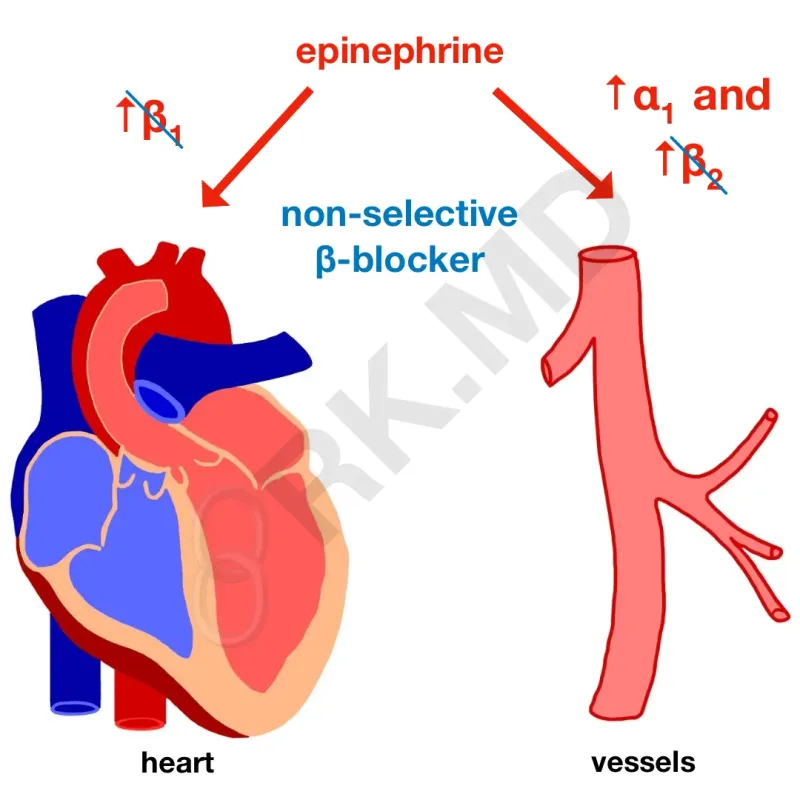
⭐ Warning: Giving β-blockers first causes unopposed α₁-receptor stimulation, leading to severe, refractory hypertension and potential pulmonary edema. This is a classic exam trap!
- Pheochromocytomas are catecholamine-secreting tumors from adrenal chromaffin cells; extra-adrenal tumors are paragangliomas.
- Presents with the classic triad: episodic headaches, sweating, and tachycardia (palpitations).
- Diagnose with ↑ 24-hour urinary metanephrines and catecholamines.
- Associated with MEN 2A/2B, VHL, and NF1 syndromes.
- Crucial management step: preoperative α-blockade (e.g., phenoxybenzamine) before β-blockade and surgery.
- Histology shows characteristic "Zellballen" nests of cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

