MI Pathogenesis - The Clot Thickens
- Initiating Event: Rupture or erosion of an unstable atherosclerotic plaque exposes its thrombogenic lipid core.
- Thrombosis: Platelet adhesion, activation, and the coagulation cascade rapidly form a thrombus, leading to coronary artery occlusion.
- Infarct Progression:
- Subendocardial Infarct: Involves the inner third of the myocardium, the region most vulnerable to ischemia. Often due to incomplete or transient occlusion.
- Transmural Infarct: Infarction spans the entire myocardial wall thickness, resulting from complete and prolonged occlusion (typically >6 hours).

⭐ The Left Anterior Descending (LAD) artery is the most commonly occluded coronary artery, typically leading to an anteroseptal MI.
Infarct Evolution - A Scar is Born
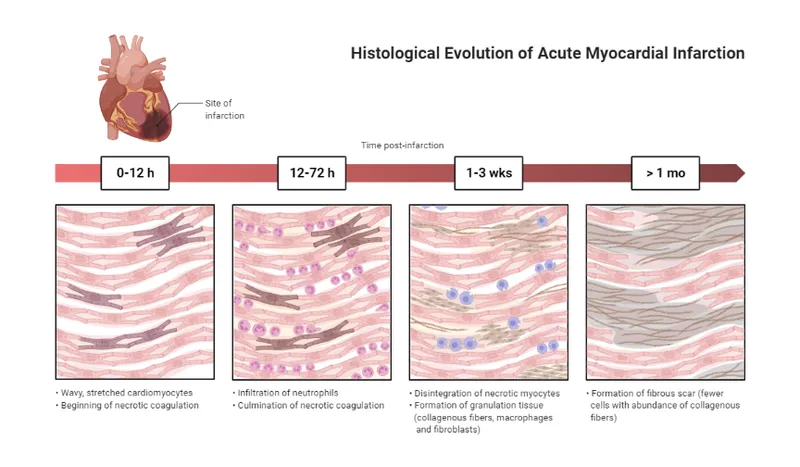
| Time Post-MI | Gross Changes | Microscopic Findings | Key Complications |
|---|---|---|---|
| 0-24h | Dark mottling | Early coagulative necrosis; edema, hemorrhage. Contraction bands with reperfusion. | Arrhythmia, cardiogenic shock, sudden death |
| 1-3d | Hyperemia, yellow-tan center | Coagulative necrosis, acute inflammation (neutrophils). | Fibrinous pericarditis |
| 3-14d | Yellow-tan, soft, with hyperemic border | Macrophages, granulation tissue formation. | Ventricular free wall rupture, papillary muscle rupture, interventricular septum rupture |
| >2w | Gray-white scar | Dense collagenous scar (fibrosis). | True aneurysm, Dressler syndrome, heart failure |
MI Complications - When the Heart Breaks
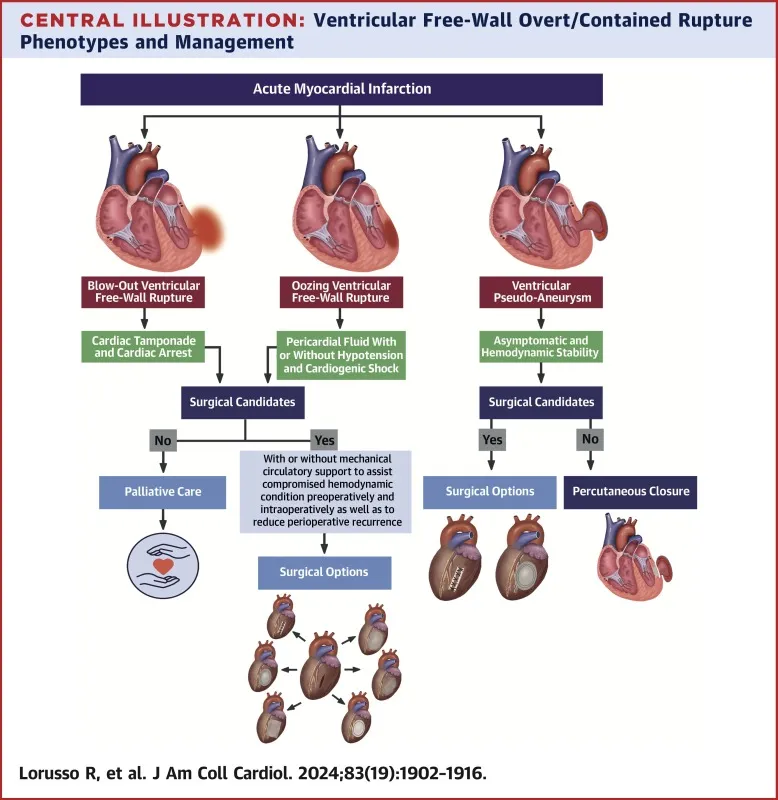
⭐ Papillary muscle rupture (posteromedial papillary muscle is most susceptible) leads to acute, severe mitral regurgitation.
- Free wall rupture: Leads to cardiac tamponade.
- Interventricular septum rupture: Creates a VSD (shunt).
- Mural thrombus: Risk of systemic embolization.
- Dressler syndrome: Autoimmune fibrinous pericarditis, weeks to months post-MI.
📌 Mnemonic (DARTH VADER): Death, Arrhythmia, Rupture, Tamponade, Heart failure, Valve disease, Aneurysm, Dressler's syndrome, Embolism, Recurrence.
High‑Yield Points - ⚡ Biggest Takeaways
- Coagulative necrosis and wavy fibers are the earliest changes (4-24 hours), followed by neutrophilic infiltrate.
- Macrophages dominate at 3-7 days, creating the highest risk period for myocardial rupture.
- Granulation tissue (type III collagen) appears at 1-2 weeks, maturing into a dense type I collagen scar.
- Reperfusion injury is characterized by contraction band necrosis due to massive calcium influx.
- The LAD artery is the most commonly occluded vessel, typically causing an anteroseptal MI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

