Risk Factors - Recipe for Disaster
-
Non-Modifiable:
- Age (risk increases with age)
- Sex (Male > Premenopausal Female)
- Genetics (Family history)
-
Modifiable (Major):
- Hyperlipidemia (↑ LDL, ↓ HDL)
- Hypertension (BP > 130/80 mmHg)
- Cigarette Smoking
- Diabetes Mellitus
-
Other Factors:
- Inflammation (e.g., ↑ hs-CRP)
- Obesity & Physical Inactivity
⭐ Hypertension is the single most important modifiable risk factor for atherosclerosis.
📌 Mnemonic: "SAD CHF" → Smoking, Age, Diabetes, Cholesterol (Hyperlipidemia), Hypertension, Family History.
Pathogenesis - Plaque Build-Up Blueprint
- Initiated by endothelial dysfunction; a "response-to-injury" process.
- Key steps in plaque formation:
- Cellular & Mediator Soup:
- Platelets: Adhere to injured endothelium.
- Growth Factors: PDGF (from platelets, macrophages) & FGF stimulate SMC proliferation.
- Cytokines: IFN-γ from T-cells activates macrophages, inhibiting SMC proliferation and collagen synthesis, thus weakening the cap.
⭐ Plaque stability, not size, is the primary determinant of clinical events. Stable plaques have thick fibrous caps, minimal inflammation, and small lipid cores. Unstable plaques are the opposite and prone to rupture.
Plaque Morphology - Anatomy of an Enemy
- Fibrous Cap: Superficial layer of smooth muscle cells (SMCs) & dense collagen.
- Separates lumen from the thrombogenic core.
- Stability depends on its thickness and collagen content.
- Necrotic Core: Central lipid-rich core.
- Contains cholesterol crystals, cellular debris, foam cells (lipid-laden macrophages), and calcium.
- Shoulder: Junction of cap and vessel wall.
- Weakest point, rich in inflammatory cells.
- Common site of plaque rupture.
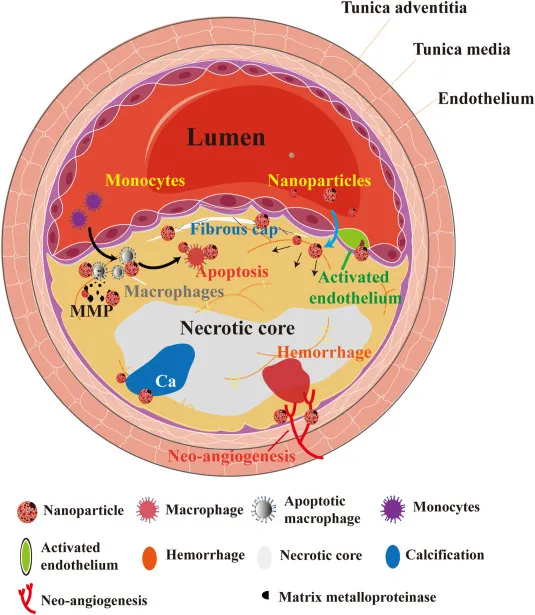
⭐ Plaque stability depends more on cap thickness and inflammation than on plaque size. Thin-capped fibroatheromas (TCFAs) are the most vulnerable plaques, prone to rupture and thrombosis.
Clinical Consequences - When Arteries Clog
- Chronic Stenosis: Leads to tissue ischemia when demand exceeds supply.
- Critical Stenosis: Typically >70% occlusion; causes symptoms with exertion (e.g., stable angina, intermittent claudication).
- Acute Plaque Change: Rupture, erosion, or hemorrhage of the plaque cap.
- Triggers thrombosis, causing acute occlusion → Myocardial Infarction (MI), stroke.
- Aneurysm Formation: Atherosclerosis weakens the vessel media, predisposing to dilation and rupture (e.g., Abdominal Aortic Aneurysm).
Vessel-Specific Syndromes:
- Coronary: Angina, MI
- Cerebral: TIA, Stroke
- Peripheral: PAD (claudication)
- Mesenteric: Ischemic bowel
- Renal: Secondary hypertension
⭐ The most common sites for severe atherosclerosis are, in order: abdominal aorta > coronary arteries > popliteal arteries > internal carotid arteries.
High‑Yield Points - ⚡ Biggest Takeaways
- Atherosclerosis is a chronic inflammatory and healing response of the arterial wall to endothelial injury.
- Major modifiable risk factors are dyslipidemia (especially ↑LDL), hypertension, cigarette smoking, and diabetes mellitus.
- The hallmark lesion is the atheroma, or fibrofatty plaque, which consists of a lipid core and a fibrous cap.
- Plaque rupture, ulceration, or erosion can induce thrombosis, leading to acute vascular occlusion.
- Clinical consequences include myocardial infarction, stroke, aortic aneurysms, and peripheral artery disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

