Fourth Stage of Labor - The Recovery Kickstart
- Timing: First 1-4 hours immediately following placental delivery.
- Physiology: Uterine involution begins; myometrial contractions compress vessels to achieve hemostasis.
- Maternal Monitoring (q15min for 1st hr):
- Uterus: Palpate fundus for tone (firm, midline) & location (at/below umbilicus).
- Lochia: Assess flow (rubra); saturation of >1 pad/hour suggests PPH.
- Vitals: BP & pulse checks for signs of hypovolemia.
- Perineum: Inspect for hematoma formation or suture dehiscence.
⭐ Uterine atony is the leading cause of early postpartum hemorrhage (PPH). Prophylactic oxytocin and fundal massage are key preventive measures.
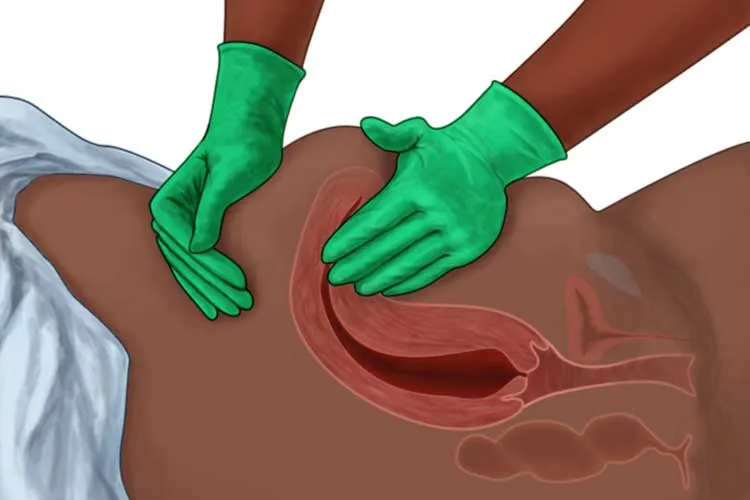
Maternal Assessment - The Postpartum Check-In
- Frequency: Vitals & fundal checks every 15 min for the first hour, then every 30 min for the second hour.
- Uterine Assessment:
- Palpate fundus for tone and location (should be firm, midline, at/below umbilicus).
- A boggy (soft) uterus signifies atony. First action: Fundal massage.
- Lochia Assessment:
- Check color (rubra), amount, and clots.
- Saturation of a perineal pad in <1 hour suggests excessive bleeding.
- Perineal Assessment:
- Inspect for hematomas, swelling, or signs of infection at laceration/episiotomy sites.
- Bladder: Encourage voiding; a full bladder can displace the uterus and cause atony.
⭐ High-Yield: Uterine atony is the #1 cause of early postpartum hemorrhage. Always perform fundal massage as the initial management step for a boggy uterus.
Postpartum Hemorrhage - The Red Alert
- Definition: Estimated Blood Loss (EBL) >1000 mL or blood loss with signs/symptoms of hypovolemia within 24 hours of birth.
- Etiology (The 4 T's) 📌
- Tone: Uterine atony (>70% of cases). Boggy, enlarged uterus.
- Trauma: Lacerations, uterine rupture.
- Tissue: Retained placenta or clots.
- Thrombin: Coagulopathy (pre-existing or acquired).
- Management
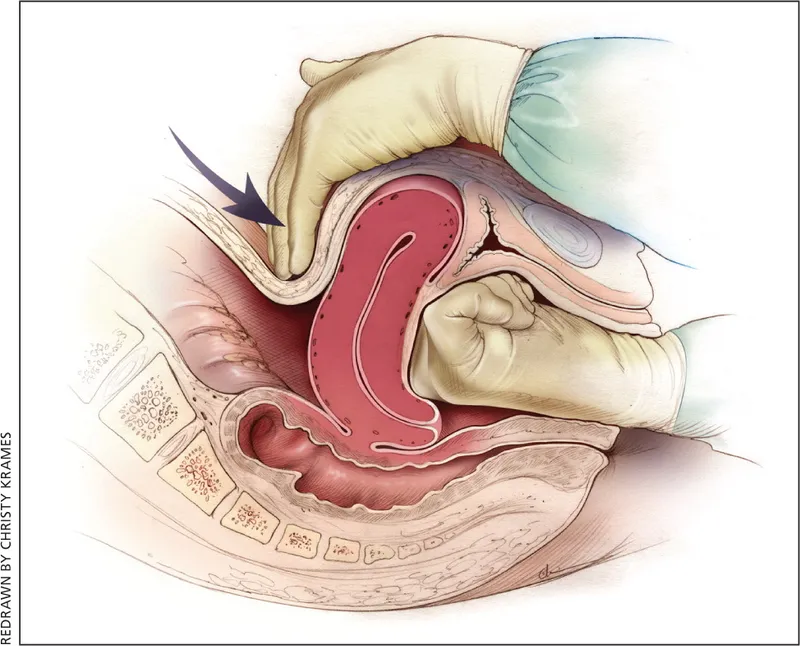
- First-line: Bimanual uterine massage & IV oxytocin.
- Second-line Uterotonics: Methylergonovine, Carboprost, Misoprostol.
⭐ Exam Favorite: Avoid Methylergonovine (Methergine) in patients with hypertension or preeclampsia due to its vasoconstrictive effects.
Postpartum Interventions - The Action Plan
- Uterine Assessment & Massage: Immediately palpate fundus; perform firm massage to maintain tone and express clots.
- Uterotonics: Administer Oxytocin (IV/IM) prophylactically to prevent postpartum hemorrhage (PPH).
- Perineal Care & Repair: Inspect for and repair any lacerations or episiotomies.
- Hemodynamic Monitoring: Closely monitor vital signs, uterine tone, and lochia amount for at least 1-2 hours. Check every 15 minutes.
⭐ Uterine atony is the most common cause of early postpartum hemorrhage, responsible for over 70% of cases.
High‑Yield Points - ⚡ Biggest Takeaways
- The fourth stage spans the first 1-4 hours postpartum, a critical period for physiologic stabilization.
- The most significant risk is postpartum hemorrhage (PPH), most commonly from uterine atony.
- Management involves frequent assessment of uterine tone (fundal massage), vital signs, and lochia.
- Oxytocin is continued to maintain firm uterine contraction and ensure hemostasis.
- This period is crucial for initiating maternal-infant bonding (e.g., skin-to-skin contact).
- Persistent bleeding with a firm uterus suggests genital tract lacerations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

