Fetal Growth Assessment - Sizing Up The Bump
- Fundal Height (FH):
- Measures symphysis pubis to uterine fundus.
- After 20 weeks, FH (cm) approximates gestational age (± 2 cm).
- Landmark: 20 weeks at umbilicus.
- Ultrasound Biometry:
- Confirms suspected abnormalities when FH is discordant.
- Parameters: Biparietal Diameter (BPD), Head Circumference (HC), Abdominal Circumference (AC), Femur Length (FL).
- Calculates Estimated Fetal Weight (EFW).
- Classification:
- Fetal Growth Restriction (FGR): EFW <10th percentile.
- Large for Gestational Age (LGA): EFW >90th percentile.
⭐ Abdominal Circumference (AC) is the single most sensitive parameter for detecting FGR, reflecting liver size and subcutaneous fat stores.
Ultrasound Biometry - Peeking with Sound
-
Core Parameters: Four key measurements assess fetal size and estimate gestational age (GA) and weight (EFW).
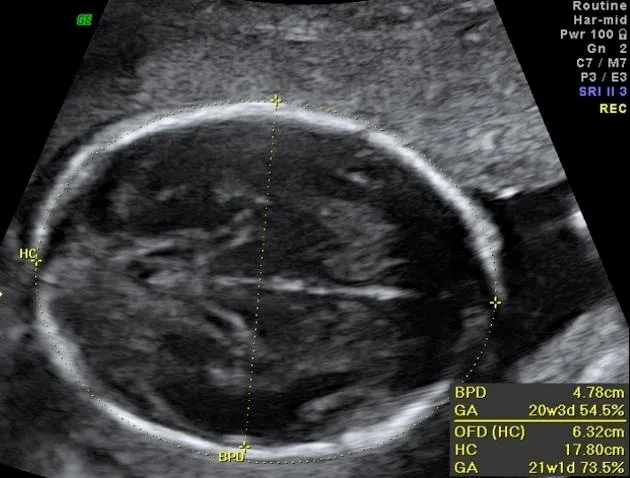
- Biparietal Diameter (BPD): Widest diameter of the fetal head.
- Head Circumference (HC): Measured at the same level as BPD.
- Abdominal Circumference (AC): Most critical for EFW. Reflects fetal nutrition and liver size.
- Femur Length (FL): Longest bone; reflects longitudinal growth.
-
Estimation Models:
- GA: Composite of BPD, HC, AC, and FL is used after the 1st trimester.
- EFW: Calculated using Hadlock's formula, which incorporates all four parameters.
⭐ High-Yield: Abdominal circumference (AC) is the single most sensitive indicator for detecting fetal growth restriction (FGR) as it's affected earliest by diminished glucose/glycogen stores in the liver.
Growth Abnormalities - Too Big, Too Small
-
Fetal Growth Restriction (FGR/IUGR): Estimated Fetal Weight (EFW) < 10th percentile.
- Symmetric: Early insult (1st trimester); chromosomal abnormalities, TORCH infections. Global, proportionate growth lag.
- Asymmetric: Late insult (2nd/3rd trimester); uteroplacental insufficiency (HTN, pre-eclampsia), maternal malnutrition. "Head-sparing" as brain growth is preserved over abdominal growth.
-
Large for Gestational Age (LGA): EFW > 90th percentile.
- Macrosomia: Birth weight > 4000 or 4500 g. Most common cause is maternal diabetes.
- Risks: Shoulder dystocia, birth trauma (clavicle fracture, brachial plexus injury), neonatal hypoglycemia.
- Management: Consider C-section if EFW > 5000 g (non-diabetic) or > 4500 g (diabetic).
⭐ In FGR, umbilical artery (UA) Doppler is critical. Absent or reversed end-diastolic flow indicates severe placental dysfunction and is a key factor in deciding the timing of delivery.
Management & Surveillance - The Growth Watch
- Serial Growth Ultrasounds: Every 3-4 weeks to monitor fetal growth velocity.
- Antenatal Surveillance: Initiated upon diagnosis. Frequency depends on severity.
- Nonstress Test (NST)
- Biophysical Profile (BPP)
- Modified BPP (NST + Amniotic Fluid Index)
- Umbilical Artery (UA) Doppler: Key for risk stratification and delivery timing.
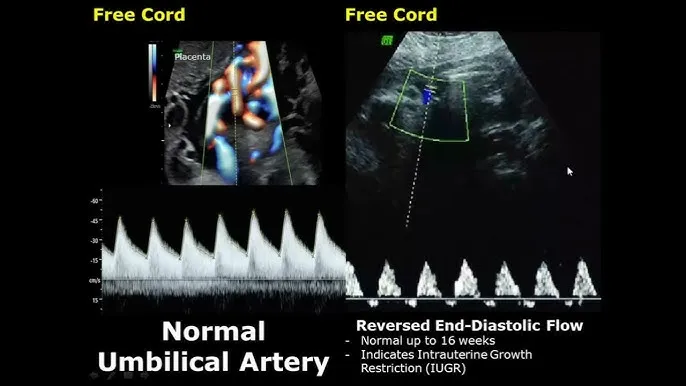
⭐ Reversed end-diastolic flow (REDF) in the umbilical artery is an ominous finding associated with a high risk of perinatal mortality, prompting delivery as early as 32 weeks.
High‑Yield Points - ⚡ Biggest Takeaways
- Fundal height is the initial screen; a >2-3 cm discrepancy from gestational age prompts ultrasound.
- Ultrasound biometry (BPD, HC, AC, FL) is the gold standard to estimate fetal weight (EFW).
- IUGR/SGA is an EFW <10th percentile; LGA is an EFW >90th percentile.
- Asymmetric IUGR (head-sparing) implies late-onset uteroplacental insufficiency (e.g., preeclampsia).
- Symmetric IUGR suggests an early insult like aneuploidy or congenital infection.
- Umbilical artery Doppler is crucial for IUGR management; absent or reversed end-diastolic flow is a critical finding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

