Etiology & Risks - The Tear Factors

- Maternal Factors:
- Primiparity (first delivery)
- Precipitous labor (< 3 hours)
- Previous perineal scarring (e.g., FGM, prior tear)
- Fetal Factors:
- Macrosomia (birth weight > 4 kg)
- Abnormal presentation (e.g., occiput posterior)
- Intrapartum Events:
- Operative vaginal delivery (forceps > vacuum)
- Episiotomy (especially midline)
- Prolonged second stage of labor
⭐ Midline episiotomy, while easier to repair and less painful, carries a higher risk of extension into the anal sphincter (3rd/4th-degree tears) than mediolateral episiotomy.
Classification - Degrees of Damage
Describes perineal tears sustained during vaginal delivery. Accurate classification is critical for appropriate management and prognosis.

- 1st Degree: Injury to perineal skin and/or vaginal mucosa only.
- 2nd Degree: Injury extends to the muscles of the perineal body, but the anal sphincter remains intact.
- 3rd Degree: Injury involves the anal sphincter complex.
- 3a: Less than 50% of the external anal sphincter (EAS) thickness is torn.
- 3b: More than 50% of the EAS thickness is torn.
- 3c: Both EAS and internal anal sphincter (IAS) are torn.
- 4th Degree: Injury extends through the entire anal sphincter complex (EAS and IAS) and into the rectal mucosa.
⭐ Proper identification and repair of third and fourth-degree tears are crucial to minimize the risk of future anal incontinence.
Repair Techniques - Stitching Strategy
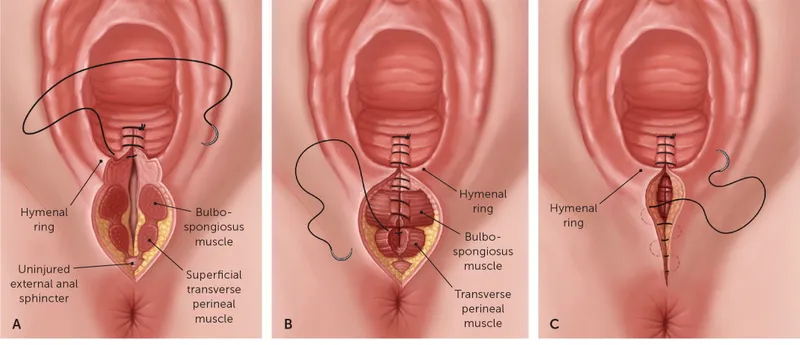
- Primary Goal: Achieve hemostasis and reapproximate tissue layers anatomically without tension.
- Suture Material: Use absorbable sutures.
- 2-0 or 3-0 polyglactin 910 (Vicryl) or similar synthetic suture is standard.
- Chromic gut is an alternative but may cause more tissue reaction.
- Core Technique:
- Anchor Above the Apex: The initial stitch must be placed ~1 cm proximal to the apex of the laceration to ligate the retracting artery, preventing hematoma formation.
- Continuous Suture: Generally preferred for vaginal mucosa and muscle layers. It's faster and uses less suture material.
- Non-locking: Standard for most of the repair to maintain tissue perfusion.
- Locking: Use selectively for improved hemostasis, especially at the apex or for brisk bleeding.
⭐ Failure to identify and secure the apex of a vaginal tear is a primary cause of postpartum hematoma formation and continued bleeding. Always ensure adequate visualization.
Post-Op & Complications - Healing Hurdles
- Infection:
- Signs: ↑pain, fever, purulent discharge, erythema.
- Prophylactic antibiotics for 3rd/4th degree tears.
- Wound Dehiscence:
- Breakdown of repair.
- Risks: infection, hematoma, poor surgical technique.
- Hematoma Formation:
- Severe pain, swelling, palpable mass.
- Small: conservative (ice, analgesia).
- Large (>5 cm) or expanding: surgical evacuation.
- Pain Control: NSAIDs, sitz baths.
⭐ Infected Dehiscence: Do not re-suture immediately. Allow drainage & granulation (secondary intention), then consider delayed repair.

High‑Yield Points - ⚡ Biggest Takeaways
- Suspect genital tract trauma when there is persistent bleeding despite a firm, contracted uterus.
- A systematic examination of the perineum, vagina, and cervix is crucial for diagnosis.
- Cervical lacerations most commonly occur at the 3 and 9 o'clock positions.
- Fourth-degree tears involve the rectal mucosa and require meticulous, layered repair to prevent fistulas.
- Expanding hematomas can present as severe pain and pressure with minimal visible bleeding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

