Definition & Quantification - More Than a Feeling
- Primary Definition (ACOG 2017): Cumulative blood loss (CBL) of ≥1,000 mL OR blood loss accompanied by signs/symptoms of hypovolemia within 24 hours of birth.
- Traditional Definitions:
- Vaginal Delivery: >500 mL
- Cesarean Delivery: >1,000 mL
- Quantification:
- QBL (Quantitative Blood Loss): Formal measurement (weighing drapes/sponges). More accurate.
- EBL (Estimated Blood Loss): Visual inspection. Notoriously inaccurate.
- Classification by Onset:
- Primary (Early): Within the first 24 hours postpartum. (Most common)
- Secondary (Late): Between 24 hours and 12 weeks postpartum.
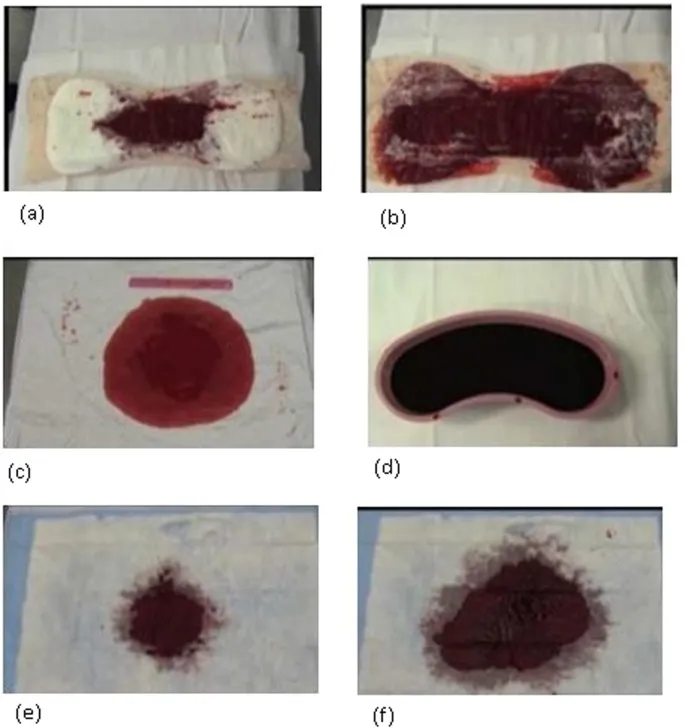
⭐ Visual estimation of blood loss (EBL) is highly unreliable, often underestimating actual loss by up to 50%. This is why a shift to QBL is emphasized in modern protocols.
Classification & Etiology - The Usual Suspects (4 T's)
- Primary (Early) PPH: Blood loss within the first 24 hours postpartum.
- Secondary (Late) PPH: Occurs between 24 hours and 12 weeks postpartum.
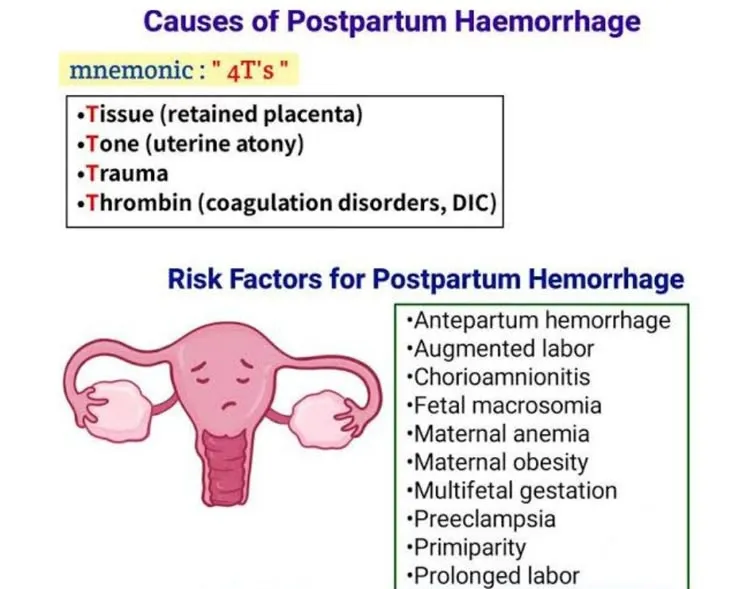
📌 Mnemonic: The "4 T's" outline the primary etiologies, ordered by frequency.
-
Tone (Uterine Atony) (~70-80%)
- Most common cause. The uterus fails to contract adequately ("boggy" uterus).
- Risk Factors: Uterine overdistension (macrosomia, multiples), prolonged labor, high parity, chorioamnionitis, tocolytic use.
-
Trauma (~20%)
- Lacerations of the genital tract (cervix, vagina, perineum), often after operative delivery.
- Uterine rupture or inversion.
- Hematoma formation (perineal, vaginal).
-
Tissue (~5-10%)
- Retained placental fragments (e.g., succenturiate lobe) or membranes.
- Abnormal placentation (placenta accreta spectrum).
- Retained blood clots.
-
Thrombin (~1%)
- Pre-existing or acquired coagulopathies that impair clot formation.
- Examples: von Willebrand disease, ITP, HELLP syndrome, DIC (e.g., from placental abruption or amniotic fluid embolism).
⭐ Uterine atony is the single most common cause of PPH. In a patient with a soft, boggy uterus and continued bleeding after delivery, atony should be the primary diagnosis to address.
High‑Yield Points - ⚡ Biggest Takeaways
- Postpartum hemorrhage (PPH) is blood loss >500 mL (vaginal) or >1000 mL (cesarean).
- Clinically, it's any blood loss causing signs of hypovolemia.
- Primary PPH is within 24 hours postpartum; secondary PPH is from 24 hours to 12 weeks.
- Uterine atony is the leading cause of primary PPH (~80% of cases).
- Diagnosis relies on Quantitative Blood Loss (QBL), not visual estimation.
- Tachycardia is often the earliest sign of significant hemorrhage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

