Indications & Mechanism - The Pressure Play
-
Primary Indication: Atonic postpartum hemorrhage (PPH) refractory to uterotonic medications.
- Used when bleeding persists despite oxytocin, methylergonovine, and carboprost.
-
Mechanism of Action: Direct physical tamponade.
- An inflated balloon applies pressure to the uterine wall, exceeding arterial pressure.
- This collapses the open spiral arterioles at the placental site, achieving hemostasis.
⭐ Balloon tamponade is a temporizing "bridge" therapy, not definitive. It buys time for patient stabilization and transfer for higher-level care (e.g., uterine artery embolization) if needed.
Device Types - The Balloon Brigade
-
Purpose-Built (FDA-Approved):
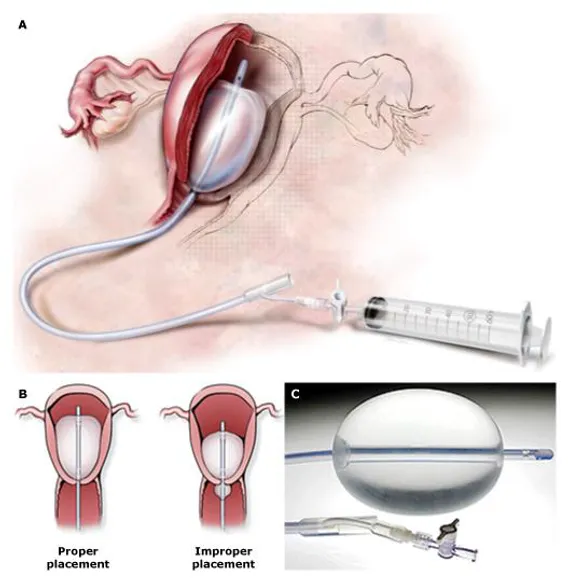
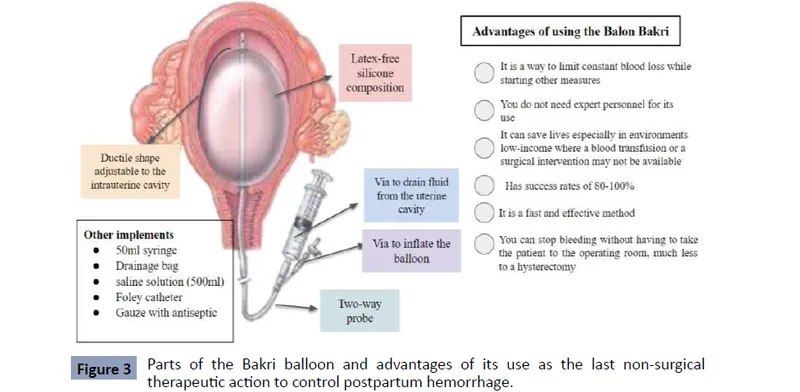
- Bakri Balloon: Pear-shaped silicone balloon conforming to the uterine cavity. Inflate with 300-500 mL of sterile saline.
- BT-Cath: A balloon catheter system designed for ease of use in PPH.
-
Off-Label Options:
- Foley Catheter: Widely available; inflate with 60-80 mL.
- Sengstaken-Blakemore Tube: Borrowed from GI hemorrhage management.
- Rusch Catheter: A straight, firm urologic catheter.
⭐ Key Feature: The Bakri balloon has a central drainage lumen to monitor ongoing blood loss from above the balloon, allowing for real-time assessment of tamponade effectiveness.
Procedure & Placement - The Inflation Drill
- Preparation: Position patient (dorsal lithotomy), ensure adequate anesthesia.
- Placement: Manually or with forceps, guide the balloon into the uterine cavity, ensuring it's above the internal os. Confirm placement with transvaginal ultrasound.
- Inflation: Instill sterile saline until the balloon is full (300-500 mL for Bakri) or bleeding stops. The uterus should feel firm abdominally.
- Traction: Apply gentle downward traction and secure the catheter to the patient's thigh, creating a tamponade effect against the lower uterine segment.
⭐ The "tamponade test": After inflation, observe for 15-20 minutes. If bleeding is not significantly reduced, the balloon is likely ineffective or misplaced, and you must escalate care.
Management & Complications - The Aftermath
- Post-Placement Care:
- Monitor vitals and bleeding closely; ensure continued uterotonic therapy.
- The balloon acts as a tamponade, not a definitive cure.
- Removal Protocol:
- Maintain inflation for 12-24 hours.
- Deflate balloon gradually, observing for renewed bleeding for ~30 min before removal.
- Potential Complications:
- Uterine rupture or perforation.
- Endometritis or chorioamnionitis.
- Device migration or spontaneous expulsion.
- Pain, cramping, or bladder tenesmus.
⭐ Prophylactic broad-spectrum antibiotics are crucial while the balloon is in situ to prevent endometritis.
High-Yield Points - ⚡ Biggest Takeaways
- Indicated for postpartum hemorrhage (PPH) refractory to uterotonic agents, most commonly due to uterine atony.
- Functions by exerting direct intracavitary pressure on the uterine wall to mechanically control bleeding.
- Common devices include the Bakri balloon, but a Foley catheter can be an alternative.
- Placement is confirmed with ultrasound to ensure it is within the uterus and not the lower uterine segment.
- Inflate with sterile saline until bleeding stops, typically 300-500 mL.
- Leave in place for 12-24 hours with concurrent antibiotic prophylaxis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

