Pathophysiology - The Great Separation
- Primary Event: Rupture of maternal spiral arteries in the decidua basalis.
- Hematoma Formation: Bleeding leads to a retroplacental hematoma.
- As the hematoma expands, it shears the placenta off the uterine wall.
- This separation severely compromises fetal oxygen and nutrient supply.
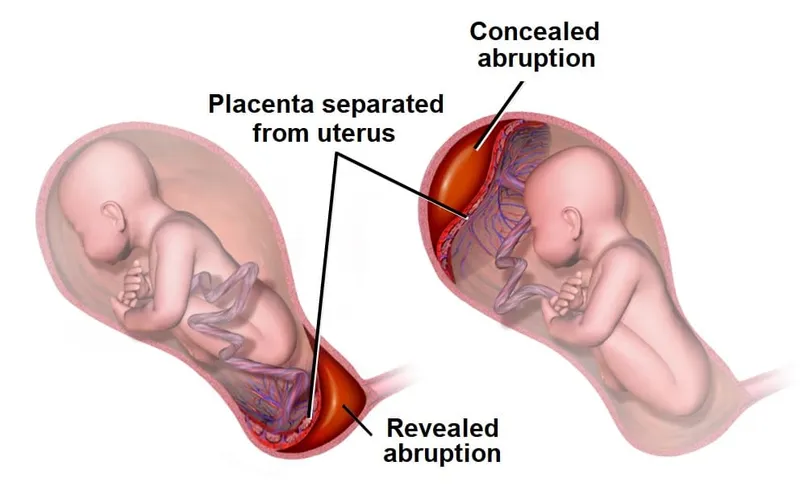
- Bleeding Types:
- Revealed: Blood tracks down and drains through the cervix (visible bleeding).
- Concealed: Blood is trapped behind the placenta, with no visible external bleeding.
⭐ Disseminated Intravascular Coagulation (DIC) is a major risk. Damaged decidual tissue releases large amounts of tissue factor (thromboplastin) into maternal circulation, triggering the coagulation cascade.
Risk Factors - Recipe for Disaster
- Prior placental abruption: Strongest predictor, with a 10-15% recurrence risk.
- Maternal hypertensive disorders:
- Chronic hypertension
- Preeclampsia / eclampsia
- Trauma:
- Blunt abdominal trauma (e.g., MVA, falls, domestic violence)
- Substance use:
- Cocaine (vasoconstriction)
- Tobacco smoking
- Sudden uterine decompression:
- Amniorrhexis with polyhydramnios
- Delivery of the first twin
- Other key factors:
- PPROM (Prelabor Rupture of Membranes)
- Advanced maternal age (AMA)
- Thrombophilias
⭐ A history of abruption in a previous pregnancy is the single most important risk factor.
Clinical Presentation - Code Red
- Sudden-onset, severe abdominal pain or backache.
- Painful, dark vaginal bleeding (⚠️ can be concealed in 20% of cases).
- Uterine findings:
- Tender, firm-to-rigid consistency.
- High-frequency, low-amplitude contractions (tetanic).
- Maternal instability:
- Tachycardia, hypotension (signs of shock).
- Risk of Disseminated Intravascular Coagulopathy (DIC).
- Fetal distress:
- Non-reassuring fetal heart rate patterns (bradycardia, late decelerations).
- Sinusoidal pattern is an ominous sign.
⭐ High-Yield: The amount of visible vaginal bleeding does not correlate with the degree of maternal hemorrhage, as a significant volume can be trapped behind the placenta (concealed abruption).
Diagnosis & Management - Damage Control
- Maternal Stabilization First: Priority is aggressive resuscitation.
- Secure airway; administer supplemental O₂.
- Place 2 large-bore IVs (≥16-gauge).
- Begin rapid infusion of crystalloids.
- Transfuse blood products (PRBCs, FFP, platelets) for hemorrhage & coagulopathy.

- Delivery Decision Algorithm:
⭐ Be prepared for Disseminated Intravascular Coagulation (DIC). The large retroplacental hematoma releases tissue factor (thromboplastin), triggering a massive consumptive coagulopathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Painful third-trimester vaginal bleeding is the hallmark sign, unlike the painless bleeding of placenta previa.
- Strongly associated with maternal hypertension, cocaine use, and abdominal trauma.
- Diagnosis is clinical; ultrasound may show a retroplacental hematoma but is not sensitive.
- Risk of Disseminated Intravascular Coagulation (DIC) from thromboplastin release.
- Can present with a tender, rigid (hypertonic) uterus.
- Management requires immediate C-section for fetal or maternal distress.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

