Thyroid Physiology in Pregnancy - Hormone High Jinks
- Estrogen: ↑ Estrogen → ↑ hepatic synthesis of Thyroxine-Binding Globulin (TBG).
- Binds more thyroid hormone, leading to ↑ Total T4 (TT4) and Total T3 (TT3).
- Free T4/T3 levels remain relatively stable.
- hCG: The α-subunit of hCG is similar to TSH, weakly stimulating the TSH receptor.
- Results in ↑ T4/T3 production.
- Causes a physiological ↓ in TSH, especially in the 1st trimester.
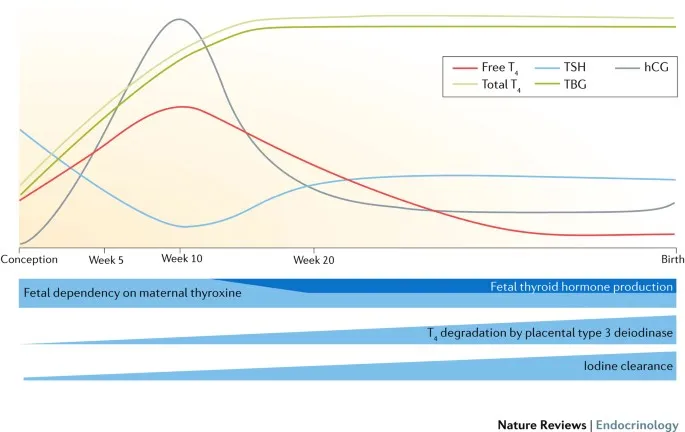
⭐ High first-trimester hCG levels can cause transient gestational thyrotoxicosis and are linked to hyperemesis gravidarum; TSH will be appropriately suppressed.
Hypothyroidism in Pregnancy - Low & Slow
- Etiology: Most common cause is Hashimoto's thyroiditis (anti-TPO antibodies).
- Maternal Risks: Preeclampsia, anemia, miscarriage, postpartum hemorrhage.
- Fetal/Neonatal Risks: Impaired neurodevelopment (cretinism), preterm birth, low birth weight.
- Management: Treat with levothyroxine to maintain TSH < 2.5 mU/L. Monitor TSH every 4-6 weeks during pregnancy and adjust dose as needed.
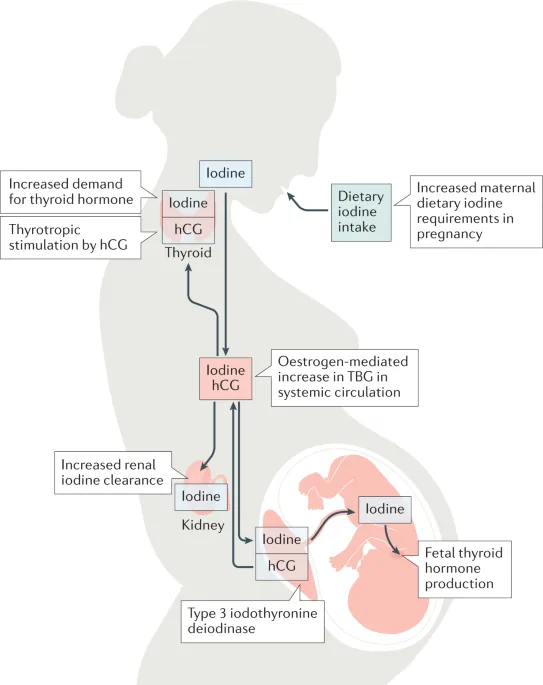
⭐ Maternal thyroxine (T4) is crucial for fetal brain development before the fetal thyroid becomes functional around 12 weeks gestation.
Hyperthyroidism in Pregnancy - High & Hasty
- Etiology: Most commonly Graves' disease (~95%). Can also be hCG-mediated (molar pregnancy, multiple gestations) as hCG α-subunit mimics TSH.
- Diagnosis: ↓TSH, ↑Free T4/T3. TSH-receptor antibodies (TRAb) confirm Graves'.
- Maternal Risks: Preeclampsia, heart failure, thyroid storm.
- Fetal Risks: Goiter, tachycardia, IUGR, hydrops fetalis, preterm birth.
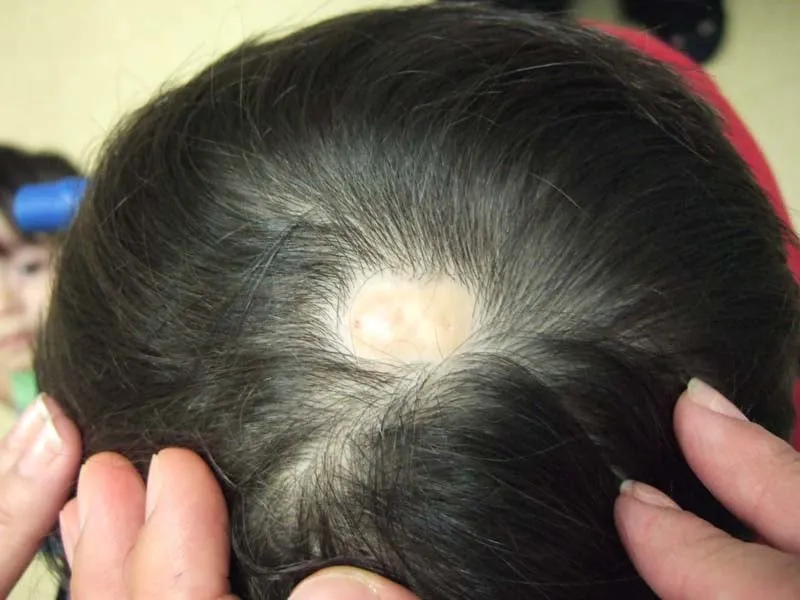
⭐ Methimazole (MMI) use in the first trimester is associated with a specific pattern of birth defects known as methimazole embryopathy, most notably aplasia cutis congenita.
- Management:
- 1st Trimester: Propylthiouracil (PTU). 📌 PTU for Primary trimester.
- 2nd/3rd Trimester: Switch to Methimazole (MMI) to avoid PTU's hepatotoxicity risk.
Postpartum Thyroiditis - The Aftermath
- Autoimmune thyroiditis occurring within 1 year postpartum, often revealing underlying Hashimoto's.
- Presents with a triphasic course: transient hyperthyroidism, then hypothyroidism, followed by recovery.
- Diagnosis: Based on clinical picture and positive anti-TPO antibodies. Radioiodine uptake is low.
⭐ There is a 20-40% risk of developing permanent hypothyroidism and a high risk of recurrence in future pregnancies.
- Management: Symptomatic. Use β-blockers for thyrotoxicosis and Levothyroxine for symptomatic hypothyroidism.
High-Yield Points - ⚡ Biggest Takeaways
- Maternal hypothyroidism is a major risk for impaired fetal neurodevelopment and cretinism.
- hCG can stimulate TSH receptors, leading to gestational transient thyrotoxicosis in the 1st trimester.
- Graves' disease is the most common cause of hyperthyroidism; TSH-receptor antibodies cross the placenta.
- Treat hyperthyroidism with propylthiouracil (PTU) in the 1st trimester, then switch to methimazole.
- PTU has a risk of maternal hepatotoxicity; methimazole is linked to aplasia cutis.
- Thyroid storm is an obstetric emergency requiring beta-blockers, PTU, and steroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

