Risks & Complications - The Heavy Burden
-
Maternal Risks:
- ↑ Gestational Diabetes (GDM) & insulin resistance.
- ↑ Hypertensive disorders (preeclampsia, chronic HTN).
- ↑ Venous thromboembolism (VTE).
- ↑ Cesarean delivery rates & associated morbidity (e.g., infection, blood loss).
- Failed induction, dysfunctional labor.
-
Fetal & Neonatal Risks:
- Macrosomia (birth weight > 4000-4500 g) → shoulder dystocia.
- ↑ Congenital anomalies (neural tube defects, cardiac).
- ↑ Stillbirth / Intrauterine Fetal Demise (IUFD).
- Neonatal hypoglycemia.
- Childhood obesity.
⭐ Maternal obesity is an independent risk factor for neural tube defects, warranting higher dose folic acid supplementation pre-conceptionally and in early pregnancy.
Antenatal Management - Proactive Pregnancy Patrol
-
Weight & Lifestyle Counseling:
- Establish strict weight gain goals based on IOM:
- Overweight (BMI 25-29.9): 15-25 lb
- Obese (BMI ≥30): 11-20 lb
- Refer for nutritional counseling.
- Advise moderate-intensity exercise, ~150 min/week.
- Establish strict weight gain goals based on IOM:
-
Screening & Prophylaxis:
- Early glucose challenge test or HbA1c for pre-existing diabetes.
- Low-dose aspirin (81 mg/day) initiated between 12-16 weeks for preeclampsia prophylaxis.
- Standard GDM screening with 1-hr GCT at 24-28 weeks.
-
Fetal Surveillance:
- Detailed anatomy scan (18-22 weeks); visualization may be limited.
- Consider serial growth scans in the 3rd trimester for macrosomia/FGR.
⭐ For patients with obesity (a significant risk factor for preeclampsia), initiating low-dose aspirin before 16 weeks is a key evidence-based intervention to mitigate risk.
Intrapartum & Postpartum - The Final Stretch
- Intrapartum Management:
- Labor: Higher risk of dystocia (prolonged labor) and failed induction.
- Delivery: Increased rates of operative vaginal delivery and cesarean section.
- Anesthesia: Anticipate difficult epidural/spinal placement. Higher failure rate of regional anesthesia, potentially requiring general anesthesia. Anesthesia consult is recommended.
- Postpartum Risks:
- Hemorrhage: ↑ risk of postpartum hemorrhage (PPH) from uterine atony.
- VTE: Significantly elevated risk for venous thromboembolism. Utilize mechanical and/or pharmacologic prophylaxis.
- Wound: ↑ risk of C-section wound infection, seroma, and dehiscence.
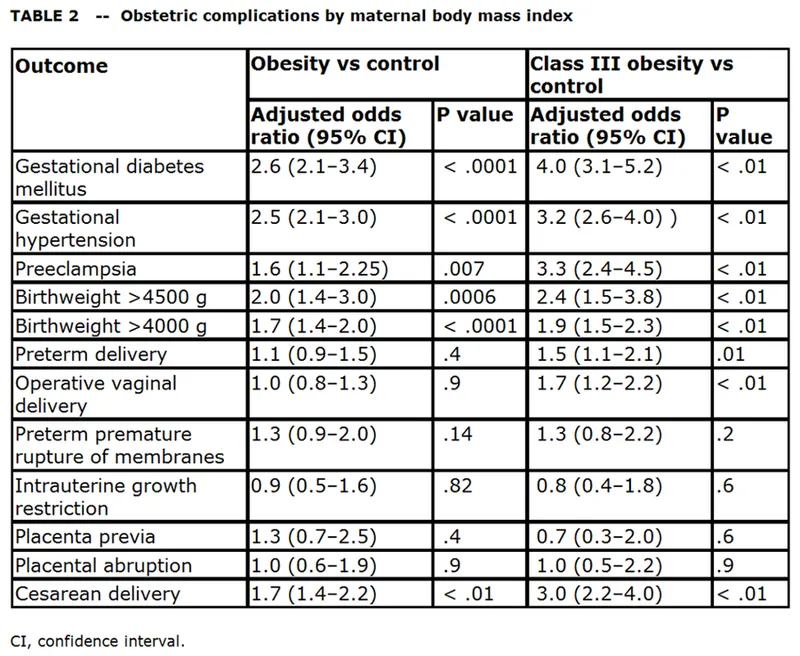
⭐ Women with a BMI >30 have a 2-3 fold increased risk of requiring a cesarean delivery and a significantly higher risk of postpartum venous thromboembolism.
Weight & Counseling - Pounds and Plans
-
IOM Gestational Weight Gain (GWG) Recommendations:
- Underweight (BMI < 18.5): Gain 28-40 lbs
- Normal weight (BMI 18.5-24.9): Gain 25-35 lbs
- Overweight (BMI 25.0-29.9): Gain 15-25 lbs
- Obese (BMI ≥ 30.0): Gain 11-20 lbs
-
Counseling Focus:
- Diet: Refer to a nutritionist. Emphasize balanced meals, avoiding empty calories. Caloric restriction for weight loss is contraindicated.
- Exercise: Advise 30+ minutes of moderate activity (e.g., walking, swimming) on most days of the week, if not contraindicated.
⭐ Exam Favorite: Excessive gestational weight gain, especially in obese women, significantly ↑ the risk of fetal macrosomia ($> 4000-4500$ g), cesarean delivery, and long-term maternal/child obesity.
- Pre-conception counseling on weight loss and nutritional optimization is the most critical intervention.
- Major maternal risks include gestational diabetes, preeclampsia, VTE, and higher C-section rates.
- Key fetal risks are macrosomia, neural tube defects (NTDs), stillbirth, and future childhood obesity.
- Mandates early glucose screening for GDM and a higher dose of folic acid to reduce NTD risk.
- Labor may be complicated by failed induction, prolonged stages, and anesthesia challenges.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

