Pneumocystis jirovecii - The Immunocompromised Foe
- Yeast-like fungus, primarily affects immunocompromised hosts, especially with CD4 count < 200 cells/mm³.
- Causes Pneumocystis Pneumonia (PCP), presenting with fever, dry cough, and dyspnea.
- Diagnosis: Bronchoalveolar lavage (BAL) fluid stained with methenamine silver or toluidine blue.
- Shows characteristic cysts (crushed ping-pong balls).
- Treatment & Prophylaxis: Trimethoprim-sulfamethoxazole (TMP-SMX).
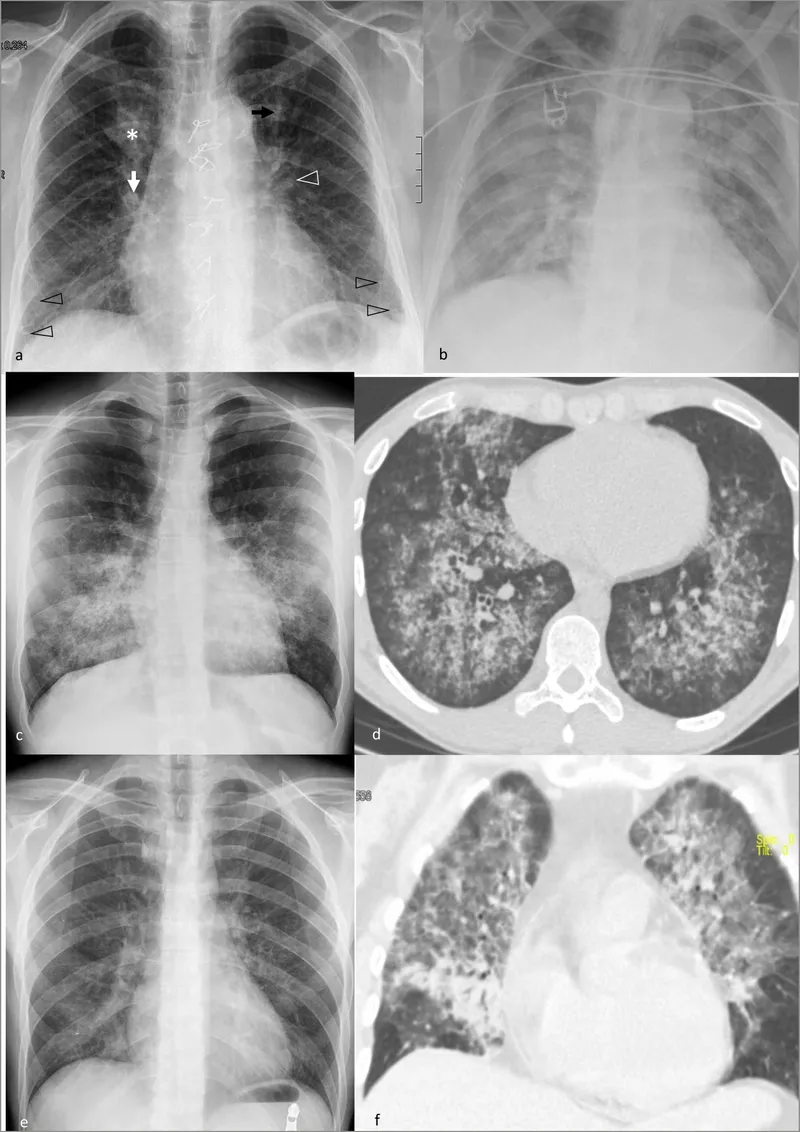
⭐ High-Yield: Chest X-ray classically shows diffuse, bilateral ground-glass opacities or "bat-wing" appearance.

Pathophysiology - Suffocating the Alveoli
- Inhalation & Attachment: Airborne cysts are inhaled, lodge in alveoli, and differentiate into trophic forms.
- Replication: Trophozoites attach to alveolar type I epithelial cells but do not invade. They replicate extracellularly within the alveolar space.
- Alveolar Filling: Proliferation leads to a characteristic foamy, eosinophilic, proteinaceous exudate-a mix of organisms, host proteins, and debris.
- Gas Exchange Block: This thick exudate fills alveoli, creating a significant diffusion barrier, causing progressive hypoxemia and respiratory failure.
⭐ The hallmark histological finding is a "honeycomb" or "cotton candy" appearance of pink, frothy exudate filling the alveolar spaces on H&E stain.

Clinical Presentation - The Classic Triad
- Classic Triad:
- Progressive dyspnea on exertion (DOE)
- Fever
- Non-productive cough
- Onset: Insidious, developing over days to weeks, unlike bacterial pneumonias.
- Patient Profile: Primarily in immunocompromised hosts (HIV with CD4 < 200 cells/mm³, transplant, malignancy).
- Exam: Often unremarkable; minimal auscultatory findings despite significant hypoxia.
⭐ A markedly elevated serum lactate dehydrogenase (LDH) > 220 U/L is a classic, albeit non-specific, finding.
Diagnosis - Unmasking the Fungus
- Specimen Collection:
- Bronchoalveolar lavage (BAL) is the gold standard.
- Induced sputum is less invasive but has lower sensitivity.
- Microscopy & Stains:
- Methenamine Silver (GMS): Stains cysts black, often appearing as classic “crushed ping-pong balls” or “dented helmets”.
- Giemsa or Wright-Giemsa: Stains trophozoites and intracystic sporozoites.
- Direct fluorescent antibody (DFA) staining is also highly sensitive and specific.
- Lab Markers:
- ↑ Lactate Dehydrogenase (LDH >200 U/L) is a non-specific but common finding.
- ↑ Serum (1,3)-β-D-glucan.
⭐ Exam Favorite: Pneumocystis jirovecii cannot be grown in routine fungal cultures.

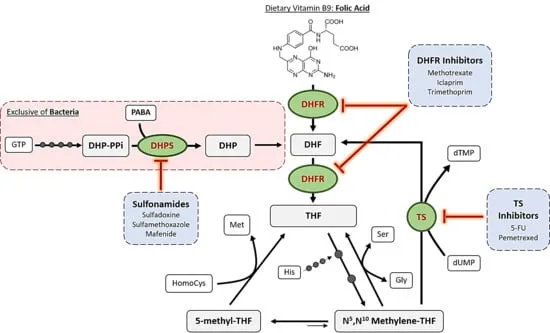
Treatment & Prophylaxis - The Sulfa Solution
- Primary Tx: Trimethoprim-sulfamethoxazole (TMP-SMX) is the drug of choice for treatment.
- Alternatives: For sulfa allergy or intolerance, use:
- Pentamidine (IV)
- Clindamycin + Primaquine
- Atovaquone
- Prophylaxis: Indicated for HIV patients with CD4+ count < 200 cells/μL.
- TMP-SMX is the preferred agent.
- Alternatives include Dapsone, Atovaquone, or aerosolized Pentamidine.
⭐ Adjunctive corticosteroids are given in moderate-to-severe disease (PaO₂ < 70 mmHg or A-a gradient > 35 mmHg) to reduce inflammation and improve survival.
High‑Yield Points - ⚡ Biggest Takeaways
- Opportunistic fungus that causes Pneumocystis Pneumonia (PCP), almost exclusively in the immunocompromised.
- Strongly associated with HIV/AIDS, particularly when the CD4 count drops < 200 cells/mm³.
- Chest X-ray classically shows diffuse, bilateral interstitial infiltrates or ground-glass opacities.
- Definitive diagnosis via bronchoalveolar lavage (BAL) with methenamine silver stain to visualize characteristic disc-shaped cysts.
- Trimethoprim-sulfamethoxazole (TMP-SMX) is the cornerstone for both prophylaxis and treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

