Microbiology & Risk Factors - The Moldy Menace
- Causative Agents: Mucor, Rhizopus, Lichtheimia (formerly Absidia) species.
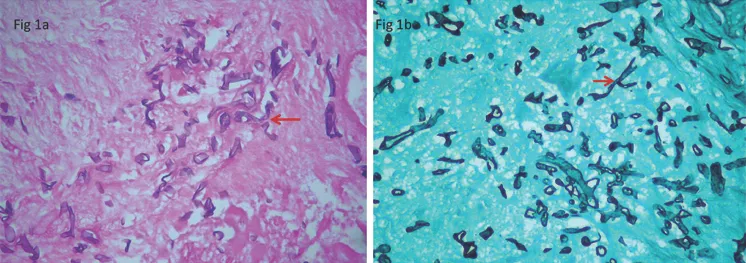
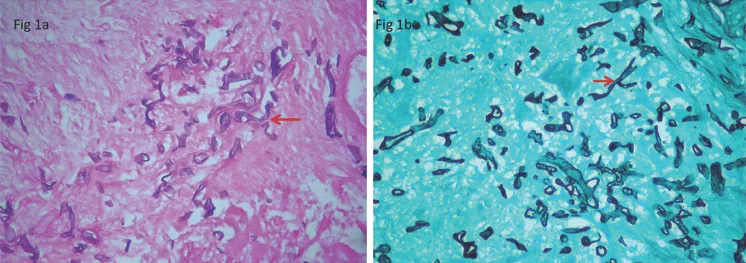
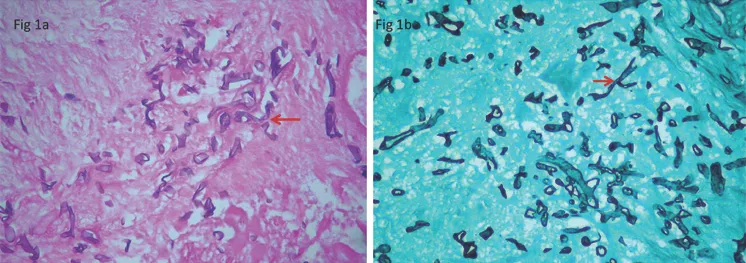
- Microscopic Morphology:
- Broad, ribbon-like, non-septate (pauciseptate) hyphae.
- Branching occurs at wide, often right angles (~90°).
- Major Risk Factors:
- Diabetic Ketoacidosis (DKA): Hyperglycemia & acidosis create a favorable environment.
- Immunosuppression: Especially neutropenia and high-dose corticosteroid therapy.
- Iron Overload: Deferoxamine use paradoxically ↑ risk by acting as a fungal siderophore.
⭐ In DKA, acidosis causes dissociation of iron from binding proteins, and hyperglycemia enhances fungal growth, creating a perfect storm for Mucor invasion.
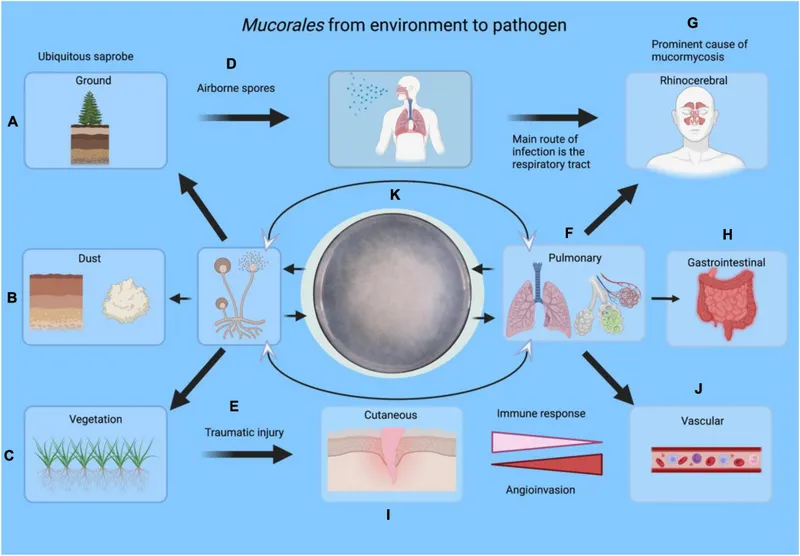
Pathophysiology - Angioinvasive Attack
- Host Factors: Thrives in high-glucose, acidic environments. Key risks: Diabetic Ketoacidosis (DKA), neutropenia, iron overload (deferoxamine use).
- Angioinvasion: Hyphae have a predilection for invading blood vessels, leading to thrombosis, infarction, and subsequent tissue necrosis.
⭐ The fungus possesses ketone reductase systems, allowing it to thrive in the high glucose, acidic conditions of DKA, a classic USMLE association.
Rhinocerebral Mucormycosis - A Sinister Spread
Primarily affects immunocompromised hosts, especially with Diabetic Ketoacidosis (DKA). Fungi (Rhizopus, Mucor) invade blood vessels, causing thrombosis and tissue necrosis.
- Presentation: Acute sinusitis with fever, facial pain, headache.
- Hallmark Sign: Black necrotic eschar on the nasal mucosa or hard palate.
- Progression: Rapidly spreads through the cribriform plate to the brain.
- Leads to cavernous sinus thrombosis, proptosis, and cranial nerve palsies.
⭐ In DKA, high glucose and acidic pH impair neutrophil function, while excess free iron (released from transferrin) acts as a critical growth factor for the fungi.
Diagnosis & Management - ID and Intervene
- Diagnosis:
- Histopathology: Key for rapid diagnosis. Biopsy shows broad, non-septate hyphae with wide-angle (90°) branching.
- Culture: Confirms organism, but slow and may be falsely negative.
- Imaging: CT/MRI to assess the extent of angioinvasion and tissue necrosis.
- Management:
- Emergent Surgical Debridement: Aggressive removal of all necrotic tissue is critical.
- Antifungal Therapy: High-dose IV Liposomal Amphotericin B is first-line. Step-down to oral posaconazole or isavuconazole.
- Control Risk Factors: Reverse DKA, manage neutropenia.
⭐ The presence of a black necrotic eschar in the nasal cavity or on the hard palate of a diabetic (especially DKA) or immunocompromised patient is highly suggestive of rhinocerebral mucormycosis.
- Primarily affects immunocompromised hosts, especially those with diabetic ketoacidosis (DKA) and neutropenia.
- Caused by fungi like Rhizopus, Mucor, and Lichtheimia species.
- Histopathology reveals broad, non-septate hyphae with right-angle (90°) branching.
- Classic presentation is rhino-orbital-cerebral infection, often with a black necrotic eschar on the palate or nasal turbinates.
- Diagnosis requires biopsy for histology and culture.
- Treatment is emergent: aggressive surgical debridement and systemic amphotericin B.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

