Prophylactic Vaccines - Prevention Power-Up
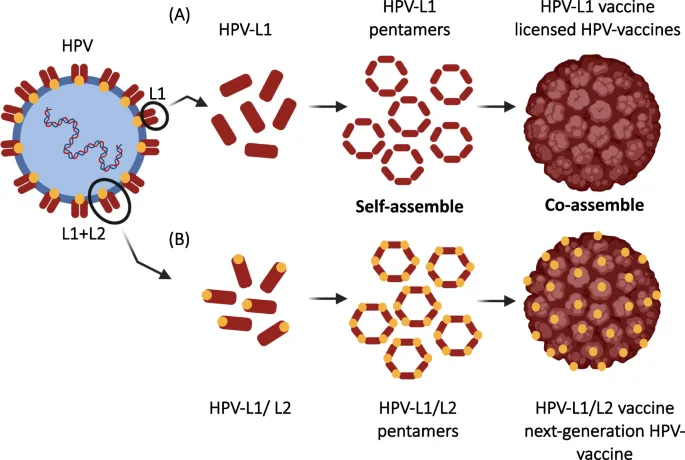
- Human Papillomavirus (HPV) Vaccine (e.g., Gardasil 9):
- Targets high-risk oncogenic types (16, 18, 31, 33, 45, 52, 58) & wart-causing types (6, 11).
- Prevents cervical, anogenital, and oropharyngeal cancers.
- Mechanism: Recombinant L1 capsid proteins form non-infectious Virus-Like Particles (VLPs), inducing potent neutralizing antibodies.
- Hepatitis B Virus (HBV) Vaccine:
- Crucial for preventing Hepatocellular Carcinoma (HCC).
- Mechanism: Contains recombinant Hepatitis B surface antigen (HBsAg) to stimulate protective anti-HBs antibodies.
⭐ The HPV vaccine is purely prophylactic; it prevents new infections but does not treat existing HPV or related neoplasia.
Antiviral Agents - Viral Eradication
-
Goal: Reduce viral load, prevent replication, and decrease cancer risk. Complete eradication is the aim but not always achieved.
-
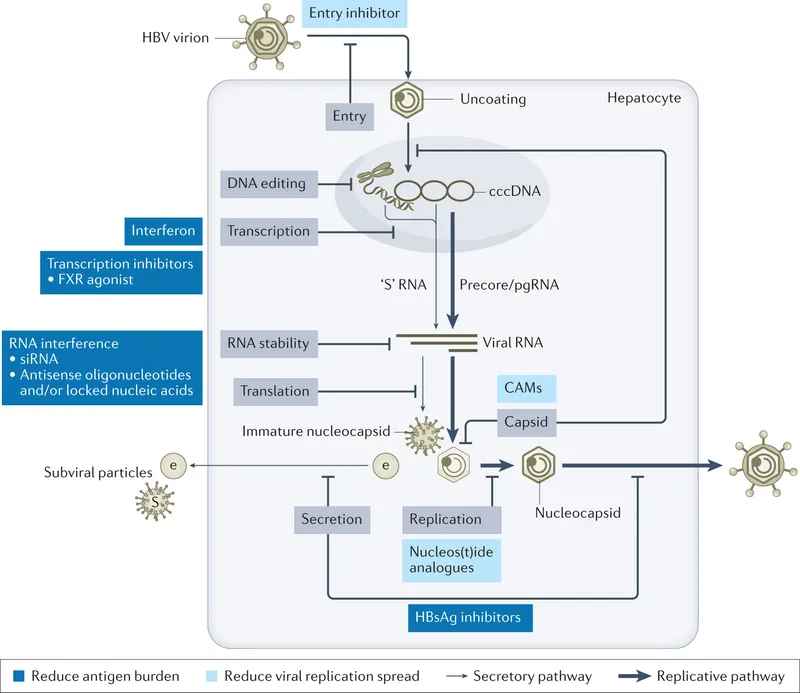
Hepatitis B Virus (HBV):
- Agents: Tenofovir, Entecavir (NRTIs).
- Mechanism: Inhibit viral reverse transcriptase.
- Outcome: Lifelong viral suppression, not a cure. Significantly lowers Hepatocellular Carcinoma (HCC) risk.
-
Hepatitis C Virus (HCV):
- Agents: Direct-Acting Antivirals (DAAs) like Sofosbuvir/Ledipasvir.
- Mechanism: Target specific viral proteins (e.g., NS5A/NS5B).
- Outcome: Cure rates >95% (Sustained Virologic Response).
-
HPV & EBV:
- No curative antiviral therapy for latent infection; management focuses on prevention (HPV vaccine) or treating lesions/cancer.
⭐ Sustained Virologic Response (SVR) after DAA therapy for HCV is considered a cure and is associated with a >70% reduction in HCC incidence.
Immunotherapy - Unleashing the Host
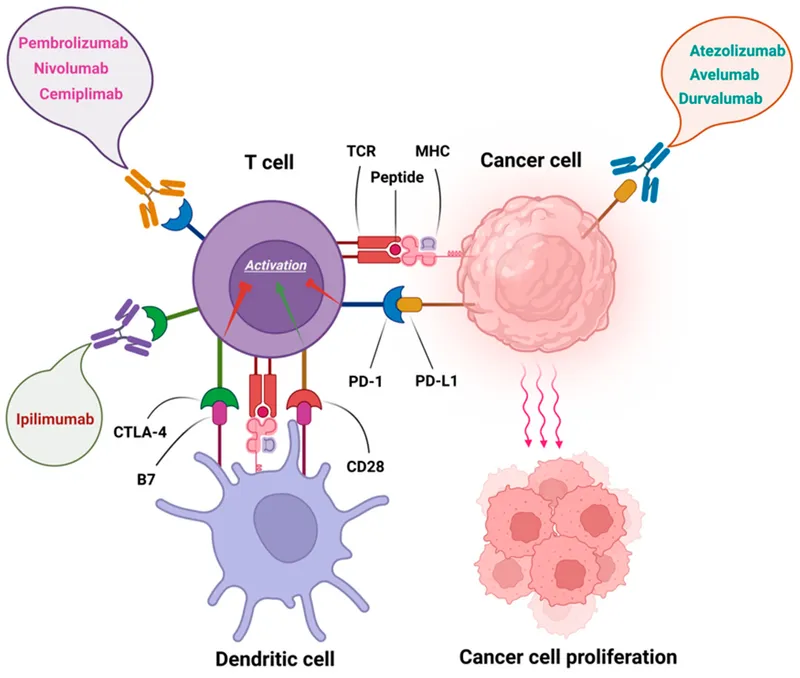
- Immune Checkpoint Inhibitors (ICIs): Reinvigorate exhausted T-cells to attack virus-infected tumor cells.
- PD-1/PD-L1 Inhibitors: Block the "off switch" on T-cells. Used in Merkel cell carcinoma (polyomavirus) & EBV-associated gastric cancer.
- Examples: Pembrolizumab, Nivolumab.
- CTLA-4 Inhibitors: Target another T-cell inhibitory receptor.
- Example: Ipilimumab.
- PD-1/PD-L1 Inhibitors: Block the "off switch" on T-cells. Used in Merkel cell carcinoma (polyomavirus) & EBV-associated gastric cancer.
- Therapeutic Vaccines: Stimulate a de novo T-cell response against viral antigens (e.g., HPV E6/E7 oncoproteins).
- Goal: Break immune tolerance to established infections and associated cancers.
- Adoptive Cell Therapy (CAR-T): Genetically engineer a patient's T-cells to express Chimeric Antigen Receptors (CARs) targeting viral antigens on tumor cells (e.g., EBV-positive lymphomas).
⭐ High-Yield: Many oncogenic viruses (e.g., EBV, KSHV) induce chronic inflammation and exploit the PD-1/PD-L1 pathway to cause T-cell exhaustion, hiding the tumor from the immune system. ICIs restore this lost surveillance.
Targeted Cellular Therapies - Hacking the Hijack
-
Concept: Genetically engineering a patient's own T-cells to specifically recognize and kill cancer cells expressing viral antigens. This offers high specificity, minimizing off-tumor effects.
-
Chimeric Antigen Receptor (CAR)-T Cells:
- Engineered to express synthetic receptors (CARs).
- Recognize viral proteins on the tumor cell surface (MHC-independent).
- Example: Targeting EBV's LMP1/LMP2 in nasopharyngeal carcinoma.
-
T-Cell Receptor (TCR)-T Cells:
- Engineered to express specific TCRs.
- Recognize processed viral peptides presented by MHC molecules.
- Can target intracellular antigens (e.g., HPV E6/E7, EBV EBNA1).
- MHC-restricted, requiring HLA matching.
⭐ High-Yield: Unlike conventional cancer antigens, viral antigens are truly tumor-specific. This makes therapies like CAR-T/TCR-T targeting viral proteins (e.g., HPV E6/E7) highly precise with a lower risk of attacking healthy host cells.
High‑Yield Points - ⚡ Biggest Takeaways
- Prophylactic vaccination is the primary prevention for cancers caused by HPV and HBV.
- Treating chronic HCV/HBV with antivirals lowers hepatocellular carcinoma risk.
- For EBV and KSHV, treatment targets the malignancy itself (e.g., lymphoma, sarcoma), not the latent virus.
- Immune checkpoint inhibitors are effective for cancers like Merkel cell carcinoma (MCPyV) and cervical cancer.
- Restoring immunity is crucial for Kaposi's sarcoma in HIV/AIDS.
- Screening (e.g., Pap smear) is key for early detection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

