The Core Problem - Why Bother Washing?
- Primary Vector: Healthcare workers' (HCWs) hands are the main vehicle for transmitting nosocomial pathogens between patients.
- Acquisition of Flora:
- Contact with patients or contaminated environmental surfaces leads to hand contamination.
- HCWs can acquire 100 to 1,000 colony-forming units (CFUs) of bacteria during "clean" activities (e.g., lifting a patient).
- Pathogen Survival: Organisms like S. aureus and Gram-negatives can survive on hands for hours if not properly cleaned.
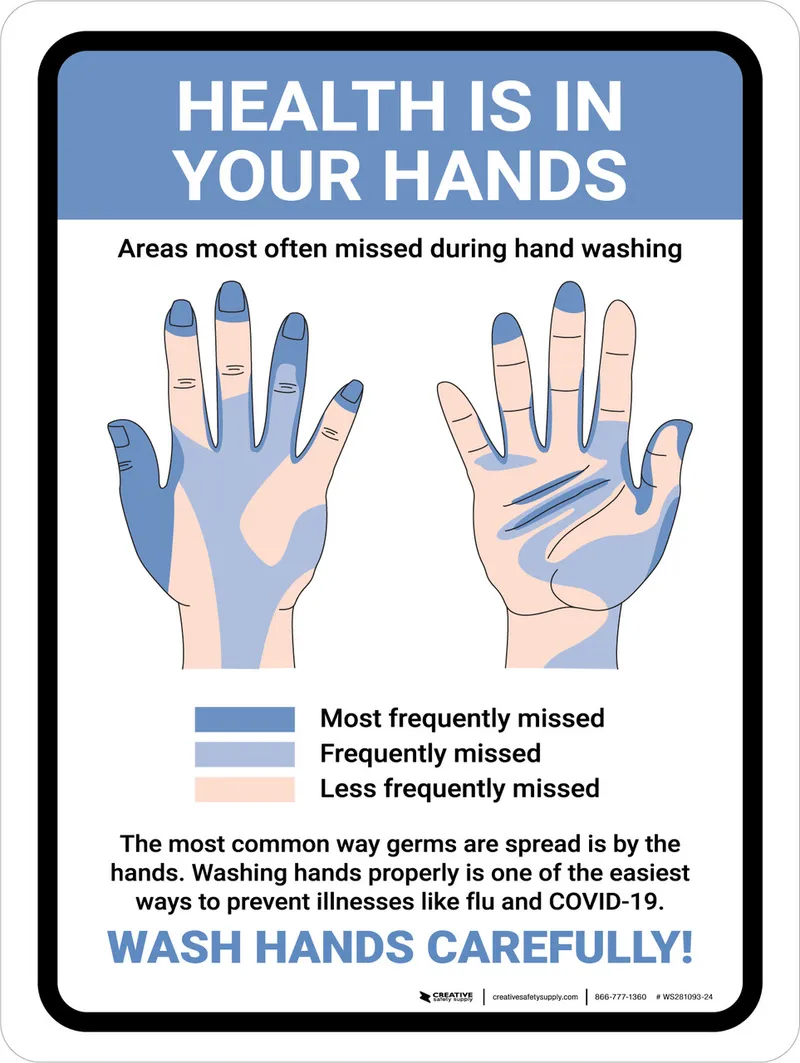
- Inadequate Cleansing: Pathogens are often missed in areas like fingernails, subungual spaces, and between fingers, leading to cross-contamination.
⭐ The skin under rings is more heavily colonized than other areas of the hand. Even after handwashing, rings can harbor pathogens, making their removal a key consideration in high-risk settings like operating rooms and ICUs.
The 5 Moments - Your Cues to Clean
A WHO framework to minimize pathogen transmission and reduce hospital-acquired infections (HAIs). Perform hand hygiene at these critical points to protect both patient and provider.
- 1. Before Touching a Patient: Prevents colonization of the patient with healthcare-associated microorganisms.
- 2. Before a Clean/Aseptic Procedure: Protects the patient against infection with harmful germs, including their own.
- 3. After Body Fluid Exposure Risk: Protects you from colonization or infection with patient's germs.
- 4. After Touching a Patient: Prevents transmission to the healthcare environment and other patients.
- 5. After Touching Patient Surroundings: Protects you and mitigates environmental contamination.

⭐ Exam Favorite: The most commonly missed areas during hand hygiene are the fingertips, thumbs, and interdigital spaces. This oversight is a frequent source of persistent bacterial contamination and transmission.
The Right Stuff - Suds vs. Sanitizer
-
Soap & Water (The Classic Scrub)
- Mechanism: Mechanical friction & detergent action (saponification) lifts dirt & microbes.
- Required When:
- Hands are visibly soiled.
- After restroom use / before eating.
- Contact with spore-forming organisms (e.g., Clostridioides difficile, Bacillus anthracis).
- Contact with certain parasites (e.g., Cryptosporidium).
-
Alcohol-Based Hand Rub (ABHR) (The Go-To Gel)
- Mechanism: Denatures proteins. Must contain 60-95% alcohol.
- Preferred For Most Clinical Encounters (if hands not visibly soiled).
- Advantages: Faster, more accessible, generally less dermatologically irritating than frequent soap/water washing.

⭐ Exam Favorite: ABHRs are ineffective against bacterial spores. After caring for a patient with C. difficile infection, hand washing with soap and water is mandatory to physically remove the spores.
Compliance Crashers - The Human Factor
- Perceived Barriers: High workload, skin irritation from agents, and inconveniently located sinks or sanitizers.
- Knowledge & Attitude: Forgetting, doubting the evidence, or lacking institutional safety culture and positive role models.
- Misconceptions: Believing gloves are a complete substitute for hand hygiene.
⭐ Glove use is not a substitute for hand hygiene; contamination of hands can occur during glove removal.
High‑Yield Points - ⚡ Biggest Takeaways
- Hand hygiene is the single most effective measure to prevent hospital-acquired infections (HAIs).
- Alcohol-based hand rubs (ABHRs) are preferred for most clinical situations, but do not kill spores.
- Soap and water are mandatory for visibly soiled hands and after contact with C. difficile or Norovirus.
- Low compliance among healthcare workers is a major driver of nosocomial outbreaks.
- Fingernails, especially artificial ones, are significant reservoirs for pathogens, compromising hygiene efficacy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

