Group B Strep - Baby's Big Foe
- Streptococcus agalactiae; β-hemolytic, bacitracin-resistant.
- Colonizes vagina & GIT; major risk is vertical transmission to neonate during birth.
- Neonatal Disease:
- Early-onset (<7 days): Sepsis, pneumonia, meningitis.
- Late-onset (>7 days): Meningitis, bacteremia.
- Screening: Universal rectovaginal culture for all pregnant women at 36-37 weeks gestation.
- Prophylaxis: Intrapartum penicillin G for positive screen or GBS risk factors (e.g., prolonged rupture of membranes >18 hrs, fever).
⭐ The CAMP test is a key identifier: GBS produces a diffusible protein (CAMP factor) that enhances the β-hemolysis of Staphylococcus aureus.

Clinical Punch - From Neonate to Nanna
- Neonates: Leading cause of early-onset sepsis & meningitis.
- Early-onset (<7 days): Pneumonia, sepsis, meningitis. Acquired in-utero or during delivery.
- Late-onset (7 days - 3 months): Bacteremia with meningitis is common.
- Pregnant Women:
- Usually asymptomatic carriers (vaginal/rectal colonization).
- Can cause chorioamnionitis, endometritis, or UTIs.
- 📌 Universal screening via rectovaginal culture at 36-37 weeks gestation.
- Non-pregnant Adults (esp. Elderly/Comorbid):
- Pneumonia, skin and soft tissue infections (cellulitis), bacteremia, and endocarditis.
- Associated with diabetes mellitus, malignancy, and other immunocompromised states.
⭐ Exam Favorite: Streptococcus agalactiae (GBS) is the most common cause of meningitis in neonates <1 month old.
Lab Sleuthing - Catching the Culprit
- Specimens: Vaginal/rectal swabs (35-37 weeks gestation), blood, CSF.
- Microscopy: Gram-positive cocci in chains.
- Culture: Narrow zone of β-hemolysis on blood agar.
- Key Tests: Catalase-negative, Bacitracin-resistant.
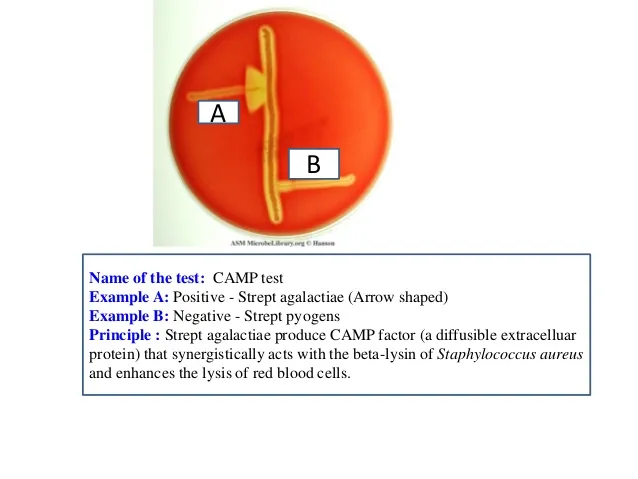
⭐ The CAMP test is a classic identifier. GBS produces a diffusible CAMP factor that enhances the β-hemolysis of Staphylococcus aureus, creating a distinct arrowhead-shaped zone of hemolysis.
📌 Bacitracin-resistant, Beta-hemolytic, Big-time Baby-killer.
Treatment & Shielding - Penicillin's Power Play
- Primary Treatment: IV Penicillin G is the drug of choice for maternal and neonatal GBS infections. Ampicillin is an alternative.
- Penicillin Allergy:
- Low-risk (e.g., rash): Cefazolin.
- High-risk (anaphylaxis): Clindamycin (if susceptible) or Vancomycin.
- Intrapartum Antibiotic Prophylaxis (IAP): Essential to prevent vertical transmission. Administer IV antibiotics ≥4 hours before delivery.
⭐ Intrapartum prophylaxis is highly effective at preventing early-onset (<7 days) neonatal GBS disease but does not prevent late-onset disease or eradicate maternal colonization.
- *Risk factors: Labor <37 wks, ROM ≥18 hrs, or intrapartum fever ≥38°C.

High‑Yield Points - ⚡ Biggest Takeaways
- Group B Strep (S. agalactiae) is a leading cause of neonatal meningitis, sepsis, and pneumonia.
- Transmission is typically vertical from the mother's colonized vagina during birth.
- Universal screening for pregnant women is performed at 35-37 weeks gestation.
- Intrapartum penicillin is the standard prophylaxis for colonized mothers or those with risk factors.
- Lab diagnosis: CAMP test positive, bacitracin-resistant, and positive for hippurate hydrolysis.
- The primary virulence factor is its polysaccharide capsule, which inhibits phagocytosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

