Overview - Branching Filamentous Foes
- Gram-positive, filamentous branching rods that resemble fungi but are true bacteria (prokaryotes).
- Actinomyces:
- Anaerobic
- Not acid-fast
- Normal oral, reproductive, and GI flora
- Nocardia:
- Aerobic
- Weakly acid-fast (mycolic acids)
- Found in soil
📌 Mnemonic: SNAP (Sulfur granules - Actinomyces; Nocardia - Aerobic, Pulmonary infections)
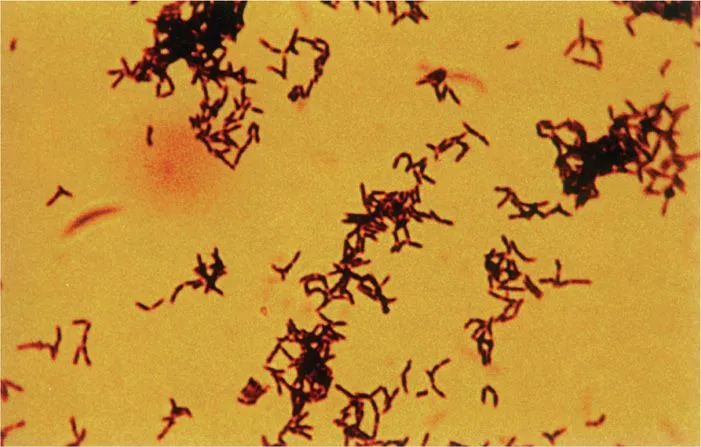
⭐ Both are bacteria that can be mistaken for fungi on microscopy due to their branching, filamentous morphology. Unlike fungi, they are prokaryotes and are sensitive to antibiotics (e.g., Penicillin for Actinomyces, TMP-SMX for Nocardia), not antifungals.
Actinomyces - Jaw-Dropping Granules
- Organism: Gram-positive, branching filamentous rod; strict anaerobe. Not acid-fast.
- Pathogenesis: Component of normal oral, GI, and vaginal flora. Infection arises from mucosal disruption (e.g., dental procedures, aspiration, IUDs).
- Spreads contiguously, ignoring tissue planes, forming hard, indurated masses.
- Leads to chronic, suppurative infections with draining sinus tracts.
- Clinical Features:
- Cervicofacial ("Lumpy Jaw"): Most common form; a firm, non-tender swelling at the angle of the jaw.
- Thoracic, abdominal, and pelvic (especially with IUDs) disease.
- Treatment: High-dose Penicillin G for a prolonged duration (weeks to months); surgical drainage is often required.
⭐ High-Yield: The hallmark of Actinomycosis is the formation of draining sinus tracts that exude pus containing yellow sulfur granules, which are macroscopic colonies of the bacteria.
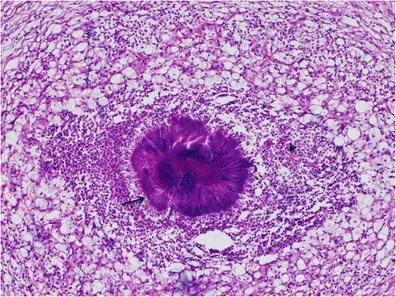
Nocardia - Acid-Fast Impostor
- Gram-positive, branching, filamentous rod found ubiquitously in soil.
- Aerobic and weakly acid-fast (resists decolorization with weak acid) → key distinction from Mycobacterium tuberculosis.
- Transmission: Primarily through inhalation (pulmonary) or direct skin inoculation (cutaneous).
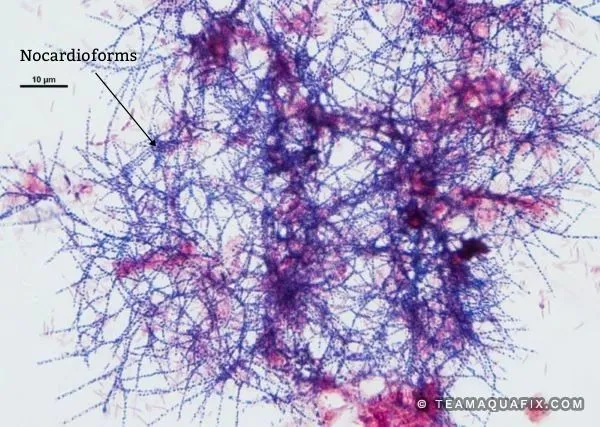
- High-Risk Groups: Immunocompromised patients (transplant recipients, chronic steroid use, HIV/AIDS).
- Clinical Manifestations:
- Pulmonary (most common): Pneumonia with cavitary lesions, mimicking TB.
- CNS: Brain abscesses are common with dissemination.
- Cutaneous: Cellulitis, subcutaneous abscesses, or mycetoma.
⭐ Treatment of choice is Trimethoprim-Sulfamethoxazole (TMP-SMX); therapy may be required for >6 months.
📌 Mnemonic (SNAP): Sulfonamides for Nocardia; Actinomyces use Penicillin.
Actinomyces vs. Nocardia - The Great Divide
| Feature | Actinomyces israelii | Nocardia asteroides |
|---|---|---|
| Morphology | G(+) branching filamentous rod | G(+) branching filamentous rod |
| Stain | Not Acid-Fast | Partially Acid-Fast |
| Oxygen | Obligate Anaerobe | Obligate Aerobe |
| Habitat | Normal oral/GI/GU flora | Found in soil |
| Pathology | Draining sinus tracts, sulfur granules | Pneumonia, brain/skin abscesses |
| Treatment | Penicillin G (high dose) | Sulfonamides (TMP-SMX) |
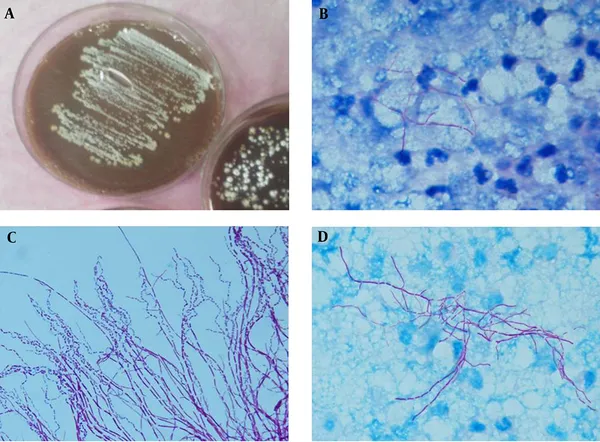
⭐ Exam Favorite: Both are filamentous bacteria, often mistaken for fungi. Nocardia primarily affects immunocompromised patients (HIV, transplant), while Actinomyces infection often follows local trauma (e.g., dental work).
- Actinomyces is an anaerobe and not acid-fast; Nocardia is an aerobe and partially acid-fast.
- Both are Gram-positive branching filamentous rods, mimicking fungi.
- Actinomyces classically causes cervicofacial infections with draining sinus tracts and yellow sulfur granules.
- Nocardia primarily causes pulmonary infections in the immunocompromised, which can disseminate to the brain.
- Treatment for Actinomyces is penicillin G; for Nocardia, it's sulfonamides (TMP-SMX).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

