Biofilm Formation - It Takes a Village
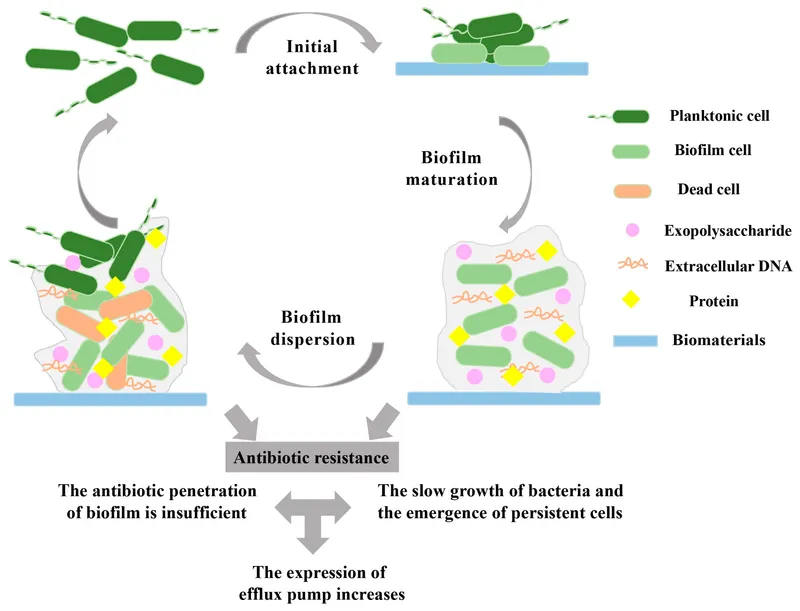
- Stage 1: Attachment
- Reversible adhesion of free-swimming (planktonic) bacteria to a surface (e.g., catheters, implants).
- Stage 2: Adhesion & Colonization
- Irreversible binding, followed by proliferation into protective microcolonies.
- Stage 3: EPS Production
- Secretion of an Extracellular Polymeric Substance (EPS) matrix-a protective slime of polysaccharides, proteins, and eDNA that confers antibiotic resistance.
- Stage 4: Maturation & Dispersal
- The biofilm matures; some bacteria detach to colonize new sites.
⭐ Quorum sensing orchestrates this entire process. Bacteria release signaling molecules (autoinducers); once a critical concentration is reached, it triggers coordinated gene expression for EPS production and virulence.
Pathogenesis & Resistance - The Fortress of Infection
- Physical Barrier (EPS Matrix):
- The slimy extracellular polymeric substance (EPS) matrix acts as a physical shield.
- Blocks host immune cells (↓ phagocytosis), antibodies, and complement activation.
- Mechanisms of Extreme Resistance:
- Limited Drug Penetration: The dense EPS matrix physically obstructs antibiotic diffusion.
- Slow Growth State: Bacteria in the biofilm's deeper layers have low metabolic activity, making them tolerant to antibiotics that target growth (e.g., β-lactams).
- Persister Cells: A subpopulation of dormant cells that are highly resistant to antibiotics; they can repopulate the biofilm after therapy ceases.
- Horizontal Gene Transfer: Close cell proximity facilitates the efficient exchange of resistance plasmids.
⭐ Biofilm-based infections may require antibiotic concentrations 100-1000 times higher than the standard Minimum Inhibitory Concentration (MIC) to be effective.
Clinical Examples - The Usual Suspects
- Pseudomonas aeruginosa: Classic cause of chronic pneumonia in Cystic Fibrosis. Its mucoid alginate exopolysaccharide creates a protective biofilm in the airways.
- Staphylococcus epidermidis: The most common cause of infections on indwelling medical devices like catheters, prosthetic heart valves, and artificial joints.
- Staphylococcus aureus: A key agent in chronic osteomyelitis, endocarditis, and persistent wound infections. Biofilm protects it from host defenses and antibiotics.
- Viridans Group Streptococci (S. mutans): Primary colonizers of dental surfaces, forming plaque that leads to dental caries and gingivitis. Can seed and cause subacute native valve endocarditis.
- Non-typeable Haemophilus influenzae: A frequent cause of recurrent otitis media in children, forming biofilms in the middle ear.
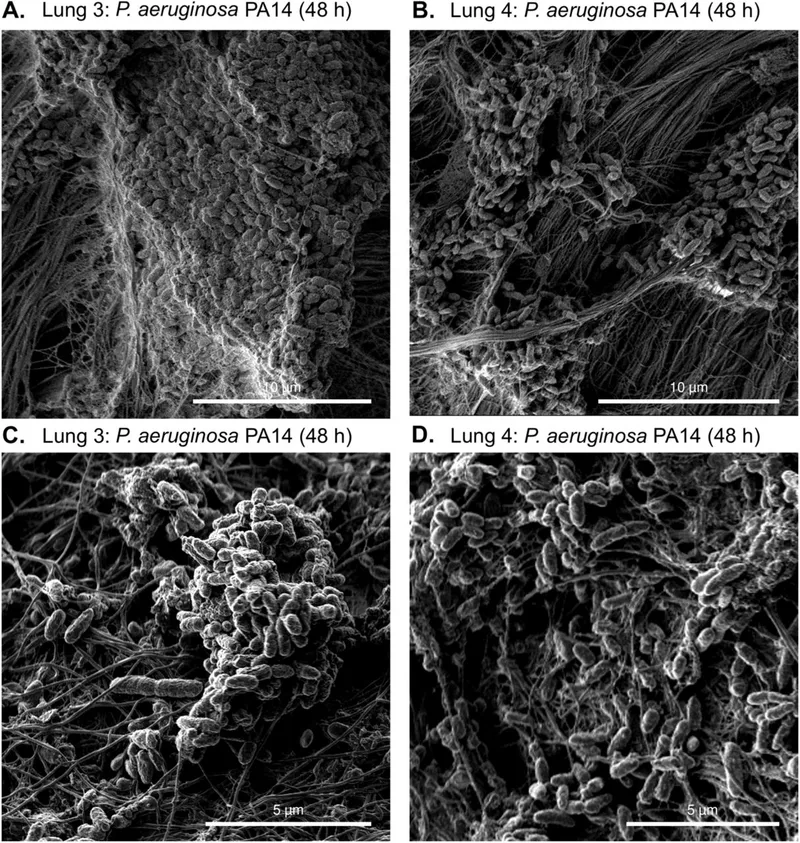
⭐ The quorum-sensing system in P. aeruginosa coordinates the expression of virulence factors and biofilm formation, making it a prime target for novel anti-biofilm therapies.
High‑Yield Points - ⚡ Biggest Takeaways
- Biofilms are microbial communities encased in a self-produced extracellular polymeric substance (EPS), shielding them from threats.
- This matrix confers high resistance to antibiotics and host immune responses, causing chronic, persistent infections.
- Key examples: P. aeruginosa in cystic fibrosis lungs, S. epidermidis on catheters, and dental plaque.
- Quorum sensing is the cell-to-cell communication system that regulates biofilm formation.
- Treatment often requires physical removal of the biofilm source (e.g., infected device).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

