Neurological Issues - Brain Under Siege
-
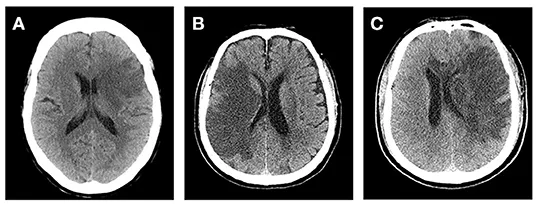
Cerebral Edema & ↑ Intracranial Pressure (ICP)
- Pathophysiology: Cytotoxic edema peaks 3-5 days post-infarct, leading to mass effect.
- Clinical Signs: Deteriorating consciousness, new focal deficits, Cushing's triad.
- Management: Follows a tiered approach to lower ICP and improve cerebral perfusion.
-
Seizures
- Incidence: ~5% of patients; can be early (<1 week) or late (>1 week).
- Acute Management: Benzodiazepines (e.g., Lorazepam).
- Prevention: Prophylaxis is not routine. Start an AED (e.g., Levetiracetam) after a first seizure.
-
Hemorrhagic Transformation
- Ischemic tissue converts into a hemorrhage.
- Major risk factors: Large infarct size, thrombolysis (tPA), anticoagulation.
- Action: Immediately stop offending agents; urgent neurosurgical evaluation.
⭐ Malignant MCA Syndrome: A devastating complication in large MCA strokes with massive edema. Decompressive hemicraniectomy within 48 hours of stroke onset is life-saving and improves outcomes in patients <60 years.
Systemic Crises - Body-Wide Breakdown
- Hypertension: A critical balancing act.
- Ischemic Stroke: Allow "permissive hypertension" (up to 220/120 mmHg) to maintain cerebral perfusion. If thrombolysis (tPA) was administered, strictly maintain BP < 185/110 mmHg to prevent hemorrhagic conversion.
- Hemorrhagic Stroke: Aggressively lower systolic BP, with a common target of < 140 mmHg.
- Hyperglycemia: Stress-induced state that worsens neurologic outcomes. Target glucose range is 140-180 mg/dL using insulin; avoid hypoglycemia.
- Fever: Increases metabolic demand and exacerbates neuronal injury. Treat promptly with antipyretics while investigating underlying infections (e.g., aspiration pneumonia, UTI).
- VTE Prophylaxis: For all immobile patients.
⭐ Post-stroke cardiac monitoring is vital. Strokes involving the insular cortex are particularly associated with dangerous arrhythmias (like AFib) and even Takotsubo cardiomyopathy.
Rehabilitation Phase - Rebuilding Life
- Goal: Maximize functional independence and quality of life through a multidisciplinary team (PT, OT, SLP).
- Physical Therapy (PT):
- Focuses on mobility, strength, balance, and gait training.
- Prevents complications like joint contractures and deep vein thrombosis (DVT).
- Occupational Therapy (OT):
- Aids in regaining Activities of Daily Living (ADLs) like dressing, bathing, and eating.
- Involves adaptive strategies and equipment.
- Speech-Language Pathology (SLP):
- Addresses aphasia (language deficits), dysarthria (slurred speech), and dysphagia (swallowing difficulty).
- Crucial for preventing aspiration pneumonia.
- Spasticity Management: Treat with physical modalities first, then consider baclofen, tizanidine, or botulinum toxin for focal spasticity.
- Post-Stroke Depression: Common; screen and treat with SSRIs to improve participation and outcomes.

⭐ Constraint-Induced Movement Therapy (CIMT): An OT technique involving restraining the unaffected limb to force the use of the weaker, affected limb, promoting neuroplasticity and functional recovery.
High-Yield Points - ⚡ Biggest Takeaways
- Cerebral edema is a peak cause of mortality 3-5 days post-stroke; manage with hyperosmolar therapy (mannitol, hypertonic saline).
- Suspect hemorrhagic transformation with neurologic worsening after tPA; get an immediate non-contrast CT.
- Prophylactic anticonvulsants are not indicated; treat seizures only when they occur.
- Prevent DVT/PE with early mobilization and subcutaneous heparin/LMWH once hemorrhage is ruled out.
- Keep patients NPO until a formal swallowing study clears them to prevent aspiration pneumonia.
- Post-stroke depression is common; screen and treat with SSRIs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

